ABRUPTIO PLACENTA-AN OBSTETRIC
ENDANGERMENT
Dissertation submitted to
THE TAMILNADU DR. M.G.R. MEDICAL
UNIVERSITY
In partial fulfillment of the regulations
For the award of the degree of
M.S. BRANCH-II
OBSTETRICS AND GYNECOLOGY
KILPAUK MEDICAL COLLEGE
CHENNAI
CERTIFICATE
This is to certify that the dissertation entitled “
Abruptio placenta-an
obstetric endangerment.”
is a bonafide record of work done by
Dr.SWETHA.S
in Kilpauk Medical college, Chennai during the
period January 2018 to August 2018 under the guidance of
Prof.Dr.K.L.MALARVIZHI.,MD.,DGO.,DNB
HOD &Professor
of Obstetrics and Gynaecology,Government Kilpauk Medical
College in partial fulfilment of requirement of MS degree in
Obstetrics and Gynaecology degree examination of The Tamilnadu
Dr. M.G.R Medical University to be held in May 2019.
Dr.P.VASANTHAMANI MD.,DGO.,MNAMS.,DCPSY.,MBA Dean
Government Kilpauk Medical College& Hospital,
Chennai – 600 010
Dr.K.L.MALARVIZHI MD.,DGO.,DNB
Prof & HOD,Dept. Of Obstertrics & Gynaecology
Government Kilpauk Medical College& Hospital,
DECLARATION
I Dr.SWETHA.S, Post graduate, Department of Obstetrics and
Gynaecology,Government Kilpauk Medical college, solemnly declare
that this dissertation entitled“Abruptio Placenta-an obstetric
endangerment” was done by me at Government Kilpauk Medical College
during 2016-2019 under the guidance and supervision of
Prof.Dr.K.L.MALARVIZHI.,MD.,DGO.,DNB,Professor&Head,
Department of Obstetrics and Gynaecology,Government Kilpauk
Medical College. This dissertation is submitted to the Tamil Nadu
Dr. M.G.R. Medical University towards the partial fulfilment of
requirements for the award of M.S. Degree in Obstetrics and
Gynaecology (Branch-II).
Place: Chennai-10
Date: Dr.SWETHA.S,
Postgraduate student
Dept. Of Obstetrics & Gynaecology Govt. Kilpauk Medical College Chennai-10
Prof.DR.K.L.MALARVIZHI,MD.,DGO.,DNB
Professor&HOD
Dept.of Obstetrics and Gynaecology Guide
ACKNOWLEDGEMENT
I am thankful to our Dean , Dr.P.VASANTHAMANI, MD.,DGO.,MNAMS.,
DCPSY, MBA,Government Kilpauk Medical College, Chennai for allowing
me to conduct the study and use the facilities and clinical materials available
in the hospital.
It is my greatest pleasure to express my gratitude and thank
Prof.Dr.K.L.MALARVIZHI,MD.,D.G.O.,DNB,Professor&Head,
Department of Obstetrics and Gynaecology,Government Kilpauk Medical
College& Hospital for her valuable guidance, interest, encouragement and the
constructive ideas which she provided for this study.
I take this opportunity to express my deep sense of gratitude and humble
regards to my beloved teacher Prof.Dr.S.USHARANI,M.D.,DGO.,DNB for
being a constant source of inspiration and support.
I thank all my other Professors,Assistant Professors and paramedical Staffs of
this Department of Obstetrics and Gynaceology, Kilpauk Medical College,
Chennai-600010,without whom this would not have been possible.
I sincerely thank Dr.Padmanabhan,PhD, for his constant support during this
study and for his help in the statistical analysis of data and results.
I would like to thank all my fellow post graduates for helping me accomplish
I sincerely thank all my patients for their cooperation .
Last, but not the least,I thank my family and God Almighty for the blessings
showered onto me.
CONTENTS
1.
INTRODUCTION
1
2.
AIMS OF STUDY
3
3.
REVIEW OF LITERATURE
4
4.
MATERIALS AND METHODS
38
5.
RESULTS & DISCUSSION
40
6.
SUMMARY
76
7.
CONCLUSION
79
8.
BIBLIOGRAPHY
80
Page | 1 INTRODUCTION
• Abruptio placentae is the premature separation of a normally implanted placenta from the uterus, usually after 20 wk gestation.
• The Royal College of Obstetricians and Gynaecologists (RCOG) defines antepartum haemorrhage (APH) as bleeding from or in to the
genital tract after 24+0 weeks till the birth of the baby, and recognizes
abruptio placenta (AP) as an important cause of APH.
• It can be an obstetric emergency as it can be a cause of maternal and fetal mortality and morbidity.
• 50 patients admitted with clinical presentation of abruptio placenta – vaginal bleeding, pain abdomen or uterine tenderness after 24 weeks of
gestation (gestational age from dating scan was considered ) were
included in the study and the diagnosis of abruptio placenta was
confirmed later on by placental examination.
• All the patients in the study population were clinically evaluated and worked up immediately with ultrasonogram,complete hemogram,renal
function test,liver function test, serum electrolytes and coagulation
profile and followed up for 4 weeks.
• Maternal outcome like shock,post partum hemorrhage,acute renal failure, need for mechanical ventilation,Disseminated Intra Vascular
Page | 2
• The fetal/neonatal outcome like intrauterine demise, birth weights, and an Apgar score at 1 min and 5 min were recorded and compared.
• The abruption – delivery interval will be correlated with the maternal and perinatal outcome.
• The data obtained from this study would help in improving maternal and fetal morbidity and mortality by planning appropriate and timely
Page | 3 AIMS AND OBJECTIVES
AIMS :
To study the maternal and perinatal outcomes of abruptio placenta in the
Department of Obstetrics and Gynaecology ,KMCH and to see if early
intervention reduces the perinatal mortality and morbidity,thereby improving
the maternal-fetal outcome.
OBJECTIVES:
1)To assess the maternal outcome in the form of maternal mortality/ morbidity.
2)To assess the perinatal outcome in the form of APGAR,Birth
weight&perinatal mortality/morbidity.
3) To discuss future management options and see if early intervention has a
Page | 4 REVIEW OF LITERATURE
NORMAL PLACENTATION
• The placenta is a remarkable organ performing many diverse functions including transport of gases and metabolites, immunological protection
and production of steroid and protein hormones.
• The zygote after repeated mitotic divisions gets converted in to a blastocyst.The outer layer of the blastocyst is known as the trophoblast
and the inner cell mass is known as the embryoblast.
• The blastocyst after getting embedded into the endometrium, the trophoblast rapidly proliferates and differentiates into an outer
syncitiotrophoblast and an inner cytotrophoblast.
• The primary, secondary and tertiary villi are formed by the syncitiotrophoblasts and the intervillous space is formed by the
cytotrophoblasts.
• Until the end of sixteenth week the placenta grows in thickness and circumference due to the growth of the chorionic villi and expansion of
the inter-villous space.
• After that there is little increase in thickness but it increases circumferentially until term.
Page | 5
Page | 6 DEFINITION OF ABRUPTIO PLACENTAE
• The Royal College of Obstetricians and Gynaecologists (RCOG) defines antepartum haemorrhage (APH) as bleeding from or in to the
genital tract after 24+0 weeks till the birth of the baby.
• According to FOGSI , APH is bleeding occurring beyond 20 weeks of gestation prior to the onset of labour.
CAUSES OF APH
OBSTETRIC CAUSES NON OBSTETRIC CAUSES
Placenta previa Cervical polyp
Abruptio placenta Cervicitis,Cervical ectropion
Vasa previa Cervical or vaginal malignancies
Excessive show Cervical or vaginal lacerations
Uterine rupture Coagulation defects
• Placenta previa and Abruption constitute about 50% of APH. • Placental abruption is defined as complete or partial separation of
Page | 7
• It can present anytime after the 20 week of gestation till term either as an ante-partum or an intra-partum event.
