A Dissertation on
A PROSPECTIVE CLINICAL STUDY OF
TEMPORAL MANUAL SMALL
INCISION CATARACT SURGERY
Dissertation submitted for
M.S. Degree in Ophthalmology
April 2013
THE TAMILNADU Dr. M.G.R. MEDICAL UNIVERSITY
Dept. of Ophthalmology
Coimbatore Medical College Hospital
Coimbatore
CERTIFICATE
This is to certify that the dissertation entitled “A
PROSPECTIVE CLINICAL STUDY OF TEMPORAL MANUAL
SMALL INCISION CATARACT SURGERY “is a bonafide research
work done by Dr. Vinodhini. K. in partial fulfilment of the requirement
for the degree of Master of Surgery in Ophthalmology.
Prof. Dr. A. Rajendra Prasad,. MS.DO
Date: HOD & Professor, Dept of Ophthalmology
Place: Coimbatore Coimbatore Medical College Hospital.
Date: The Dean,
DECLARATION
I hereby declare that this dissertation entitled “A PROSPECTIVE
CLINICAL STUDY OF TEMPORAL MANUAL SMALL
INCISION CATARACT SURGERY “is a bonafide and genuine
research work carried out by me under the guidance of Prof. Dr. A.
RAJENDRA PRASAD M.S.,(ophthal),D.O.,HOD & Professor,
Department of Ophthalmology, Coimbatore Medical College & Hospital,
Coimbatore.
Date:
Place DR. VINODHINI K
ACKNOWLEDGEMENT
It gave me great pleasure and satisfaction in preparing this
dissertation and I take this opportunity to thank everyone who has made it
possible. Firstly, I would to convey my heartfelt gratitude and sincere
thanks to my guide DR. A. RAJENDRA PRASAD, M.S., D.O., HOD &
Professor, Department of Ophthalmology, Coimbatore Medical College
Hospital, Coimbatore, who with his knowledge and experience, has
provided able guidance and constant encouragement throughout the
course of my postgraduate studies and in the preparation of this
dissertation.
It also gives me immense pleasure to thank Dr. ZAIBUNISSA
M.S., D.O., Professor, Department of Ophthalmology, Coimbatore
Medical College Hospital, Coimbatore, who has been a constant source of
inspiration and has motivated me not only in this dissertation but also
throughout my course.
I would like to extend my heartfelt gratitude to Dr J
SARAVANAN M.S., who performed all the surgeries in the study.
Without his goodwill this dissertation would not have been possible. I
Department of Ophthalmology, Coimbatore for their whole hearted
support throughout.
I would like to express my gratitude to THE DEAN, Prof Dr
VIMALA M.D., Coimbatore Medical College Hospital, Coimbatore for
her able guidance and encouragement. I also thank the administrative
staff of Coimbatore Medical College Hospital, Coimbatore for their help
and permission for carrying out the study availing all the required
facilities in this hospital. I would also like to thank all the staff nurses and
technicians for helping me in this study.
My full hearted thanks to my family, friends and colleagues who
have helped me in all my endeavours, supporting me through all.
Last but not the least; I am most grateful to all my patients for their
kind cooperation, without whom this study would not have been possible.
I pray to almighty for all his blessings.
DATE:
A PROSPECTIVE CLINICAL STUDY OF TEMPORAL
MANUAL SMALL INCISION CATARACT SURGERY
CONTENTS
PART ONE
INTRODUCTION
EVOLUTION OF CATARACT SURGERY
REVIEW OF LITERATURE
PART TWO
AIM OF THE STUDY
MATERIALS AND METHODS
RESULTS AND OBSERVATIONS
DISCUSSION
SUMMARY AND CONCLUSION
BIBLIOGRAPHY
PROFORMA
KEY TO MASTER CHART
ABBREVIATIONS
SMC – senile mature cataract
SIMC – senile immature cataract
V/A – visual acuity
UCVA – uncorrected visual acuity
BCVA – best corrected visual acuity
WHO – World Health Organisation
POD – post operative day
SICS – small incision cataract
MSICS – manual small incision cataract
ECCE – Extracapsular cataract extraction
UV-B – ultraviolet B radiation
US – United States
NPCB – National Program for Control of Blindness
IOL - Intraocular lens
PCIOL – Posterior chamber intraocular lens
ICCE – Intracapsular cataract extraction
CCC – Continuous curvilinear capsulorhexis
PMMA – poly methyl methacrylate
AC – anterior chamber
INTRODUCTION
Blindness is a major public health problem1. It is a devastating physical
condition with deep emotional and economic implications1. A blind
person loses his or her independence and is prone to experience a sense of
profound loss and depression arising from being plunged into darkness1.
The family directly shares the economic burden and indirectly so does the
community1. Blindness is also associated with lower life expectancy1.
Cataract is responsible for 50% of blindness in the world; the overall
prevalence rate varies from 1 to 4% of the population1. Cataract
prevalence increases with age2. As the world’s population ages,
cataract-induced visual dysfunction and blindness is on increase2.Cataract is a
significant global problem of 21st century2.
The challenges are to prevent or delay cataract formation, and cure that
which does occur2. Cataract occurs early in developing countries
compared to developed countries1. Multiple factors like increasing age,
genetic and environmental factors contribute to cataract formation2. In
addition to these factors diabetes, exposure to oral and topical
corticosteroids, malnutrition and dehydrational states contribute to the
The increasing age is an important risk factor and prevalence doubles
with each decade of age after 40years according to a data from Australia2.
The age-adjusted prevalence of cataract in India was three times that of
the US, with 22% of Indians of 75-83 years old having visually
significant cataract, compared to 46% of those aged 75-85years in the
US8. In India cataract occurs nearly 14years earlier than in a comparable
study in US2. This adds to the existing backlog of cataract cases due to
exponential population growth and insufficient health-care resources2.
Environmental risk factors can be altered by reducing ocular exposure to
UV-B radiation and stopping smoking2. In India the high incident light
and populations dependent on outdoor agrarian activities vastly limits the
success of these interventions2.
Cataract progresses faster in diabetic patients, more so in diabetic women
than in men5. People with diabetes have an increased risk of cortical and
subcapsular cataract and are also more likely to have early cataract
surgery2. These associations will assume greater importance as diabetes
continues to increase in both developing and industrialized areas2. The
challenge is to design and deliver widespread public health initiatives
aimed at dietary and physical activity education and behaviour change to
The current 20 million people with severely reduced vision of 3/60 or
worse due to cataract will have swelled to 40 million by the year 20202.
The benefits of cataract prevention are obvious, but unfortunately, the
likelihood of achieving it is remote2.
The cure for cataract is surgery, and is one of the most cost-effective of
all health interventions2. But this is not equally available to all, and the
available surgery does not produce equal visual outcomes2. The need of
hour is comprehensive strategy including preventive measures to avoid
risk factors combined with widespread surgical services capable of
delivering good vision rehabilitation2.
India has the distinction of being the first country in the world to launch a
nationwide National Programme for Control of Blindness quarter of a
century ago30. Cataract surgeries are performed under NPCB30.
