Targeting interleukin-6 in rheumatoid arthritis
Full text
Figure
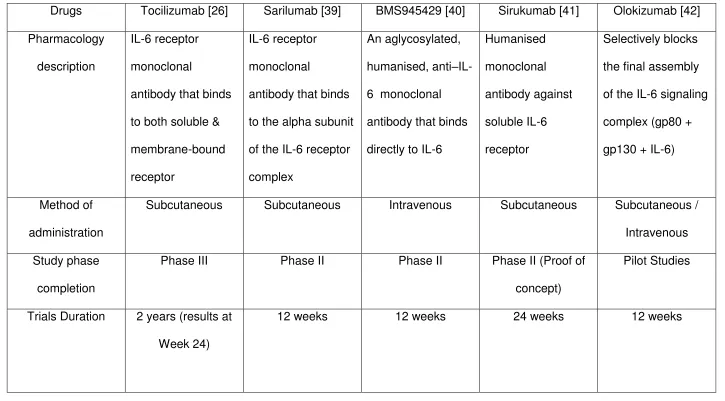
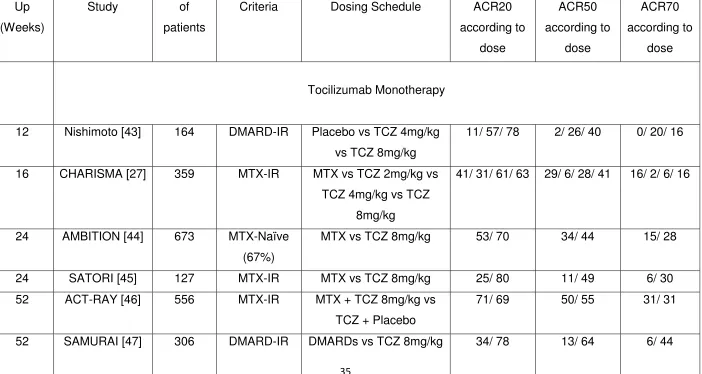
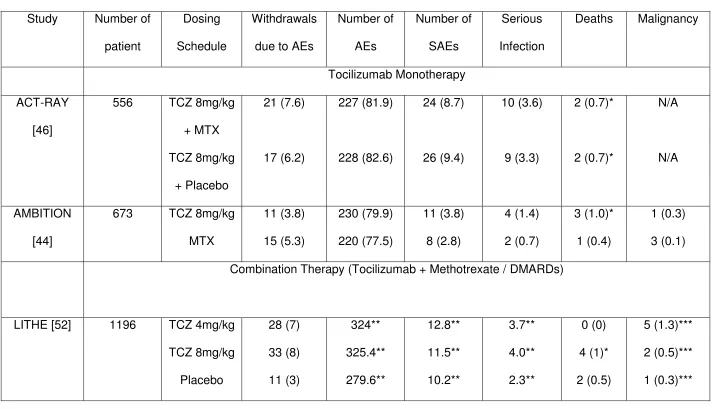
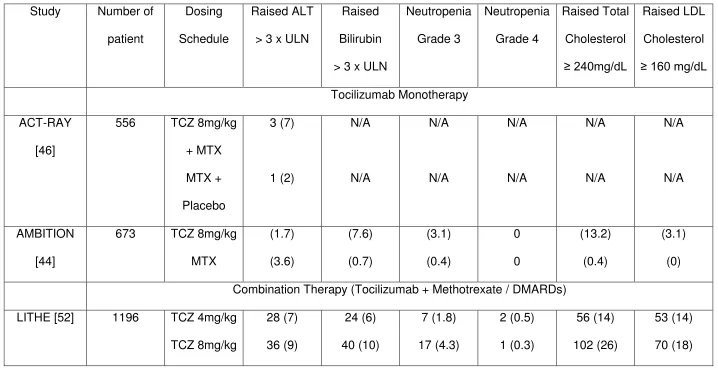
Related documents
This report deals with the Divisions of Government and Political Theory and Interna- tional Relations in the School of Political Sciences in the Faculty of Social Studies at
prevention early intervention and diversion services to minors served by Cupertino Union School District CUSD and the
Different databases used for this course recommendation they are: Former student base- collection of data which is collected using data mining technique
• Citizen participation tool: municipalities are able to contact cyclists directly and vice versa. Cyclists feel that their concerns are
The material substrate cotton makes the fabrication more easy in an handmade embroidery and also makes the antenna to work in higher frequency range and the stainless steel
Our results showed that activation of ER stress by tunica- mycin counteracted the inhibitory effects of GB on cTnI and cTnT levels and apoptosis index, verifying our conclusion
We successfully developed an exposure–response model describing the extent and time course of weight loss in response to sibutramine treatment. We did this by utilizing
The rate of transition of the fuel composition to the equilibrium in considered mode of processing was determined for different starting isotopic compositions of plutonium