• Abruptio placenta is known by several names such as accidental haemorrhage, ablation placenta and premature separation of placenta.
• AP is classified into concealed and revealed types. In concealed type the blood collects behind the placenta and there is no evidence of
vaginal bleed whereas in the revealed variety the blood tracks down
between the membranes and the uterine wall to present through the
vagina.
• The primary cause of Abruptio Placenta in majority of the cases
remains unknown but the RCOG recognizes hypertensive disorders of
pregnancy(previously called as pregnancy induced hypertension ),
advanced maternal age, multiparity, premature rupture of membranes
(PROM), smoking, polyhydramnios, abdominal trauma, fetal growth
restriction, intrauterine infections and past history of abruption as
predisposing risk factors.
HISTORICAL PERSPECTIVE OF ABRUPTIO PLACENTA
• In Latin, abruption placenta means “rending asunder of the placenta” which means separation or splitting of the placenta.
Page | 8
• The term accidental haemorrhage was 1st introduced by Rigby in the year 1776. He was the one who differentiated between placenta previa
and placental abrution.Hence, he called abrutio placenta an accidental
hemorrhage.
• DeLee and Coole coined the term ABRUPTIO PLACENTAE in the year 1848 to denote sudden separation of placenta from its normal
attachment site.
EPIDEMIOLOGY OF ABRUPTIO PLACENTA
• The incidence is up to 1.5% in overall pregnancies and 0.3% in pregnancies at term.
• 14% abruptions occur before 32 weeks of gestation.
• Incidence of abruptio placenta in India varies anywhere between 1:50 to 1:500.This wide variation is because of various modes of presentation
and the inaccurate documentation. It may be a very asymptomatic case
where the diagnosis is retrospectively done by the presence of a
retro-placental clot after delivery (4.5%) or a classical case presenting with
sudden painful bout of bleeding or collapse of a pregnant woman
associated with either overt or covert bleeding along with fetal
compromise.
• The perinatal mortality rate is approximately 20-fold higher in comparison to pregnancies without abruption (12 percent versus 0.6
Page | 9
• The majority of perinatal deaths (up to 77 percent) occur in utero; deaths in the postnatal period are primarily related to preterm delivery.
• A very high index of clinical suspicion is required to diagnose a case of placental abruption.
BASIC PATHOLOGY INVOLVED IN ABRUPTIO PLACENTA
• The very first event that is thought to occur is the formation of a retro-placental clot.
• But the event that triggers this clot formation is a matter of question . • It was postulated that there was an uterine spasm/contraction followed
by relaxation which lead on to venous engorgement that in turn
triggered the rupture of arterioles,which lead to bleeding into the
deciduas basalis.
• This blood can either get collected and form a clot behind the
placenta(concealed) or can dissect between the fetal membranes and
decidua,leading on to a vaginal bleeding(revealed).
• Or, it may disrupt the membranes and enter into the amniotic
cavity,which presents as a blood stained liquor or a port-wine colored
liquor.
• In more severe instances,it may extravasate into the myometrium, reaches the serosa and may cause bleeding into the peritoneum –a
condition which is known as COUVEILAIRE UTERUS OR
Page | 10
• The bleed may be small and self-limited, or may continue to dissect through the placental-decidual interface, leading to complete or near
complete placental separation.
• The detached portion of the placenta is unable to exchange gases and nutrients; when the remaining fetoplacental unit is unable to
compensate for this loss of function, the fetus becomes compromised.
• From the diagnostic standpoint, abruption placenta is diagnosed by the classical triad of : abdominal pain of sudden onset, vaginal bleeding and
a tense,tender uterus.
• It may just be asymptomatic in the early stages or may present with deadly complications like maternal collapse or fetal distress or even an
intrauterine fetal demise.
RISK FACTORS FOR ABRUPTIO PLACENTA
1)MATERNAL AGE:
The incidence of abruption increases with maternal age.Maternal age >35 yrs
and < 18 yrs is a significant risk factor. In the FASTER TRIAL-First and
Second Trimester Evaluation of Risk trial, women who were older than 40
years of age were 2.3 times at an increased risk of developing abruption than
those who were 35 years or younger. In another study,there is an increased
incidence with maternal age and patients who are over 35 years are twice as
Page | 11
The risk of abruptio placentae for women over the age of 35 years was 2.2
times the risk for women aged 19-34 years.
2)PARITY:
A study by Pritchard and colleagues (1991) reported that the incidence of
abruption is higher in women with increased parity.In another study, Toohey
and associates (1995) did not find this association.
But overall, majority of the studies report the incidence of abruption to be
higher in multiparous women.
3)HYPERTENSIVE DISORDERS OF PREGNANCY:
The most common condition associated with abruption seems to be some form
of hypertension (gestational hypertension, chronic hypertension,
preeclampsia).
Hypertensive disorders of pregnancy(mainly gestational hypertension and pre
eclampsia) is associated with 2.1-4% of the abruption cases whereas chronic
hypertension is associated with 1.8-3% of abruptions.(Sibai and coworkers in
1998).
Ananth and associates in2007 reported a 2.4fold increase in the incidence of
placental abruption with chronic hypertension and this incidence was further
Page | 12
4)NUTRITION AND ANEMIA:
Folic acid deficiency is one of the important factors in the etiology of
abruptio placentae. The possible mechanism between folic acid deficiency and
development of abruption is proved by bone marrow biopsy studies showing
megaloblastic erythropoiesis.
5)PREMATURE RUPTURE OF MEMBRANES:
There is an increased occurence of placental abruption in patients with
premature rupture of membranes,especially if duration was >24hours. The
incidence was 13% when premature rupture of membranes occured between
gestational age 29-32 weeks.
Histological chorioamnionitis is associated with increased incidence of
placental abruption and this association is dependent on its severity of
chorioamnionitis.
6)SMOKING AND COCAINE ABUSE:
Smoking tends to increase the overall risk of abruption placentae. According to
the results of a prospective cohort study the increase in incidence is by 40% for
Page | 13
The rate of abruption has been reported to be about 13-35% in patients who
use cocaine and the effect seems to be dose dependent.
7)BLUNT ABDOMINAL TRAUMA:
The incidence of abruption in blunt abdominal trauma is somewhere between
1.5-9.4%.Blunt abdominal trauma or rapid decompression of uterus may result
in shearing of placenta due to the sudden stretching or contraction of the
uterine wall. Maternal trauma has been associated with a six fold increase in
the risk of abruption.
8)EXTERNAL CEPHALIC VERSION:
External cephalic version is not a very popular common practice
Page | 14
complication of ECV, especially when the version was performed under
anaesthesia.
The incidence of abruption is said to be 2 to 9 % according to one study
9)THROMBOPHILIAS:
The association between placental abruption and the maternal thrombophilias
supports the fact that abruption is a final acute clinical presentation of a
chronic placental disease.
10)MULTIPLE PREGNANCY
The risk of placental abruption is increased 2-3 times in multi fetal gestations
and in such patients , subsequently the risk of preterm delivery tends to be on
the higher side and there by adding to the perinatal mortality and morbidity.
In multiple pregnancies there can be a sudden decompression and abruption
after delivery of the first baby.
11)PLACENTA PREVIA:
About 10% women with placenta previa may have placenta previa
concurrently. The bleeding from the placenta previa may collect behind the
placenta and may trigger further separation of the placenta,causing abruption.
12)ABRUPTIO PLACENTA IN PREVIOUS PREGNANCY
Recuurence of severe abruption was noted in about 1 in 8 cases by a study by
Page | 15
13)INVASIVE PROCEDURES:
Invasive procedures like amniocentesis can cause bleeding from the puncture
site which may collect behind the placenta and trigger abruption.