Vision 2020 is a global initiative launched by the World Health
Organization in 19991. It is based on the concept that every living person
has a right to sight and aims to eliminate avoidable blindness worldwide
by the year 20201.The Vision 2020 programme was adopted by the
Government of India as a priority area for health development1. Cataract
The surgical services need to be accessible, affordable and effective of
good vision rehabilitation2. The goals of modern cataract surgery include
restoration of vision as completely and as rapidly as possible while
minimizing complications28. At the same time, the post operative
refractive errors should be neglible28.
Phacoemulsification is now the standard technique as it offers early visual
rehabilitation and better un-aided visual acuity than the conventional
sutured extracapsular cataract extraction 31, 15. However, the high
expenses of instrumentation and requirement of advanced training have
limited the role of phacoemulsification in our country16, 17.
Manual sutureless small incision cataract surgery has emerged as a cost
effective alternative to phacoemulsification in the developing world16.
SICS has the advantage of a self-sealing Sutureless incision with least
surgically induced astigmatism at a low cost15. It is a safe, simple,
consistent, stable, and cost-effective way of cataract removal6.
The technique of small incision cataract extraction has various
modifications and names31. Nonphaco Sutureless cataract extraction,
Mini-Nuc technique, Manual phaco small incision surgery is some of the
names given. Modifications involve the site, size and type of incision and
Every modification has its own set of advantages and limitations but the
outcome of cataract surgery depends on the selection of appropriate
technique. Each technique is selected according to the case encountered,
the setting, as well as the surgeon's skill and comfort level.
Present study is done to evaluate the efficacy and safety of temporal
EVOLUTION OF CATARACT SURGERY
The written history of cataract surgery spans around 20 centuries3. The
term “cataract” was introduced by Constantinus Africanus (AD 1018). He
translated the Arabic “suffusion” into Latin “cataracta” meaning
“something poured underneath something” the “waterfall”3.
For more than 20 centuries, couching was the primary method for
dislodging the cataract away from pupil3. The written description came
from our own Indian surgeon Susruta (600 BC) 3. He used two
instruments – a sharp lancet to penetrate the sclera around 4mm temporal
to limbus and a blunt needle passed through the conjunctiva behind the
iris to dislodge the lens. The temporal approach was used as couching
was performed in sitting posture and surgeon facing the patient3. The
surgeon had to be ambidextrous3.
Jacques Daviel, the father of modern cataract surgery introduced the
incisional extraction of the cataract in 17533. He described a planned
extracapsular cataract extraction and he placed the incision in inferior
limbus as patient was operated in seated position3.
The two milestones that occurred in-between 1753 to 1862 changed the
1. Pierre-Francois-Benzet Parnard shifted the incision site to upper part
of eye and the patient was operated in supine position.
2. Carl Himly introduced pharmacological mydriasis.
The focus of cataract surgeons shifted towards intracapsular cataract
extraction as removing the lens in toto was considered to be safe3.
Many eminent surgeons like Albert Von Grafe (1867), Christiane
(1845), A.Terson (1871) and G. Reuling contributed to this3.
Boston’s Henry Williams introduced suturing of the cataract surgery
wound in 18673. Colonel Henry Smith refined the intracapsular
cataract surgery by employing Indian-Smith manoeuvre, a sliding
method to tumble the lens into anterior chamber in 19263.
Lens extraction methods changed with the introduction of various
forceps like Veerhoff forceps, Kalt smooth forceps and Arruga’s
capsular forceps3. Ignacio Barraquer (1917) performed phacoerysis
with pneumatic forceps3.
The next breakthrough came by chemical zonulolysis with alpha
chymotrypsin by Jose Barraquer in 19583. Cryoextraction
was introduced by T. Krawawicz and refined by other surgeons like
Richard Brubaker and David Worhten3.
Harold Ridley introduced artificial lens IOL implantation in 19493.
Between 1965 and 1972, Cornelius Binkhorst modified the IOL
concept. He refined ECCE and used a IOL with two or four loops for
support3. In 1977 Worst devised the “Worst Medallion” IOL, required
suture fixation to iris and two loops through pupil resting on posterior
capsule. This model was used in ICCE cases3. Modern PCIOL was
devised by S P Shearing with J loops.
The era of intracapsular cataract extraction came to an end with the
introduction of intra ocular lens implantation. The need for safe
scaffolding for IOL shifted the focus towards extracapsular cataract
extraction. The other additional influencing factors are the quest for
small incisional cataract wound and lesser post operative
complications. Coonan et al and Wetzig et al showed reduction of
cystoid macular edema and retinal detachment by keeping posterior
capsular intact3.
PC IOL constituted the first generation but gave way to ACIOL and
iris fixating IOLs. But PCIOL again captured the centre stage5.
PCIOL forms the VII generation of IOL with refinement like
multifocal, accommodative capacity5.
ECCE method was refined by many pioneers. William Simcoe
introduced the 23-gauge irrigating cannula with suction by syringe.
He popularised the ‘grasp’ method of nucleus delivery. McIntyre and
James Gill are the pioneers of ECCE movement. The introduction of
the anterior chamber maintaining viscoelastic gel, hyaluronic acid
contributed to safer and more highly successful surgery3.
Charles Kelman (1967) introduced Phacoemulsification of the
cataract through a small wound3. But initially the procedure failed to
catch on due to high rate of complications like corneal edema,
vitreous loss and technical difficulty3. The final flaw was in the lack
of ideal IOL which was corrected in the coming years1. The
innovative idea of new capsulotomy like capsulorrhexis advanced the
safety of phacoemulsification. The resurgence of phacoemulsification
was facilitated by the nucleus manipulation techniques and the
Smaller phacoemulsification probes and foldable implants allowed
the surgeons quest for astigmatically neutral surgical wounds. Girard
was the first to name and describe the scleral tunnel3.
An innovative technique was developed by surgeons to retain the
advantages of phacoemulsification with the need to invest in
equipments. They replaced the mechanics of phaco machine by
modifying the incision architecture and nucleus manipulation. This
technique is described by various terms like manual small incision
surgery, Nonphaco small incision surgery. The cost of the surgery is
reduced significantly by manual methods and use of 6.5mm PMMA
REVIEW OF LITERATURE
MANUAL SMALL INCISION CATARACT SURGERY
MSICS is an alternative surgical technique that developed after
phacoemulsification. It is a safe, simple, consistent, stable, and
cost-effective way of cataract removal6. In this technique the whole nucleus,
or the nucleus divided in parts, is removed through a self-sealing
sutureless tunnel incision42.
In our country due to the earlier occurrence of cataract and the delay in
seeking treatment, mature and hypermature lenses account for a
significant proportion of cataract cases16. We come across dense brown
and black cataracts associated with Pseudo exfoliation and subluxation,
where manual small incision surgery will be a better option18. Even in the
most experienced hands and in the best operative settings,
phacoemulsification is difficult and prone to complications in eyes with
mature white cataracts16. Therefore it is prudent to consider manual small
METHODS
Classic Blumenthal technique uses the ACM (Anterior chamber
maintainer) to allow all steps to be performed under positive irrigation
pressure61. It is modified later and is highly effective and reproducible for
all grades of cataract36.
The Ruit technique is well-known modification of MSICS, used in
developing countries36. This technique uses temporal scleral tunnel
straight incision of 6.5 – 7mm incision61.