14)OTHERS:
• First trimester ultrasound examination showing a subchorionic or retroplacental haematoma increases the subsequent risk of placental
abruption by 6-7 fold.
• Uterine tachysystole (> 5 contractions in a 10 minute period) can cause abruption.
• Unexplained elevation of plasma alpha feto protein is associated with a 5% increase in the incidence of abruption.
• When the membranes rupture as in the case of polyhydramnios there is sudden decompression of the uterus which leads to the reduction in
uterine volume and a corresponding loss of surface area and as a result
the placenta sheers off.
• Uterine malformations may lead to poor decidualisation and placentation. The contractility of a malformed uterus may lead to
uncoordinated uterine action resulting in increased risk of placental
Page | 16
RECURRENCE OF ABRUPTION IN SUBSEQUENT PREGNANCIES.
• An antenatal woman with a history of abruptio placentae in previous pregnancy should be monitored with caution.
• The incidence of recurrent abruption was quite high ,approximately a 20-fold to 30-fold increased chances of abruption in subsequent
pregnancies when the previous pregnancy was complicated by placental
abruption.
PATHOLOGY IN ABRUPTIO PLACENTA
GROSS
• The hallmark of clinical diagnosis of placental abruption is the presence of retroplacental clots or any adherent clots or hematoma or
hemorrhage of variable size into the placenta or membranes with or
Page | 17
• The retroplacental clots are usually dark, firm, and adherent when compared to the red, soft, non adherent clots formed during physiologic
placental separation which occurs in the third stage of labor.
MICROSCOPIC
• Upon microscopic examination of the placenta & the uterus in cases where it has been removed, there were variable structural changes in the
decidua basalis, muscularis of the uterus, chorionic plate; and the
intervillous architecture.
• In low risk pregnancy, the spiral arteries of the uterus will undergo a transformation from the high resistance muscular arterioles to
low-resistance capacitance vessels.
• Such changes occur due to trophoblastic invasion which occurs in 2 spells, the first (10–16 weeks) and second (16–20 weeks) trimesters.
• In patients with placental abruption, however,the microscopic pathological changes in the placental bed show a high incidence of
vascular abnormalities with the most common finding (60%) being the
absence of any evidence of the physiologic transformation of
uteroplacental arteries.
Page | 18
• These abnormal placental vessels are prone to ischemia and rupture of involved vessels, there by causing placental abruption.
• Evidence of vasculopathy may be seen in the placental vessels- such as atherosis, narrowing of vessels, necrosis, and thrombosis.
• Vessels deep in the myometrium may show changes like vessel
occlusion with surrounding myometrial hemorrhage, which are seen in
about 33% of the cases.
• Decidual hematomas, thrombosis of the vessels, and focal necrosis are common, together with recent infarcts and these changes may be
extensive enough to involve large areas of the chorionic plate.
• Congestion of the capillaries in the chorionic villi is often present. Placental abruption usually develops simultaneously with placental
infarction, which is also a major risk factor for fetal or neonatal death.
• Placental infarcts are predominantly caused by spiral artery occlusion in the myometrium or decidua.
Page | 19
Extensive hemorrhage at the top of the image, at the decidual plate, with
placental villi below.(microscopic image of abruption placenta)
TYPES OF ABRUPTIO PLACENTA:
There are two major types of placental abruption:
1) The concealed variety: where the blood gets accumulated behind the
placenta and is not evident outside- may be partial or complete.
2) The revealed variety: where the blood tracks between membranes and
Page | 20
CLASSIFICATION OF ABRUPTIO PLACENTA:
PAGE CLASSIFICATION:
CLASS MATERNAL FETAL
0 asymptomatic,discovered retrospectively
after delivery
usually none
1 Mild/no vaginal bleeding
Uterine tenderness
Maternal vitals are stable
Usually none
2 Moderate vaginal bleeding
Moderate to severe uterine contractions,
titanic contractions
Maternal tachycardia
Fetal distress
Fetal bradycardia
3 Severe vaginal bleeding
Tetanic uterine contractions
Maternal shock
Coagulopathy
Page | 21
SHER & STUDLAND(1985) CLASSIFICATION
CLASS 1- clinically not recognized until delivery.
CLASS 2- the classical signs of abruption is present but the fetus is still alive
CLASS 3- Severe-the fetus is dead
A) Without coagulopathy
B) With coagulopathy
DIAGNOSIS
• Abruptio placenta most commonly present with the classical triad of abdominal pain, abnormal uterine tenderness and vaginal bleeding
after 20 weeks of gestation.
• However, pain abdomen may be present in only upto 50% of cases and it is most probably caused due to the hypertonic contractions or
extravasation of blood into the myometrium and it is said that
abruption placenta of a posteriorly situated placenta does not usually
present with pain.
• The classical clinical hallmark of abruption placenta is bleeding per vaginum ,which may be present in about 80% to 90% of cases.
Page | 22
• One study involving 198 women with a diagnosis of placental abruption determined that the most common manifestations in their
frequency of occurrence were:
Bleeding per vaginum (70%)
Abdominal pain (50%)
Blood stained amniotic fluid (50%)
Fetal heart rate abnormalities (69%).
• It is also important to note that in 19% of cases, there was neither bleeding nor pain . Hence,it is important to keep in mind that these
signs and symptoms are not always present and the absence of such
symptoms cannot exclude the diagnosis of an abruption.
• The presentation of the various above mentioned symptoms and their severity is directly related to the magnitude of placental separation.
• The 1st symptom may be a sudden onset, sharp and severe pain that
either persists or becomes a poorly localized,dull aching pain in the
lower abdomen and/or sacral areas.
• The uterus usually does not relax completely in between contractions,otherwise called as a tense uterus.
• The occurrence of high-frequency low-amplitude contractions and an increased baseline uterine tone often is seen in those with placental
abruption.
Page | 23
10% of the idiopathic preterm labor cases may be caused by concealed
abruptio placentae and about 60% of the placental abruption cases is
associated with preterm labor.
DIFFERENTIAL DIAGNOSIS OF CONCEALED/MIXED ABRUPTION
Preterm labor
Torsion ovarian cyst
Red degeneration of fibroid
Rupture uterus
Acute hydramnios
FINDINGS THAT FAVOR DIAGNOSIS OF ABRUPTION:
1. level of shock that is out of proportion to the amount of external bleeding.
2. Unexplained anemia and a tense uterus.
3. Association with severe pre eclampsia.
4. uterus might be tense and tender .
5. absent fetal heart rate
6. reduced urine output/oliguria
Page | 24 IMAGING IN ABRUPTIO PLACENTA
Historically,ultrasonogram has been a little less helpful in the diagnosis of
placental abruption, with the classical sonographic evidence being rarely seen
or has been difficult to identify.
As a result, the role of sonographic diagnosis in abruptio placentae classically
has been used as a diagnosis of exclusion when the ultrasound has failed to
show the presence of a placenta previa and after ruling out other causes of
vaginal bleeding .
The detection rate of abruptio placenta in ultrasound is somewhere between
5% to 50%.
Only a few patients with the clinical evidence of placental separation have
displayed the classic ultrasound abnormalities of a retroplacental hypoechoic
area or the dissection of blood between the fetal membranes when there is
fresh blood collected in the retroplacental area.
Once an haematoma appears,it is hyperechoic to isoechoic when compared to
the normal placenta and resolution the haematoma again becomes hypoechoic
within 1 week and sonoluscent within 2 weeks.
In recent times,because of the advances in ultrasound resolution, imaging, and
interpretation, there is an improvement in the diagnostic accuracy of targeted
Page | 25
vaginal bleeding. The ultrasound examination is aimed for the following 7
sonographic features which points towards abruption:
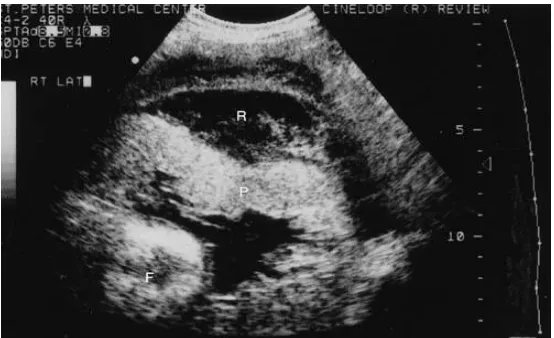
1. Preplacental collection.,under the chorionic plate (between placenta
[image:31.612.152.412.161.353.2]and amniotic fluid) (Fig.1)
Fig.1. pre placental collection P-placenta, C- collection
2. JELLO sign.: The placenta will show a jello like movement or jiggle
when sudden pressure is applied with the transducer probe
3. Retro placental collection (between the placenta and the myometrium)
(Fig. 2)
[image:31.612.150.427.515.684.2]Page | 26
4. Marginal collection (at the placental margin) (Fig. 3)
(fig 3) Sonographic blood collection at the placental margin (arrow). P,
placenta.
5. Subchorionic membranous collection (between the membranes and the
uterine wall) (Fig. 4)
(fig 4) subchorionic membranous collection between the placental
membranes and the uterine wall on ultrasound. S, subchorionic
Page | 27
6. Increased placental thickness or echogenicities (defined as thickness
greater than 4 cm perpendicular to the plane of the placenta (Fig.5)
(Fig 5)showing a thickened placenta with heterogenic foci,later
macroscopically confirmed to be an abruption.
7. Intra-amniotic hematoma or collection within the amniotic fluid) (Fig.
[image:33.612.152.384.91.268.2]6).
Page | 28 CARDIOTOCOGRAPHY IN ABRUPTIO PLACENTA
According to RCOG, there was some sort of a CTG abnormality in
about 69% of the cases of placental abruption.
Hence, continuous electronic fetal heart rate monitoring and the uterine
activity may help the obstetrician in the assessment of the severity of
placental abruption. Even if the uterine contractions are irregular, their
amplitude and frequency usually exceeds that of a normal labor
contraction, and the baseline tone of the uterus is often increased.
Fetal heart rate monitoring might display various FHR abnormalities,
including fetal tachycardia, loss of baseline variability, sinusoidal
Page | 29 PREDICTORS OF ABRUPTIO PLACENTA
BIOCHEMICAL MARKERS:
MSAFP- Second trimester elevation of MSAFP may be a biochemcial
marker that is related to certain adverse obstetric outcome including
placental abruption. There is chronic villitis and vascular thromboses or
infarction which is thought to cause this elevation.AFP levels
>2.0MoM was found in 17% of pregnancies with placental abruption.
Page | 30
Beta HCG Increased levels of maternal serum beta hcg has been linked
to an increased chance of developing placental abruption.
PAPP-A Low levels of PAPP-A in the first trimester has been linked
with placental abruption .
Proangiogenic placental growth factor (PIGF) and antiangiogenic
soluble - fms like tyrosine kinase-1(sflt-1) are angiogenic regulators in
pregnancy. Increased ratio of sflt1/PIG F at 21-32 weeks of gestation
puts a woman at risk of placental abrubtion ,in those who have
developed preeclampsia or gestational hytpertension.
Fibronectin produced by the endothelial cell is increased in cases of
placental abruption .
Thrombomodulin ,a marker of endothelial cell damage may be elevated
in placental abruption .
Uterine artery flow measurement:
Increased uterine artery pulsatility index at 11-14 weeks or notching of
the uterine artery waveform at 20-24 weeks also may predict
subsequent placental abruption.
But none of these are accepted as standard methods to diagnose
Page | 31 COMPLICATIONS OF ABRUPTIO PLACENTA
The principal maternal complications associated with abruption placenta are:
• Hemorrhagic shock resulting from acute blood loss which causes a contraction of the intravascular compartment
• generalized coagulopathy due to active consumption of clotting factors within the vascular tree and consequent secondary fibrinolysis
• ischemic necrosis of distant organs. The organs most frequently involved are the kidneys and the anterior pituitary gland.
• Acute renal failure is a serious complication and may lead to maternal death
• preterm PROM resulting from decidual hemorrhage.
HEMORRHAGIC SHOCK
• Hemorrhagic shock is caused by an absolute reduction in peripheral circulating blood volume along with subsequent tissue hypo perfusion.
The shock that occurs in patients with abruptio placentae is usually out
of proportion to the observed blood loss.
• The end point of persistent hypotension is asphyxia of both the fetus and mother; therefore, the immediate treatment is replacement of the
intravascular volume deficit as rapidly as possible and restoring
Page | 32
• Crystalloids should be infused until cross matched blood is available. Crystalloid therapy initially should involve volumes two- to three-times
in excess of the actual hemorrhage, because shock often is associated
with major fluid shifts from the intravascular to the extravascular
compartments.
COAGULOPATHY
• The inciting event leading to DIC with placental abruption is thought to be entry of thromboplastins from the placental injury site into the
circulation. The thromboplastins cause widespread intravascular
activation of the clotting cascade. There is widespread activation of the
coagulation system within the vascular compartment which produces a
consequent depletion of various clotting factors and a resultant
hemorrhagic state.
• The extensive conversion of fibrinogen to fibrin results in a decrease in the concentration of fibrinogen.
• Secondary fibrinolysis leads to the formation of fibrin degradation products (FDP), which, by their anticoagulant effect, further
compromise the hemostatic system.
• Levels of prothrombin, factor V, factor VIII, and platelets also are decreased.
Page | 33
• Steps for immediate delivery of the fetus should be taken that would help to improve the haemostatic competence
ISCHEMIC NECROSIS OF DISTANT ORGANS
• Ischemic damage to the kidneys is a well known complication of severe abruptio placentae and takes the form of acute tubular necrosis, bilateral
cortical necrosis, or both.
• The pathological changes are explained on the basis of inadequate blood supply and hypoxia from hemorrhagic hypovolemia (or)an
obstruction secondary to focal fibrin deposits in the precapillary
arterioles due to DIVC.
• Acute tubular necrosis, the most common cause of anuria in
obstetrics,is generally due to hemorrhagic shock with resultant anoxic
insult to the tubular structures of the renal medulla.
• When extreme oliguria or anuria develops,it is impossible to initially distinguish between acute tubular necrosis and acute cortical necrosis.
• Acute renal failure with lower nephron damage usually occurs later in the abruption process and is reversible after a period of time. In
contrast, the pattern of acute cortical necrosis shows involvement early
in the abruption process; if the condition is untreated by dialysis, the
Page | 34
• The key to prevention of renal ischemic damage is vigorous blood and fluid therapy to combat hypovolemic shock.
PERINATAL COMPLICATIONS
• The perinatal morbidity and mortality rate associated with abruption is as high as 20% to 40% and accounts for 15% of all perinatal deaths.
The three major causes of perinatal death are fetal anoxia,
exsanguination (because, in rare cases, rupture of fetal placental vessels
can occur), and prematurity.
• The likelihood of a normal neonatal outcome decreases with the severity of abruption. Poor outcome may be caused by the fact that
perinatal hypoxic–ischemic injury starts in utero, caused by an
interruption in placental blood flow and gas exchange.