VARIATIONS IN INCISION
Wound construction plays a major role in MSICS and has to be carefully
planned depending on the technique and type of cataract and the amount
of astigmatism6. By changing the configuration self sealing nature is
imparted to the wound. This prevented the suture related complication.
The most common cause of post operative visual impairment is
astigmatism14. The astigmatic neutral wound became the goal of incision
modification.
Kratz (1980) introduced posterior scleral incision to improve wound
healing and reduce surgically induced astigmatism68.
Singer (1991) described frown incision to reduce surgically induced
astigmatism61.
Gokhale and Sawhney (2005) studied induced astigmatism with three
scleral incision locations. Their study found induced astigmatism was
lower in the temporal and Superotemporal groups than in the superior
group14.
Lam (2009) modified the incision into large temporal scleral tunnel with
scleral pocket incision with frown configuration.
OPTIMUM INCISION ARCHITECTURE
The incision can be straight, smile shaped, chevron and frown shaped6.
The scleral tunnel incision has three dimensions.
1. The thickness of flap is one third to half the thickness of sclera.
2. The width is the distance from the scleral groove to the point of
entry into the anterior chamber. If it is equal to the length it forms a
square wound and least astigmatism inducing6.
MANAGEMENT OF NUCLEUS
ANTERIOR CAPSULOTOMY
The MSICS techniques have the nucleus prolapsed into the anterior
chamber as a common step47. The nucleus may be rotated into anterior
chamber or picked by a 26-gauge cystitome. The technique of nucleus
prolapse depends on the type of capsulotomy58.
Following a Can-opener capsulotomy, the nucleus is prolapsed
mechanically without hydroprocedures58. A 26-gauge needle or cystitome
is used to perform anterior capsulotomy47. The Sinskey hook or the lens
dialer is used to lift the superior pole of nucleus and prolapse over the
iris. Then it is rotated in a clockwise or in an anti-clockwise so that the
whole nucleus is out. But the advantage of in-bag IOL is lost in
Can-opener capsulotomy58.
Continuous curvilinear capsulorhexis (CCC) developed by Gimble and
Neuhan allows MSICS to retain the advantages in-bag IOL fixation74, 58.
The intact rim prevents extension of anterior capsular tear into posterior
capsule and provides better centration of IOL74, 25. The elastic margins of
the rim allow the safe expression of nucleus58. The right size of CCC is
5mm58. Trypan blue staining of the anterior capsule helps in getting an
optimum size CCC in mature and hypermature cataract cases49.
HYDROPROCEDURES
These procedures are manipulations of the nucleus inside the bag58.
Mastering these techniques allows the surgeon to prolapse the nucleus
without altering the pupil size and utilizes single instrument. This reduces
instrumentation and surgical time. These techniques are not safe in eyes
with very hard cataract or weak zonular support58.
Hydrodissection was introduced by Faust and modified by Fine74. This
procedure separates the nucleus from the cortex and the capsule. The
fluid is injected under the lens capsule which cleaves the cortex from
posterior capsule and mobilizes the nucleus.
Hydrodelineation introduced by Anis separates the outer epinucleus shell
from the inner compact endonucleus74. In this fluid is irrigated forcefully
into the nuclear mass giving rise to ‘golden ring’ sign. This reduces the
size of nucleus significantly so that nucleus extraction through the tunnel
incision becomes feasible58.
VARIATION IN NUCLEUS DELIVERY
The extraction of nucleus is the hardest and most critical part of the
Sandwich technique: the anterior chamber is filled with viscoelastic
material and the nucleus is extracted by sandwiching it between the
irrigating vectis and iris spatula61, 47.
Fish hook technique: this technique was developed by Lahan
(1997)42.The nucleus is delivered by using a bent 30-gauge needle tip or
an irrigating vectis47.
ACM and Sheets glide: this technique is used in Blumenthal MSICS. The
lens glide is placed under the nucleus and gentle pressure on the sclera is
applied. This opens the wound and pushes the nucleus through the tunnel
by the hydrostatic pressure provided by the anterior chamber maintainer36,
61 .
Sinskey hook method: two Sinskey hooks are introduced through two
separate paracentesis. Left hand hook is slipped under the CCC and
elevates the superior pole toward the incision. The right hand hook is
placed beneath the elevated pole prevent the nucleus from falling back
into the bag61.
Viscoexpression: a curved cannula is then insinuated under the nucleus
and the viscoelastic injected beyond the inferior margin of the nucleus.
gently depressed with the same cannula. This allows the tunnel to open
up and allow the nucleus to be expressed out slowly26.
Irrigating cannula method: Ruit technique of MSICS utilizes this method.
An irrigating Simcoe cannula that was designed with a 26-gauge infusion
and a corrugated concave edge was used. It is used to hydro dissect,
loosen and float the nucleus into the mouth of the tunnel and the nucleus
is expressed out64.
Manual phaco fracture: the scleral tunnel is made large enough to lodge
the nucleus by using the ‘chevron’ frown incision. The lodged nucleus is
manually fragmented and removed through the incision. The endothelial
damage is prevented by breaking the nucleus in the tunnel and
astigmatism is reduced by using ‘chevron’ frown incision61.
Nucleus bisection and trisection: the nucleus is divided into two by using
one instrument as the cutter and vectis as the board47. The nucleus
trisection method described by Kansas and Sax splits the nucleus into
three fragments manually using Kansas trisector and vectis. The resulting
small fragments are viscoexpressed through the small incision61. The
frequent complication is transient corneal edema due to the manipulation
Snare technique: a wire loop stainless steel snare is used to snare the
nucleus into fragments and expressed through the incision. It is a single
instrument with two cannulas with the wire loop in the tip of the first
cannula. The wire loop is lassoed around the nucleus and divides into two
pieces by constricting47, 61.
VISUAL OUTCOME OF MANUAL SMALL INCISION
CATARACT SURGERY
The outcome of cataract surgery depends on many factors like
preoperative ocular status, quality of surgery, and the postoperative
correction of refractive error51. Good patient selection is an important
determining factor of final visual outcome51. Pre-operative evaluation of
the patient allows the surgeon to select the appropriate technique in
individual case basis.
The WHO defines visual impairment as vision less than 3/6064.The
impact of cataract surgical services are assessed by number of blind
persons (visual acuity <3/60) who regained vision after cataract
surgery51.The quality of cataract services is assessed by the postoperative
vision 51.
uncorrected visual acuity in at least 80% of surgeries, and ‘poor’ outcome
in less than 5%42.
TABLE 1: WHO GUIDELINES AND RECOMMENDATIONS FOR
THE POST-OPERATIVE OUTCOME OF CATARACT SURGERY
WITH IOL42
GRADE V/A UCVA BCVA
GOOD 6/6-6/18 80% 90%+
BORDERLINE <6/18-6/60 15% <5%
POOR <6/60 <5% <5%
Various studies different parts of world have been published on the
visual outcome of MSICS, comparing with ECCE and
Phacoemulsification. They have proved that MSICS provides better result
than ECCE and comparable results with Phacoemulsification.