MANAGEMENT
GENERAL MANAGEMENT:A proper history and quick cinical
assessment should be done in women presenting with antepartum
haemorrhage and decided whether urgent intervention is required to
manage maternal or fetal compromise. In those women presenting with
massive haemorrhage,iv lifelines should be secured, blood drawn for
crossmatching and resuscitation should be started immediately since
mother is the priority and should be stabilised first. Meanwhile blood
Page | 35
The investigations include:
Blood Hb%
Platelet count
Leucocyte count
Peripheral blood smear
Blood for grouping and typing
Bleeding and clotting time
Clot observation and retraction time
Prothrombin time
Activated partial thromboplastin time
Serum fibrinogen level
Fibrin degradation product levels
D-dimer levels
Liver function tests
Renal function tests
Page | 36
OBSTETRIC MANAGEMENT:
The clinical presentation of placental abruption being variable, the obstetric
management is individualised on individual basis.The presentation,
gestaional age and the degree of maternal and fetal compromise will direct
the management.
In cases of abruption at or near term with a live fetus, prompt delivery is
indicated. If there is fetal compromise, and delivery is not
imminent,Caesarean section should be performed. When the maternal and
fetal conditions are reassuring vaginal delivery may be reasonable.
In patients with severe placental abruption resulting in intrauterine fetal
death, if the mother is stable, it is reasonable to allow for a vaginal delivery
in the absence of any obstetric indications.
Labour usually progresses rapidly because of viguorous uterine
contractions and an amniotomy and oxytocin augmentation may speed up
delivery. The main purose of doing an amniotomy is to hasten the onset of
labour and by encouraging uterine contractions, to reduce uterine bleeding.
Anytime, when the fetal heart rate deteriorates, or the maternal condition
becomes worse or when labor does not progress rapidly or in case of
obstetrical indications like cephalopelvic disproportion, a scarred uterus or
a fetal malpresentation,a caesarean delivery may be performed to avoid
Page | 37
of any coagulation defects is very much essential during surgery. The
patient should be closely monitored paying attention to vital signs, amount
of blood loss, urine output.
PREVENTION OF ABRUPTIO PLACENTA
• Early diagnoses and appropriate treatment of hypertensive disorders of pregnancy.
• Avoidance of sudden rupture of membranes.
Page | 38 MATERIALS AND METHOD:
TYPE OF STUDY : LONGITUDINAL STUDY(OBSERVATIONAL)
PERIOD OF STUDY : JAN 2018 - AUGUST 2018
PLACE OF STUDY : Dept. Of Obstetrics and Gynaecology
Govt. Kilpauk Medical College,Chennai.
METHODOLOGY:
• Patients admitted with clinical presentation of abruptio placenta – vaginal bleeding, pain abdomen or uterine tenderness after 24 weeks of
gestation (gestational age from dating scan was considered ) were
included in the study as cases.
The diagnosis of abruption placenta was confirmed later on by placental
examination.
• All the patients in the study population were clinically evaluated and worked up immediately with ultrasonogram,complete hemogram,renal
function test,liver function test, serum electrolytes and coagulation
profile and were followed for about 4 weeks
• A questionnaire which included the demographic profile and risk factors of the mothers was used to collect data. This included details
like maternal age, obstetric score,AN visits,and the gestational period at
which abruption occurred ,etc. Details of associated medical problems
(preeclampsia, gestational diabetes mellitus (GDM), hypothyroidism
Page | 39
pregnancies,anemia,polyhydramnios,growth restriction, history of
threatened abortion, previous preeclampsia and PROM) were noted.
• Intra-partum findings were recorded.
• Maternal outcome like shock,post partum hemorrhage,acute renal failure, need for mechanical ventilation,Disseminated Intra Vascular
Coagulation,etc were recorded.
• The fetal/neonatal outcome like intrauterine demise, birth weights, and an Apgar score at 1 min and 5 min were recorded and compared.
Page | 40 RESULTS & DISCUSSION
AGE DISTRIBUTION
Of the 51 patients included in the study, the youngest age at which abruption
occurred was 18 years and the oldest age was 33 years.The average age of the
study group was 24.5 years.
AGE GROUP NO. OF PATIENTS PERCENTAGE
<20 8 15.6%
20-25 21 41.1%
26-30 19 37.2%
>30 3 5.8%
It was also noted that in both extremes of age, the severity of abruption was
high.
16%
41% 37%
6%
Age distribution
Page | 41 ABRUPTION AND GESTATIONAL AGE
The average gestational age of occurrence of abruption was 34 weeks,with
least GA being 25 weeks of gestation.
The distribution of abruption based on gestational age is as follows:
GESTATIONAL AGE CASES % OF CASES
24-34 weeks 26 50.98
35-36 weeks 17 33.33
>37 weeks 8 15.68%
50.98
33.33
15.68
gestational age
24-34 weeks
35-36 weeks
Page | 42 DISTRIBUTION OF CASES BASED ON BOOKING STATUS
Among the 51 participants in the study,96.1%(49) were booked and 3.9% (2)
were unbooked. It was noticed that the unbooked patients invariably presented
with grade 3 abrution when compared to the booked patients(Grade 1- 7.8%,
grade 2- 39.2% and grade 3- 49%).
96.1 3.9
BOOKING
BOOKED
Page | 43
Among the booked patients,18(36.7%) had concealed abruptions and
31(63.3%) had revealed abruption.and among those who were unbooked, 50%
had concealed and 50% had revealed abruption.
Page | 44 DISTRIBUTION BASED ON PARITY
PARITY NUMBER OF CASES PERCENTAGE
PRIMI 23 45.1%
MULTI 28 54.9%
Of the multigravidas, 7 (13.7%) were 3rd gravida and above and all of them
presented with grade 3 abruption. Multiparity is hence a risk factor for the
development of abruption. Of all the multigravidas(3 or more), 71.4% of them
presented with revealed abruption and the remaining 28.6% presented with
concealed abruption.
45% 55%
PARITY
PRIMI MULTI
0 100
multiparity
PARITY AND ABRUPTION
Page | 45 DISTRIBUTION BASED ON THE GRADE AND TYPE OF
ABRUPTON
GRADE(SHER CLASSIFICATION)
NO. OF CASES % OF CASES
1 4 7.84%
2 20 39.21%
3 27 52.94%
DISTRIBUTION BASED ON TYPE OF ABRUPTION
TYPE OF ABRUPTION
NO. OF PATIENTS % OF PATIENTS
COCNEALED 19 37.3%
REVEALED 32 62.7%
8%
39% 53%
GRADES OF ABRUPTION
GRADE 1 GRADE 2 GRADE 3
37%
63%
TYPE OF ABRUPTION
Page | 46 DISTRIBUTION BASED ON RISK FACTORS
RISK FACTORS NO. OF CASES % OF CASES
PRE ECLAMPSIA 31 60.78
ANEMIA 26 50.98
MULTIPARITY 7 13.72
POLYHYDRAMNIOS 12 23.50
PLACENTA PREVIA 2 3.92
GDM 4 7.84
TWINS 2 3.92
Thus,in our study 60.78% of the patients had pre eclampsia,and 50.98 %
patients had anemia which were considered as the two leading risk factors for
Page | 47 ANEMIA AND ABRUPTION DISTRIBUTION
Among all the abruption cases under study, 25 patients (49%) did not have
anemia and 26 patients(51%) had anemia complicating pregnancies.Among all
these cases,4 cases(7.8%) had grade 1 abruption, 20 (39.2%) had grade 2
abruption and 27(60%) had grade 3 abruption.Among those with grade 3
abruption,9(33.3%) were not anemic whereas 18( 66.7%) were anemic.Hence
anemia is a risk factor for severe grades of abruption.
It was also notes that in those patients without anemia,11(21.6%) had
concealed abruption and 14( 27.5%) had revealed abruption, but in those
complicated with anemia,8(15.7%) presented with concealed abruption and
18( 35.3%) presented with revealed abruption.