Hennig A, et al52 study reported an uncorrected good visual acuity
(≥6/18) in 76.8% of cases at discharge, which declined to 70.5% at
6-weeks and 64.9% at 1-year follow-up. The best corrected good visual
acuity (≥6/18) was found in 96.2% at 6-weeks and in 95.9% of cases at
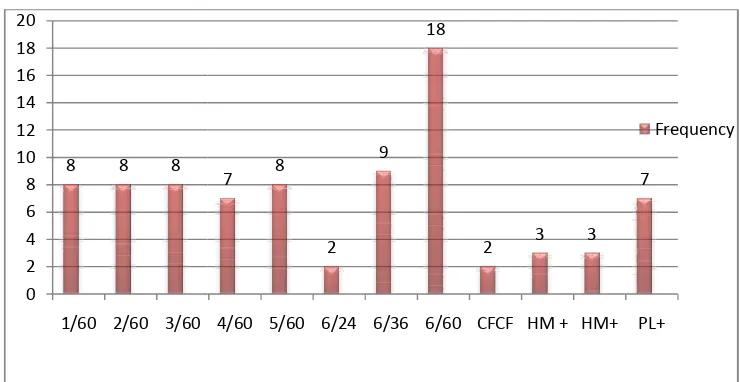
[image:27.612.122.558.276.404.2]Khan M T, et al15 study reported an un-corrected good visual acuity
(≥6/18) in 64% of cases at discharge and in 66.3% of cases at 6-weeks.
The best corrected good visual acuity (≥6/18) in 80.6% of cases at
6-weeks follow-up.
Zaman M, et al46 study reported an uncorrected good visual acuity
(≥6/18) in 62.51% of cases at 1st post-operative day and in 93.40% of
cases at 6-weeks follow-up.
Venkatesh R, et al76 study reported uncorrected good visual acuity
(≥6/18) in 78.4% of cases and best corrected good visual acuity (≥6/18)
in 97.1% of cases on 40th post-operative day.
MSICS Versus ECCE
Gogate P M, et al17 is a randomized controlled study compared the
efficacy of manual small incision cataract surgery with conventional
ECCE. At 6-weeks follow-up in MSICS group 47.9% of cases had an
uncorrected visual good acuity (≥6/18) compared to 37.3% of cases in
ECCE group. Best corrected visual acuity in MSICS group was good
(≥6/18) in 89.8% of cases compared to 86.7% in ECCE group.1.1% of
cases in ECCE group and 1.7% of cases in MSICS group had
poor(<6/60). In spite of requiring similar equipments to ECCE gives
In a Cochrane review54, 55, and 56 of surgical interventions for age related
cataract Meta -analysis of two studies, Pune Study and George 2005 was
done to compare MSICS with ECCE. These studies have shown a
significantly better uncorrected visual acuity (≥6/18) and surgically
induced astigmatism in the MSICS group (47.9%) versus ECCE group
(37.3%), but no difference in BSCVA between the two groups.
Venkatesh R, et al49 study reported an uncorrected good visual acuity
(≥6/18) in 87.9% of cases. This study evaluated the efficacy of MSICS in
phacolytic glaucoma cases. The significance of this report lies in the fact
that phacolytic glaucoma is not an uncommon presentation in a
developing country like India49.
MSICS Versus PHACOEMULSIFICATION
Ruit S, et al64 study reported an uncorrected good visual acuity (≥6/18) in
89% of cases in MSICS group and in 85% of cases in the phaco group at
six months follow-up. The best corrected good visual acuity (≥6/18) was
reported in 98% of cases in both the MSICS and the phaco group. The
two groups showed no statistically significant difference in UCVA or
Venkatesh R, et al16 study reported an uncorrected good visual acuity
(≥6/18) in 82.0% of cases in MSICS group and in 87.6% of cases in the
phacoemulsification group at 6 weeks follow-up.
Singh S K, et al40 study compared the uncorrected visual acuity between
MSICS and phacoemulsification on the first post-operative day. The
study showed an uncorrected good visual acuity (≥6/18) in 77.7% of
cases in MSICS group and in 68% of cases in the phaco group.
Better vision on first post-operative day with MSICS can be correlated
with the greater increase in corneal thickness in the
phacoemulsification64. There is no statistically significant difference
between visual outcomes at 6 weeks follow-up16, 64.
In a Cochrane review54, 55, and 56 of surgical interventions for age related
cataract Meta -analysis of the two studies Gogate 2005 and George 2005
was done. This study reported that that the phaco group has a
significantly improved proportion of patients with an uncorrected good
visual acuity (≥6/18) in 81.1% of cases compared to MSICS group. But
SURGICAL-INDUCED ASTIGMATISM
Astigmatism means “without a point”. Miller Stephen J defined
astigmatism as a condition of refraction in which a point of light cannot
be made to produce image upon the retina by a correcting spherical lens1
Any ocular surgery with incisions placed on cornea and sclera will induce
astigmatism by altering the curvature of the refracting surface32. The
astigmatism induced by the surgical manoeuvring and the wound healing
is called surgically induced astigmatism. It is a major cause of functional
disturbance and insufficient uncorrected visual acuity20, 31.
Calculating the surgically induced refractive change is important in
evaluating the outcome of small incisions and various wound closures for
cataract surgery4.
The calculation and analysis of various techniques help to determine the
optimal wound size for a cataract surgery4.
With the advent of PCIOL, microsurgical instruments and microscope the
goal of cataract surgery has become the best and earliest possible visual
rehabilitation. Here the best possible vision means best uncorrected visual
acuity19. The biggest hurdle in this quest is the astigmatic component of
Incision location, length, configuration, closure technique, and
pre-existing astigmatism are some of factors that determine the post-operative
astigmatic error19, 18.
FACTORS RELATING TO INCISION
Self sealing scleral tunnel incisions are less likely to induce astigmatism
because of their posterior (external end) location, anterior corneal
(internal flap) location and the ‘blocking effect’ of the limbus on corneal
astigmatism induction19. The incidence of SIA is more in corneal
incisions because of their anterior location15.
The cataract wound tends to flatten the corneal meridian along which the
wound is centered6. The degree of flattening varies with the site, length
and is predictable to some degree7. Thus postoperative astigmatism can
be controlled by manipulating the site and size7.
Akura J, et al(2000) study evaluated the results of modifications of large
self-sealing incisions in minimizing the SIA7. The BENT (between nine
and twelve-o clock position) frown incision achieved the astigmatic
neutrality and incisions in steeper axis reduced SIA in all cases7.
Merriam J C, et al (2001) study compared the change in corneal
magnitude and duration of change depend on both length and location of
the incision33.
Gokhale N S, et al (2005) study evaluated the reduction in astigmatism in
MSICS through change in incision site. The SIA was found to be lower in
temporal and super-temporal group compared to superior group14.
Siddique M, et al (2009) study compared the SIA between different
incision sites. The study found that minimum and safe astigmatism is
achieved in temporal approach50.
Venkatesh R, et al (2009) study compared SIA of superior approach with
temporal approach. The study reported 1.08 D in superior and 0.72 D in
temporal group76.
Pawar V S, et al (2012) study compared postoperative astigmatism in
different location and same sizes were compared32. The SIA of temporal
and supero-temporal group was found to be the least32.
Malik V K, et al (2012) study compared the astigmatism in MSICS with
superior and temporal approach. The temporal approach had the lesser
SIA than that of superior65.
Buzard K A, et al (1991) study found no statistically significant
difference in the induced astigmatism between the horizontal suture
Phacoemulsification is considered superior to manual small incision
cataract surgery due to the smaller incision size and in amount of induced
astigmatism17.This disadvantage can be minimized by altering the
location and configuration as shown in various studies.
The difference in the amount of astigmatism when comparing the
different techniques is relevant in populations that have limited access to
spectacles54, 55, and 56
In a Cochrane review54, 55, and 56 of surgical interventions for age related
cataract Meta -analysis of two studies, Pune Study and George 2005 was
done to compare MSICS with ECCE. The SIA was found to be lower in
MSICS compared to ECCE due to Sutureless wound.
In a Cochrane review54, 55, and 56 of surgical interventions for age related
cataract Meta -analysis of the two studies Gogate 2005 and George 2005
was done to compare MSICS with phacoemulsification. Even though
there was no difference in the average SIA between MSICS and PHACO,
significantly less number of patients had <1 D astigmatism in PHACO
group.
Many studies conclude that although phacoemulsification reduces
astigmatism better than MSICS at 6-weeks follow-up, there is no
The astigmatism induced in MSICS can be used to neutralize the
pre-existing astigmatism by changing the site of incision18, 65. But this method
has a limited effect in astigmatic reduction- with a maximum reduction of
around 1.00 to 1.50 diopters7.
COMPLICATIONS
MSICS is more difficult than conventional ECCE. The preparation of
optimum size scleral tunnel, handling of instruments, and removing of
nucleus all require better skill and additional training52. The manoeuvring
in the anterior chamber demands good dexterity and surgical skill47. Once
the technique is mastered the surgery is faster and the complication rate is
low52.
The principles of a good MSICS surgery are proper construction of the
scleral tunnel, minimal handling of tissues (cornea, iris), and preserving
the posterior capsule47.
The Oxford Cataract Treatment and Evaluation Team(OCTET) protocol
categorizes the intra-operative and post-operative complications into
three grades17.
Grade I: Trivial complications that may have needed medical
Grade II: Intermediate complications are that needed medical
intervention. They would have reduced the post-operative vision if left
untreated.
Grade III: Serious complications are that would have needed immediate
medical or surgical intervention. The interventions are a must to prevent
gross visual loss.
INTRAOPERATIVE COMPLICATIONS
• Related to the wound
Shallow tunnel - button holing
Deep tunnel-premature entry, iris injury, and bleeding
Iris prolapse –iris injury, chaffing
Shallowing of AC due to efflux of fluid through the wound
• Sphincter tear due inadequate mydriasis
• Iridodialysis
• Descement membrane stripping and tears
• Striate keratopathy
• Capsulotomy related
Too small – nucleus prolapse difficulty
• Difficulty in nucleus prolapse –inadequate Hydroprocedures
• Nucleus delivery difficulty due to large and hard nucleus
• Zonular disruption with or without vitreous loss
• Corneal endothelial damage
• Posterior capsular rent with or without vitreous loss
• Incomplete cortical wash- residual cortex at 12-o clock
• Failure to implant due to poor PC support
A complete pre-operative evaluation of individual cases allows the
surgeon to select the appropriate technique and plan the surgical
steps in advance. This ensures a good surgery and spares the
surgeon from unpleasant surprises on the table.
The management of intra-operative complication is made easier by
earlier identification and prompt action. A properly constructed
scleral tunnel incision prevents all the wound related
complication47.
Capsulorhexis of adequate size (>6mm) and Hydroprocedures will
ensure uneventful nucleus prolapse. The staining of anterior
capsule with Trypan blue helps in completing the capsulorhexis 49.
Inferior Iridodialysis is a unique complication of phaco sandwich
POST-OPERATIVE COMPLICATIONS17, 47
• Striate keratopathy
• Descement membrane folds
• Transient corneal edema
• Shallow AC
• Wound leak
• Hyphaema
• Iritis
• Residual 12-o clock cortex
• Vitreous in AC touching or not touching the cornea
• Pupillary block glaucoma
• Pupillary capture
• Malposition of IOL
• Deposits on IOL
• Posterior capsule opacification
• Cystoid macular edema
• Endophthalmitis
If the proper wound integrity is not maintained, shallowing of AC is seen
on first post-operative day. Whenever there is a doubt about the integrity
The corneal edema is usually transient and clears off within one week.
Excessive handling of iris will result in post-operative Iritis and cystoid
macular edema47.
Posterior capsular opacification can be prevented or delayed by good
cortical wash and polishing the capsule47.
MSICS is a safe surgery13, 17, 47. Various studies have shown that the
complication rate of MSICS is lower than ECCE and comparable to
phacoemulsification 13, 16, 40, 61, 62.
ADVANTAGES OF MANUAL SMALL INCISION CATARACT SURGERY IN INDIA
Blindness affects an estimated 12.5 million people in India, with cataract
contributing to 50-80% of this49. As the incidence increases with age the
cataract blindness burden will increase significantly due to greying of
population2. The increasing backlog of cataract blindness is the greatest
challenge in cataract surgery48.
To tackle this challenge we need is an efficient, high volume system
utilizing low cost, low technology procedure that can treat advanced
cataracts with minimal complication in the shortest amount of time 42, 48,
MSICS is considered as the most appropriate technique for performing
high-volume cataract surgery due to its efficiency, safety, shorter surgical
time and lower cost61.
Cataract surgery is considered to the most cost effective medical
intervention. Lansingh V C, et al (2007) determined the
cost-effectiveness of cataract surgery worldwide57. Phacoemulsification was
found to be costlier than either ECCE or MSICS. Since MSICS provides
better uncorrected visual acuity with the same cost, it is considered to be
the most appropriate procedure to tackle the backlog of cataract cases61.
The shorter surgical time of MSICS enhances the productivity of the
TEMPORAL MANUAL SMALL INCISION CATARACT
SURGERY
Temporal SICS is a type of manual small incision cataract surgery done
through temporal approach.
Cataract surgery is constantly evolving46. Cataract surgery has come a
long way from susrutha’s couching to phacoemulsification74. The
temporal approach was used in couching since it provided the better
access to the patient and the sitting arrangement of the surgeon in front of
the patient 74. The surgeon had to be ambidextrous to operate in both
eyes21.The site of incision shifted to superior when surgery was done with
the patient in supine position74.
With the invention of surgical microscope and intraocular lenses, modern
cataract surgery evolved into a refractive surgical procedure capable of
improving the best uncorrected vision19.
In the quest to achieve best possible post-operative vision, the cataract
surgeons improvised the technique by various modifications. One such
ADVANTAGES OF TEMPORAL APPROACH
VISUAL OUTCOME
Temporal incision is further away from the visual axis of the eye than the
superior incision. Any resulting corneal edema in postoperative period
will not affect the immediate visual rehabilitation. The wound
construction is done easily in deep sockets and small eyes32.Wound
healing is better in temporal incisions due to the absence of distractive
force of blinking33.Gravity will not interfere with the wound healing and
stability because the wound is parallel to the vector of forces32, 33.