Page | 48 PRE ECLAMPSIA AND ABRUPTION DISTRIBUTION
Among all the abruption cases,20(39.2%) did not have pre eclampsia, whereas
31(60.8%) cases were complicated by pre eclampsia.In patients with grade 1
abruption, 50 % had pre eclampsia and 50% did not have. In grade 2
abruption,35% did not have and 65% had pre eclampsia and in those with
grade 3 abruption,40.7% did not have pre eclampsia whereas 59.3% had pre
eclampsia. This shows that pre eclampsia is an important risk factor for
development of more severe grades of abruption.
Also 23.5% of cases with concealed abruption and 37.3% of cases with
revealed abruption had pre eclampsia ,whereas only 13.7% of cases with
concealed abruption and 25.5% of cases with revealed abruption did not have
Page | 49 POLYHYRAMNIOS AND ABRUPTION PATTERN
Among all the abruption cases,39(76.5%)did not have polyhydramnios and
only 12 (23.5%) had polyhydramnios.Among those with grade 1 abruption,
only 25% had polyhydramnios. In those with grade 2 abruption, only 35% had
polyhydramnios and among those with grade 3 abruption,only 14.8% had
polyhydramnios.Hence polyhydramnios alone is not a single independent risk
factor for predicting the severity of abruption.
In our study, only 26.3% of those with concealed abruption and 21.9% of those
with revealed abruption. Hence polyhydramnios did not influence the type of
Page | 50 PLACENTA PREVIA AND ABRUPTION PATTERN
In our study,49(96.1%) of the patients did not have placenta previa and
2(3.9%) patients had placenta previa and those who had placenta previa
presented with grade 2 or grade 3 abruptions.Among those cases who had
placenta previa, the abruption was revealed in both the cases.
Hence abruption cases complicated by placenta previa usually tend to present
Page | 51 GDM AND ABRUPTION
Among all the abruption cases,47(92.2%) cases did not have GDM and
4(7.8%) of the cases had GDM.of those patients with grade 1
abruption,nobody had GDM, in grade 2 abruption,2(10%) had GDM and in
grade 3 abruption, 2(7.8%) had GDM.Hence GDM is not an independent risk
factor for determining the severity of abruption.
In our study, among those with GDM, 50% showed revealed abruption and
50% showed concealed abruption,whereas in normal population incidence
Page | 52 TWIN PREGNANCY AND ABRUPTION PATTERN
In our study,49(96.1)patients had only a singleton pregnancy whereas 2(3.9)
patients had a twin pregnancy.Both the patients presented with grade 2
Page | 53 DISTRIBUTION BASED ON PRESENTING SYMPTOMS
PRESENTING
SYMPTOMS/SIGNS
NO. OF CASES % OF CASES
PAIN ABDOMEN 42 82.35%
BLEEDING P/V 32 62.74%
TENSE/TENDER UTERUS 17 33.33%
DECREASED FETAL
MOVEMENTS
5 9.8%
ASYMPTOMATIC 3 5.8%
The leading presenting complaints in cases of abruption placenta was found to
be pain abdomen in 82.35% of cases followed by bleeding p/v in 62.74% of
cases.Tense/ tender uterus was found only in 33.33% of cases and about 5.8 %
Page | 54 PRESENTING SYMPTOMS AND SEVERITY OF ABRUPTION
In our study, 96.3% of cases with grade 3 abruption; 80% of cases with grade
2 abruption and 0% of those with grade 1 abruption presented with pain
abdomen.
In this study,59.3% of cases with grade 3 abruption,80% of cases with grade 2
abruption presented with complaints of bleeding per vaginum.
In this study 35% of cases with grade 2 abruption and 37% of cases with grade
3 abruption presented with a tense/tender uterus.
Page | 55 LEVEL OF SHOCK AND SEVERITY OF ABRUPTION
In our study,of those who presented with level 1 shock, 4(11.1% ) cases had
grade 1 abruption 17(47.2%) cases had grade 2 abruption and15( 41.7% ) cases
had grade 3 abruption.
Among those cases who presented with level 2 shock,3(21.4%) cases had 2
abruption,11( 78.6%) cases had grade 3 abruption.
Among those cases who presented with level 3 shock, 100% of the cases had
grade 3 abruption.
Among those who presented with level 1 shock,47.2% cases presented with
concealed abruption and 52.8% cases presented with revealed abruption. Of
those who presented with 2 shock,14.3% cases had concealed and 85.7% cases
had revealed abruption and 100% of the cases with level 3 shock had revealed
Page | 56 DISTRIBUTION OF CASES BY MODE OF DELIVERY
Among all the 51 cases of abruption,37(72.5%) cases underwent cesarean
section,13(25.5%) cases had a normal vaginal delivery and1(2%) case had an
instrumental delivery.
In this study,among those who delivered by labor natural, 7.7% had grade 1
abruption, 7.7% had grade 2 abruption and 84.6% had grade 3 abruption.
Among those who delivered by LSCS, 8.2% cases had grade 1 abruption,
48.6% cases had grade 2 abruption and 43.2% of cases had grade 3 abruption.
Instrumental delivery was done only for 1 case,which was a grade 2 abruption. 72%
26% 2%
MODE OF DELIVERY
Page | 57 DISTRIBUTION BY COMPLICATIONS
COMPLICATION NO. OF CASES % OF CASES
PPH 10 19.6%
Acute Kidney Injury(AKI) 24 47.05%
NEED FOR DIALYSIS 11 21.56%
MASSIVE BLOOD
TRANSFUSION(>/= 4)
12 23.52%
DIVC 9 17.64%
HELLP 13 25.49%
PULMONARY EDEMA 1 1.96%
VENTILATORY
SUPPORT
3 5.88%
COUVEILAIRE UTERUS 15 29.41%
The average duration of hospital stay was 19.71 days( 9.25 days in grade 1
abruption;18.1 days for grade 2 and 22.44 days for grade 3 abruptions.
There were no maternal deaths due to abruption placenta or its complications
Page | 58 GRADES OF ABRUPTION AND POST PARTUM HEMORRHAGE
In our study, of the10 cases(19.6%) which were complicated by PPH, 30% of
the patients had grade 2 abruption and 70 % of the cases had grade 3
abruption.
And among those cases who were complicated by PPH, 50% was a revealed
Page | 59 GRADES OF ABRUPTION AND ACUTE KIDNEY INJURY
In our study, of the 24 cases(47.05%) that were complicated by AKI, 25% had
grade 2 abruption and 75% had grade 3 abruption.
Among the cases complicated by AKI,41.7% cases had concealed and 58.3%
Page | 60 GRADE OF ABRUPTION AND NEED FOR DIALYSIS
Among all the cases of abruption,11 cases(21.56%) had AKI which required
dialysis, among which,all 11 cases(100%) was due to grade 3 abruption.
Page | 61 ABRUPTION AND MASSIVE BLOOD TRANSFUSION
Of all the cases complicated by abruption, 12 cases (23.52%) required massive
blood transfusion of 4 or more blood units of which all 12(100%) was due to
grade 3 abruption.
And among these cases, 50% had concealed abruption and 50% had revealed
Page | 62 GRADES OF ABRUPTION AND DIVC
Among all the cases of abruption, 9 cases(17.64%) had DIVC,of which 11.1%
was due to grade 1 abruption and 88.9% was due to grade 3 abruption; and
Page | 63 GRADES OF ABRUPTION AND HELLP SYNDROME
Among all the cases of abruption under study,13cases(25.49%) was
complicated by HELLP syndrome , of which,23.1% was due to grade 2
abruption and 76.9% was grade 3 abruption.Also,38.5% of the cases had
Page | 64 ABRUPTION AND PULMONARY EDEMA;NEED FOR
VENTILATORY SUPPORT
In our study, of all the cases of abruption,1 case(1.96%) went in for pulmonary
edema and 3 cases(5.88%) needed ventilator support.