Temporal incisions induce less SIA than superior because of the lesser
influence of lid and the extra ocular muscle7.The mean induced
astigmatism with temporal incisions is 0.75 D, whereas in superior
incisions it is 1.75 D75. Typical human cornea is 1mm wider in
horizontal meridian than the vertical meridian75. Thus the temporal
incisions are placed slightly away than the superior incisions33. Temporal
incisions cause less change in corneal curvature than comparable superior
incisions32. So the SIA is less in temporal incisions32. Temporal small
incision minimizes the senile against the rule astigmatism31, 37, and 45 by
COMPLICATIONS
The complication incidence is less in temporal manual small incision due
to various factors. It provides better access to instruments and thus
reduces the surgical time36.It is safe in brown and hard cataracts due to its
larger wound size. The larger size may induce more astigmatism, which
is overcome by its placement away from cornea. The temporal manual
small incision cataract surgery utilizes the similar steps in nuclear
management as that of phacoemulsification. The trauma to corneal
endothelial cells is minimal through temporal approach.
ADDITIONAL ADVANTAGES
The superior conjunctiva is left intact which can be used for
trabeculectomy in future, if needed32.Temporal approach cataract surgery
can be done on a eye with filtering bleb32.Temporal approach can be used
as a component in 2-site technique in combined surgery in treatment of
patients with cataract and primary open angle glaucoma9.
SURGICALLY INDUCED ASTIGMATISM
Even though it has been known that cataract incisions influence
astigmatism for long time, only for past 15 years the attention has been
given to the control measures of astigmatism 33, 77. The modern cataract
of correcting both the spherical and astigmatic components of
refraction19.
Some degree of naturally occurring astigmatic error is said to be present
in nearly 95% of eyes. The clinically significant astigmatism is reported
to occur in 7.5% to 75% of eyes77. The postoperative astigmatism greater
than 2 D occurs in 25 to 30% of eyes77.
The goal of refract cataract surgery has become the correction of
spherical component and eliminate the cylindrical component of
refractive error simultaneously. This is achieved by utilising the biometry
to predict the exact spherical component and by imparting the astigmatic
control measures19. The astigmatic control measures includes the wound
construction to attain least induced astigmatism and exploiting the
astigmatism inducing property of incision to correct the pre-existing
astigmatism18.
The scleral tunnel incisions provide a good control over the induced
astigmatism and faster wound stability34. The pre-existing astigmatism is
neutralized by placing the incision along the steeper axis18.
Senile cataract is most important cause of reversible blindness in India
astigmatism in the elderly population37, 45. The incision placement at the
steeper axis, the horizontal axis neutralizes the pre-existing error18.
Various studies have proved temporal scleral tunnels are less astigmatism
inducing than the superior tunnels due the minor changes in keratometry,
localised incision flattening, distance from the visual axis.
In patients with mature hard cataract and deep set eyes accessibility
becomes a major problem where temporal SCIS will be better. In
temporal SICS the superior conjunctiva is left undisturbed and can be
utilized for trabeculectomy if need arises. This is advantageous in a case
scenario where the patient has cataract surgery before developing
glaucoma because cataract occurs earlier in our country.
Phacoemulsification is considered to be the gold standard of cataract
surgery 100% phaco is neither practical nor feasible in our country. Even
the experienced phaco surgeons had to be bailed out and conversion to
MSICS gives better visual outcome than ECCE70. This conversion rate is
reported to be 3.7%.
Thus Temporal SICS is not so much as an alternative to
phacoemulsification and superior MSICS but is an additional technique in
the armamentarium. All three techniques are complementary to each
CASE STUDIES
Many studies have proven the advantage and efficacy of small incision
cataract surgery using temporal approach61.
A prospective randomized clinical trial of phacoemulsification versus
MSICS by Ruit S, Tabin G, Chang D, et al proved that MSICS by
temporal approach gave equally excellent visual outcome as
phacoemulsification. MSICS was significantly faster, less expensive and
less technology dependent than phacoemulsification64.
Singh V K, Winter I, Surin L, et al compared the safety and efficacy of
SICS with temporal approach and phacoemulsification. The study
concluded that SICS with rigid PMMA lens is a suitable technique to
treat immature cataract in developing countries40.
Kongsap P, et al compared Ruit technique was compared with the
modified Blumenthal technique and concluded that both have equal
visual outcomes, with low complication rates36.
Junejo S A, et al concluded that the Nonphaco Sutureless cataract
extraction through temporal approach ensures rapid visual recovery with
Malik V K, et al concluded that SICS with temporal approach provides a
better stabilization of the refraction with significantly less SIA compared
to superior approach65.
Siddique M, et al compared the visual outcome between superior and
temporal approach in MSICS and concluded that both are safe and
effective. Also the temporal approach provides better un-corrected visual
acuity and least and safe astigmatism50.
Zawar S V, Gogate P, studied the safety and efficacy of temporal manual
small incision cataract surgery in India. The study concluded that
temporal manual small incision cataract surgery gives excellent visual
outcome with minimal astigmatism and low complication rate at
economic cost.
Gokhale N S and Sawhney S study found that induced astigmatism was
lower in temporal and supero-temporal groups compared to that in
superior group14.
Pawar V S and Sindal D K compared the post-operative astigmatism in
small incision cataract surgeries with superior, super-temporal and
temporal incisions. The clinical study concluded that SICS with temporal
and super-temporal incisions provides better quality of vision due to a
AIM OF THE STUDY
The aim of the study is to
To evaluate visual outcome of Temporal Manual Small incision Cataract
Surgery
To evaluate the intra-operative complications and their management.
To evaluate the post-operative complications and their management.
To assess the visual rehabilitation of the patients after cataract surgery
MATERIALS AND METHODS
STUDY DESIGN
A prospective hospital based study
SETTING
The study was conducted at the Department of Ophthalmology,
Coimbatore Medical College Hospital.
DURATION OF STUDY
From October 2011 to September 2012
STUDY POPULATION
Adult patients in the age group between 45 to 70 years with senile
cataract who have been operated in the department of ophthalmology
CASE SELECTION
The cases were selected those cases who were operated on two days a
week, on the author’s theatre day. The following inclusion and exclusion
criteria were applied in case selection. Similarity between cases was
maintained as far as possible.
INCLUSION CRITERIA
Senile immature cataract
Senile hypermature cataract
Nuclear sclerosis 1-4
EXCLUSION CRITERIA
Cases that have not come for 6 weeks follow-up
Cases with pterygium
Cases with corneal pathology
Cases with very high astigmatism>2D
Cases with co-existing glaucoma
Cases with uveitis
Subluxated lens
Traumatic cataract
One eyed patients
STUDY DESIGN
Case selection is done using the above mentioned inclusion and exclusion
criteria. Demographic details of the cases were recorded.
All the cases were evaluated using the routine preoperative evaluation
protocol by the author. The protocol is as follows:
1. Visual acuity with pinhole
2. Intraocular pressure
3. Syringing of NLD
4. Ruling out of any foci of infection
5. Fundus examination (dilated pupil with IDO)
6. Slit lamp examination for nucleus grading
7. Keratometry
8. A Scan biometry
9. Blood pressure
10. Urine sample for sugar and albumin
11. Random blood sugar
All the selected cases were operated by a single surgeon, who is well
and in both approaches, superior and temporal. This is done to avoid the
compounding effect of the surgeon factor.
All were operated under peribulbar anaesthesia using 3ml of 2%
xylocaine with adrenalin 1:1000 dilution mixed with Bupivacaine. Two –
needle technique was used.
PERIBULBAR ANAESTHESIA
The adjective peribulbar refers to that location external to confines of the
four muscles and their intermuscular septa8. Local anaesthetic agents are
deposited within the orbit but do not enter within the geometric confines
of the cone of rectus muscles8. The intermuscular septum was incomplete
and permitted anaesthetic solution to spread into the cone8. Of the many
variations of technique a common one is two-needle technique. In this
first injection is given in inferior-temporal and the second in superior
nasal quadrant8. Up to 5ml of
Anaesthetic solution is given. Peribulbar block is safer than the traditional
retrobulbar anaesthesia as it avoids injury to optic nerve and extracular
muscles. Delayed onset of akinesia, requirement of greater volume of
anaesthetic solution leading to increased ocular pressure, periorbital
ecchymosis and conjunctival chemosis are the main complications of
SURGICAL TECHNIQUE
The position of the surgeon and the assisting staff is important in
temporal small incision cataract surgery. The surgeon was seated right
side of operating table for right eye cases and the assisting staffs were
placed at the head end. This positioning was changed accordingly in left
eyes.
Since this rearrangement was time consuming, the cases were selected in
such a way that one(R/L) sided cases were operated on one day.
Eyelid and surrounding area cleaned using povidone iodine solution and
draped with eye towel. A wire speculum applied and conjunctival
irriagation with povidone-iodine solution was completed.
Superior rectus bridle suture was not required, which saved time and
prevented any untoward injury to the muscle sheath.
A limited peritomy and light wet field cautery done.
CONFIGURATION OF THE INCISION
A 6-7 mm external scleral straight incision, 2mm behind the limbus was
created using an 11-blade. The depth of incision was ½ of scleral
The crescent blade was used to dissect the scleral lamellae and scleral
tunnel was created. The tunnel was extended 2mm into the clear cornea.
The internal opening of the sclerocorneal tunnel was made using 2.8 mm
keratome knife in a downward angle. By this angulation three plane of
the incision was maintained. A side port was created 90° away from the
tunnel.
CAPSULORHEXIS - CCC
The anterior chamber was filled with viscoelastic (2% hydroxyl propyl
methyl cellulose). The capsulorhexis of size more than 6mm was
completed using the bent 27-gauge needle. The internal lip of tunnel was
extended full length using blunt 3.2mm extending knife.
NUCLEUS PROLAPSE AND DELIVERY
Hydroprocedures were done and nucleus was prolapsed into the AC with
the bent 27-gauge needle. The viscoelastic material was filled in the AC
and the nucleus was extracted with the phaco-sandwich technique.
Phaco-sandwich is a two-instrument technique. The prolapsed nucleus is
sandwiched between the vectis and iris spatula to deliver out. A
complication peculiar to this technique is inferior Iridodialysis.
CORTICAL WASH AND IOL IMPLANTATION
A complete cortical wash was done using simcoe irrigation aspiration
cannula. Viscoelastic material was injected into AC and the capsular bag
was inflated.
The rigid 6.5mm PMMA IOL was implanted in the capsular bag. The
visco elastic material was removed by irrigation and aspiration with
Simcoe cannula.
WOUND CLOSURE
The wound was closed with inflating the AC with ringer lactate solution
via the side port. The self-sealing nature of wound was checked at the end
of procedure. No sutures were applied and conjunctiva was opposed with
light cautery.
All the cases were given subconjunctival 0.5ml gentamycin and 0.5ml of
dexamethasone. Sterile pad and bandage was applied.
The intra-operative complications and the duration of surgery were
documented for all surgeries.
I POST-OPERATIVE DAY EVALUATION
1. Wound approximation
3. Slit-lamp examination - cornea, AC reaction, IOL position
and complications if any.
4. Fundus examination
All the patients were treated with topical ciprofloxacin and
dexamethasone eye drop every two hours on I post-op day.
The topical ciprofloxacin and dexamethasone eye drops six times
per day were given to all the patients for one week.
I WEEK FOLLOW-UP
1. Wound integrity
2. Visual acuity with pinhole
3. Slit lamp examination –cornea, anterior segment reaction, IOL
positioning, and complication if any.
The antibiotic steroid combination drug dose was tapered gradually to
twice per day in six weeks. Corneal edema and fibrinous uveitis are
treated medically.
6 WEEKS FOLLOW-UP
1. Visual acuity- best corrected vision
2. Refraction
4. Keratometry
5. Fundus examination
6. IOP measurement
Refraction was done after dilating and retinoscopy done using
plane mirror retinoscopy. Keratometry reading were recorded to
calculate the astigmatic change caused by the surgery. Bausch &
Lomb Keratometry and automated refractometry were used for
recording the keratometry values.
KERATOMETRY27
Keratometry is the optical method of determining the curvature of the
central cornea. Usually it is expressed as dioptric power (D) or as dioptric
curvature (Kd) of the cornea. The steepest and flattest curvatures act as
the principal meridians and the dioptric values associated with them are
called K readings.
Normally the K readings of the principal meridians are nearly of same
magnitude, 43D on average and usually within ±0.5D of one another. The
difference in K reading is defined as corneal astigmatism. The differences
more than 0.5D tend to indicate a significant amount of astigmatism,
Typically, there are three forms of regular astigmatism namely with- the-
rule, against-the-rule, and oblique astigmatism. The with-the-rule is most
common and against-the-rule is less common (except in older adults).
The oblique astigmatism is the least common.
The irregular astigmatism cannot be assessed perfectly with keratometry
alone, because of the distortion of the mire circle. The cases with
irregular astigmatism were ruled out during the case selection in the
present study.
A-SCAN BIOMETRY
It consists of entering K reading with ultrasonic measurement of axial
length. IOL power was calculated using SRK II formula.
METHODS OF STATISTICAL ANALYSIS
The tests used for analysis of this study are the t test and chi-square test.
The p value is calculated and less than .05 has been taken as significant.
Descriptive statistical analysis of this study was done. The measurements
are expressed in number as frequency and percentage.
The relationship between independent variables was analysed by
RESULTS AND OBSERVATIONS
The study entitled “A Prospective Clinical Study of Temporal Manual
small incision surgery” comprises of total 83 cases.
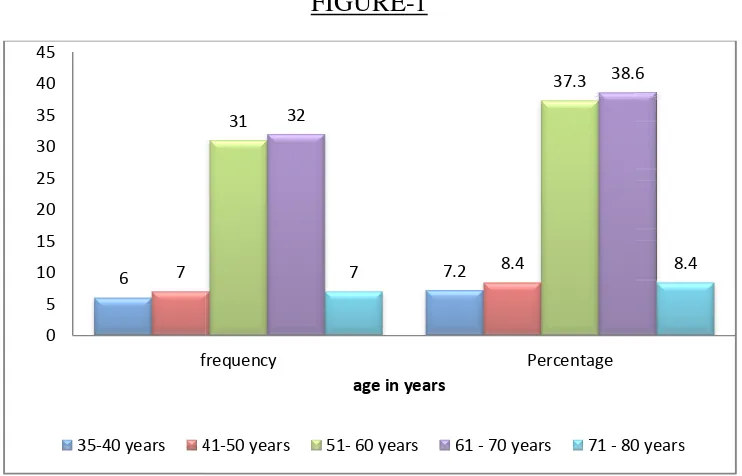
The age of the cases varies in range of 40 to 80 years. The majority (61%)
of cases were in the age group 50 to 70 years.