Among the cases that required ventilator support, 33.3% had grade 2 abruption
Page | 65 ABRUPTION AND COUVELAIRE UTERUS
Among all the cases of abruption, 15 cases (29.41%)had couvelaire uterus, of
which 6.7% cases had grade 1 abruption ;13.3% cases had grade 2 and 80% of
the cases had grade 3 abruption.
Page | 66
In our study,among the 51 patients, a total of 15 cases(29.41%) had couvelaire
uterus,which was detected during a caesarean section. The average amount of
retro placental clots found in these cases was 390 gram. Among these cases
with a couvelaire uterus,the rates of complications are as follows.
About 3 patients(20%) went in for post partum hemorrhage(PPH);10
cases(66.66%) went in for acute kidney injury;6 cases(40%) required
hemodialysis;9 cases(60%) required a blood transfusion of 4 or more units;6
cases(40%) were complicated by DIVC and 3 cases (20%) went in for HELLP
syndrome. This shows that in patients with couvelaire uterus,the complication
rates are quite high,especially post partum hemorrhage and acute kidney
injury.
Among those patients who required hemodialysis;1 case(16.66%) required
only 1 cycle; 2 cases (33.33%) required 2 cycles and 3 cases(50%) required 3
or more cycles or hemodialysis. 0 2 4 6 8 10 12
PPH AKI DIALYSIS MASSIVE TRANSFUSION
Page | 67 ABRUPTION- DELIVERY INTERVAL
The average abruption – delivery interval in our study was 3.32 hours, which
was around 2.4 hours in grade 2 abruption and 4 hours in grade 3 abruption.
RETROPLACENTAL CLOTS AND ABRUPTION
In our study, among all the cases of abruption,the average amount of
retroplacental clots was 269.6 grams.
In grade 1 abruption, average retroplacental clots was 50g
In grade 2 abruption, average retroplacental clots was 162.5g
In grade 3 abruption,average retroplacental clots was 381.4g 17%
33% 50%
HEMODIALYSIS
Page | 68
In our study, majority of the patients(49.01%) had 100-299 gram of retro
placental clots,27.45% of cases had 300-499 gram retro placental
clots,15.68% cases had retroplacental clots 500 gram or more and only 7.84%
cases had retroplacental clots <100 gram
8%
49% 27%
16%
RETRO PLACENTAL CLOTS
<100 GRAM 100-299 GRAM 300-499 GRAM 500 GRAM AND ABOVE RETROPLACENTAL
CLOTS
NO. OF CASES PERCENTAGE
<100 gram 4 7.84%
100-299 gram 25 49.01%
300-499 gram 14 27.45%
Page | 69 DISTRIBUTION OF COMPLICATION BASED ON RETRO
PLACENTAL CLOTS
In our study, among the 10 patients who had post partum hemorrhage, 40 %
had 100-299 gram of retro placental clots and 30% had retro placental clots of
300-499 gram and 30% had 500 gram or more of retro placental clots.
40%
30% 30%
PPH
100-299 gram 300-499 gram 500 gram& above RETRO
PLACENTA L CLOTS(g)
PPH AKI DIALYSI
S
BLOOD
TRANSFUSION
(4/MORE)
DIVC HELLP PULMON
ARY
EDEMA
VENTILATOR
SUPPORT
<100 0 0 0 0 0 0 1 0
100-299 (4)
40% (8) 33.33 % 1 (9.09%) 1 (8.33%) 1 (11.11%) 5 (38.46%)
0 1
300-499 (3)
30% (9) 37.5% 6 (54.54%) 4 (33.33%) 5 (55.55%) 7 (53.84%)
0 1
500 or more (3)
30% (7) 29.16 % 4 (36.36%) 7 (58.33%) 3 (33.33%) 1 (7.69%)
0 1
Page | 70
Among the 24 patients who went in for acute kidney injury, 37.5% cases had
RP clots of 300-499 gram, 33.33% had RP clots of 100-299 gram and 29.16%
had RP clots of 500 grams or more.
Among the 11 cases which required dialysis, 9.09% of cases had only 100-299
gram of retro placental clots, 54.54% had 300-499 gram of retro placental clots
and 36.36% had retro placental clots of 500 gram and above. 33%
38% 29%
AKI
100-299gram 300-499gram 500 gram& above
9.09
54.54 36.36
DIALYSIS
100-299gram
300-499gram
Page | 71
Among the 12 cases that required a blood transfusion of 4 or more units,
58.33% cases had 500 gram or more of retro placental clots,33.33% had
300-499 gram retro placental clots and 8.33% cases had retro placental clots of
100-299 gram.
Among the 9 cases that were complicated by DIVC, 11.11% cases had retro
placental clots 100-299 grams, 55.55% cases had retro placental clots of
300-499 gram and 33.33% cases had retro placental clots of 500 gram and above. 8%
33% 59%
BLOOD TRANSFUSION >4 UNITS
100-299gram 300-499gram 500gram & above
11.11
55.55 33.33
DIVC
100-299gram
300-499gram
Page | 72
Among those who developed HELLP syndrome, 38.46% cases had 100-299
gram retro placental clots, 53.84% cases had 300-499 gram of retro placental
clots and 7.69% cases had retro placental clots of 500 gram and above.
Only one case had pulmonary edema ,in whom retroplacental clots was <100
grams and 3 cases required ventilatory support,but the amount of retro
placental clots did not correlate with the need for ventilator
support.(mentioned in table)
38%
54%
8%
HELLP SYNDROME
Page | 73 FETAL OUTCOME- BIRTH WEIGHT
The average weight of the fetuses delivered was 2.02 kg .The average birth
weight of the babies were 2.47kg in grade 1 abruption, 2.1kg in grade 2
abruptions and 1.89kg in grade 3 abruptions.
This low birth weight is attributed to premature delivery of the fetuses in view
Page | 74 FETAL OUTCOME- APGAR
The average 1 minute APGAR for the babies delivered was 5 and the 5 minute
APGAR was 7. But this APGAR score only denotes the well being of those
babies which were delivered promptly in grade 1/ grade 2 abruptions. Hence
when the diagnosis of an abruption is made and appropriate timely delivery of
the fetus is done, the fetal outcome is usually good.
Page | 75 ABRUPTION AND INTRAUTERINE FETAL DEMISE
In our study, among all 51 cases of abruption,26 cases(50.9%) presented with
an intrauterine fetal demise and the remaining 25 cases (49.1%) cases had live
babies. Among those cases with intrauterine fetal demise,16 cases(61.53%)
underwent a caesarean section and 10 cases(38.46%) delivered by labor
natural. Among the live babies, 21 cases (84%) were delivered by caesarean
section and 3 cases(12%) by labor natural and 1 case(4%) by instrumental
delivery.
0
5 10 15 20 25 30
IUD BABIES LIVE BABIES
INSTRUMENTAL DELIVERY
LSCS
Page | 76 SUMMARY
• Among all the cases of abruption included in this study,the maximum incidence of abruptio placenta was seen between age group 20-25
years(41.1%). The lowest age of abruptio placenta in this study was 18
years and the highest was 33 years.
• The incidence of abruption was greatest in multipara( 55% ) when compared to primi.
• Maximum incidence of abruption occurred between 24-34 weeks(51.9%) weeks of gestation.
• Booked antenatal cases constituted the majority because of the
government policies and extended coverage by the primary health care
system produced by our State Government. Only 2 cases were
unbooked in our study.
• The main presenting symptoms were abdominal pain in 82.5%; followed by vaginal bleeding in 62.74%.9.8% of the cases presented
with reduced perception of fetal movements and 5.8% cases were
asymptomatic.
• The majority of abruptions were Grade 3 abruptions(52.94%) followed by Grade2 and Grade 1, as per Sher’s classification.
• Majority of the abruptions were revealed abruptions(62.7%). • The average abruption – delivery interval was 3.32 hours, which
Page | 77
facilities,that has enabled the patient to identify the alarming symptoms
and the prompt timely management by the hospital.
• The most common risk factor that was found in our patients was pre eclampsia of varying severities in 60.78% followed by anemia in
50.98% of the cases.Multiparity of 3rd gravida and above was found in
13.72%, polyhydramnios in 23.5%,placenta previa and multiple
pregnancy in 3.92% and gestational diabetes in 7.84% of the cases.
• 72.5% of the cases in our study were delivered by cesarean section , 25.5% by normal vaginal delivery and 2% by instrumental delivery.
The most common indication for a cesarean delivery was previous
LSCS/ fetal distress.thought he LSCS rate was high, the maternal
morbidity was lesser and perinatal outcome was better for the live
babies .
• The most common complication observed was acute kidney injury,in 47.05% of the cases and 21.56% of the cases required
dialysis.Couvelaire uterus was found in 29.4% of the cases in cesarean
section. Coagulation abnormalities were present in 17.64% of
patients.25.49% of the cases went in for HELLP syndrome,19.6% of the
cases went in for PPH.23.52% of cases required a blood transfusion of
>4 units. 5.8% of the cases required ventilatory support.
• The average amount of retroplacental clots was 269.6 grams and all the above mentioned complications was high in patients in whom
Page | 78
• There was no maternal mortality in our study,which is attributed to the prompt and timely action in the diagnosis and management of abruption
cases and to the multidisciplinary approach with the availabilty of
expert obstetricians,anaesthesiologists,
paediatricians,nephrologists,physicians and cardiologists.
• 51% of the cases had an intrauterine fetal demise, which was due to the grade 3 abruption.Among these 61.53% cases had a cesarean delivery
and 38.46% cases had normal delivery.
• Among those live babies delivered,84% were delivered by cesarean section and the average birth weight of the babies was 2.02 kg and this
low birth weight is attributed to prematurity.
• Among the live babies, the average 1 minute APGAR was 5 and 5 minute APGAR was 7, and these babies did cope up well after delivery.
This is attributed to the timely delivery of these salvageable babies in
cases of abruptio placenta.
Page | 79
CONCLUSION
This study has shown that placental abruption represents a set of potentially
serious obstetric emergency, which has a great impact on maternal and
neonatal mortality and morbidity and is one of the major risk factors for a
preterm delivery.
The chief risk factors identified in this study are pre eclampsia and anaemia
complicating pregnancy. So if these risk factors are identified at an early stage
by adequate antenatal care and treated appropriately, the incidence of
abruption and hence the maternal and perinatal mortality/morbidity can be
reduced in our community.
A major number of patients presented with Grade 3 abruption with a resultant
intrauterine death of fetus. So early identification of the problem and timely
referrals from the peripheral institution would help to bring down the perinatal
Page | 80 BIBLIOGRAPHY
1. Konje JC, Taylor DJ. Bleeding in later pregnancy. In: James DK, Steer PJ, Weiner
CP, Gonik B editors. High risk pregnancy 3 rd ed. Philadelphia: Pennsylvania; 2006.
1266-71.
2. Pitaphrom A, Sukcharoen N. Pregnancy outcomes in placental abruption. J Med
Oncolassoc Thai. 2006; 1572-8.
3. Ananth CV, Lavery JA, Vintzileos AM. Severe Placental Abruption:Clinical
definition and associations with maternal complications. Am J Obstet Gynaecol.
2016;214;272.e1-9
4. Kyrklund-Bloomberg BN, Gennser G, Cnattinguis S. Placental abruption and
perinatal death. Paediatr Perinat Epidemiol. 2001;15:290-7.
5. Willium A, Lieberman E, Mittendorf R. Risk factors of abruption placentae. A J of
Epidemiol. 1991; 134(9):965-72.
6. Menom MK, Sokshi SK. Accidental haemorrhage in teaching hospital. J Obstet
Gynaecol Ind. 1961; 11:335-41.
7. Wasnik SN and Naiknaware SV. Antepartum Haemorrhage: Causes and its effects
on Mother Child: An Evaluation. Obstetri Gynaecol Internat J. 2015;3(1):00072.
8. Bibi S, Ghaffer S, Pir MA, Yousfani S. Risk factors and clinical outcome in
placental abruption: a retrospective analysis J Pak Medic Associat.
Page | 81
9.Campbell S, Lee C. Disorders of placentation. In: Obstetrics by ten teacher 17th ed.
Arnold London 2002.p.171-3.
10. Shrivastava V, Kotur P, Jauhari A. Maternal and Fetal outcome among Abruptio
Placentae at a rural tertiary hospital in Karnataka, India: A Retrospective analysis. Int
J Res Med Sci. 2014;2(4):1655-8.
11. Subramaniyan V, Pachamuthu U, Dhanapal M, Abruptio Placentae: A
Retrospective Study. 2016;5:10.
12. Choudhary V. Rathi Somani S, Somani S. Evaluation of Risk factors and
Page | 82
ANNEXURES
STUDY PROFORMA
ABRUPTIO PLACENTA-AN OBSTETRIC ENDANGERMENT
NAME OF THE PATIENT
PATIENT IP NUMBER
DATE & TIME OF ADMISSION
REFERRAL
AGE
HEIGHT(cm)
WEIGHT(Kg)
BMI
VITALS AT THE TIME OF ADMISSION
LEVEL OF SHOCK
OBSTETRIC SCORE WITH PREVIOUS MODE OF DELIVERY(IF ANY)
LMP
Page | 83
GESTATIONAL AGE AS PER LMP
GESTATIONAL AGE AS PER DATING SCAN
PRESENTING COMPLAINTS WITH DURATION
WHETHER BOOKED AND IMMUNISED*
PREVIOUS OBSTETRIC EVENTS
OTHER OBSTETRIC RISK FACTORS:(YES/NO)
1)ANEMIA
2)PRE-ECLAMPSIA
3)GDM
4)MULTIFETAL GESTATION
5)CONCEPTION AFTER ARTIFICIAL REPRODUCTIVE TECHNOLOGY
6)NON VERTEX PRESENTATION
7)PREVIOUS LSCS
8)PROM/PPROM
9)POLYHYDRAMNIOS
Page | 84
ABRUPTION
11) MATERNAL TOBACCO CHEWING/SMOKING
12)HISTORY OF BLUNT ABDOMINAL TRAUMA/FALL
EXAMINATION FINDINGS
ULTRASONOGRAM
CONCEALED/ REVEALED ABRUPTION
GRADE OF ABRUPTION (TABLE-1)**
LAB INVESTIGATIONS
HEMOGLOBIN
TOTAL COUNT
DIFFERENTIAL COUNT
PLATELETS
PCV
BLEEDING TIME/CLOTTING TIME
BLOOD SUGAR
Page | 85
CREATININE
Na+/ K+
URINE ALBUMIN/SUGAR
SERUM BILIRUBIN
ASPARTATE AMINO TRANSFERASE
ALANINE AMINO TRANSFERASE
SERUM ALKALINE PHOSPHATASE
SERUM PROTEIN/ALBUMIN/GLOBULIN
PROTHROMBIN TIME
ACTIVATED PARTIAL THROMBOPLASTIN TIME
INR
SERUM FIBRINOGEN
D-DIMER
ABRUPTION-DELIVERY INTERVAL DETAILS OF BLOOD AND BLOOD PRODUCTS TRA