TAB – 2 : AGE GROUP
AGE FREQUENCY PERCENTAGE
35- 40 YRS 6 7.2
41-50YRS 7 8.4
51-60YRS 31 37.3
61-70YRS 32 38.6
71-80 YRS 7 8.4
The study group comprises of 53(63.9%) female patients and 30(36.1%) male patients. SEX MALE FEMALE TOTAL 6 7 0 5 10 15 20 25 30 35 40 45 frequency
[image:60.612.138.509.101.339.2]35-40 years 41
FIGURE-1
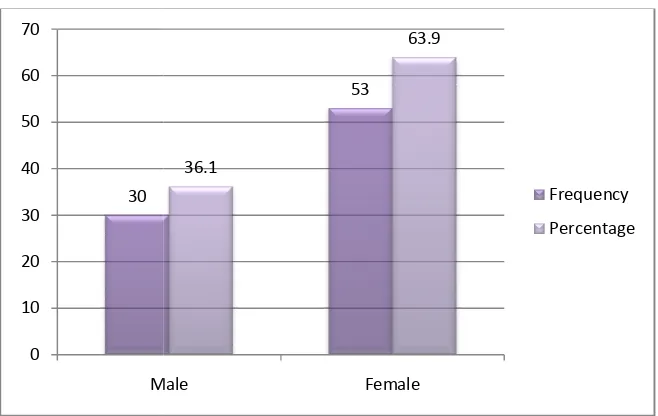
The study group comprises of 53(63.9%) female patients and 30(36.1%)
TAB- 3 : GENDER
FREQUENCY PERCENTAGE
30 36.1
53 63.9
83 100
7.2 8.4 31 37.3 32 38.6 7 frequency Percentage
age in years
41-50 years 51- 60 years 61 - 70 years 71 - 80 years
The study group comprises of 53(63.9%) female patients and 30(36.1%)
PERCENTAGE
38.6
8.4
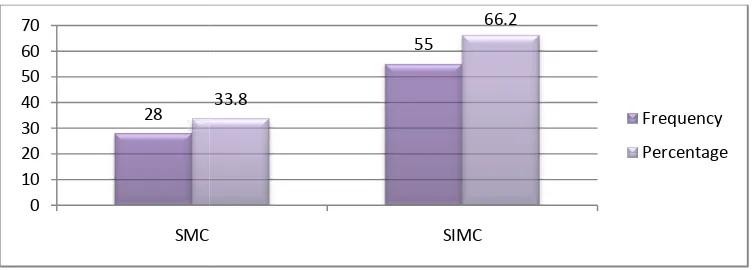
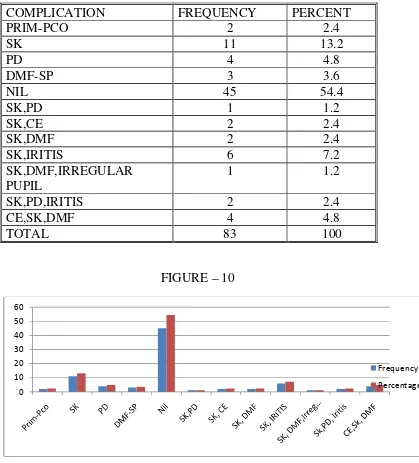
Among the 83 cases 28
immature cataract.
TAB 4
TYPE FREQUENCY
SMC 28
SIMC 55
TOTAL 83
[image:61.612.159.488.144.352.2]30 0 10 20 30 40 50 60 70 Male
FIGURE - 2
Among the 83 cases 28 were senile mature cataract and 55
TAB 4 : TYPE OF CATARCT
FREQUENCY PERCENTAGE
28 33.8
55 66.2
83 100
53 36.1 63.9 Male Female Frequency Percentage
55 were senile
Frequency
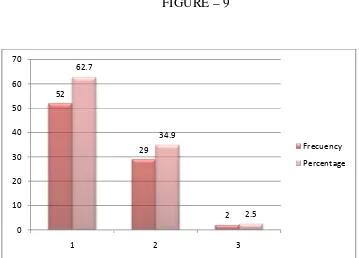
The hardness of the cataract was graded based on the colour of nucleus
under slit-lamp examination.
predominantly found the study group, 52 cases (62.6
found in 19 (22.9%) and grade IV in 12
[image:62.612.136.514.119.254.2]TAB NUCLEUS GRADE 2.00 3.00 4.00 TOTAL 28 0 10 20 30 40 50 60 70 SMC
FIGURE – 3
The hardness of the cataract was graded based on the colour of nucleus
lamp examination. Grade III nucleus sclerosis was
nantly found the study group, 52 cases (62.6%). Grade II was
in 19 (22.9%) and grade IV in 12 cases (14.5%).
TAB – 5 : GRADE OF NUCLEUS
NUCLEUS GRADE FREQUENCY PERCENTAGE
19 22.9%
52 62.6%
12 14.5%
83 100%
55
33.8
66.2
SIMC
The hardness of the cataract was graded based on the colour of nucleus
nucleus sclerosis was
%). Grade II was
PERCENTAGE
Frequency
The pre-operative visual acuity was poor <6/60 in
borderline in 11(14.5%). Among the 72 cases 15 of them had <1/60
[image:63.612.129.477.146.316.2] [image:63.612.137.507.501.692.2]vision. FIGURE 19 22.9 0 10 20 30 40 50 60 70 2
8 8 8
0 2 4 6 8 10 12 14 16 18 20
1/60 2/60 3/60
FIGURE - 4
operative visual acuity was poor <6/60 in 72cases (86.7%
14.5%). Among the 72 cases 15 of them had <1/60
FIGURE – 5 VISUAL ACUITY (PRE-OP)
52 12 62.6 14.5 3 4 Frequency Percent 7 8 2 9 18
2 3 3
4/60 5/60 6/24 6/36 6/60 CFCF HM + HM+
86.7%) and
14.5%). Among the 72 cases 15 of them had <1/60
Frequency
7
PL+
All the patients were operated by a singl
sclerocorneal tunnel incision
peribulbar anaesthesia was given to all cases.
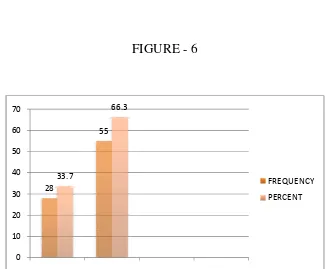
The size of the incision was either 6 or 6.5mm depending on the pre
operative evaluation. 55 cases (66.3%) had
the remaining 28 cases (33.7%) had a 6mm incision.
TAB SIZE(MM) 6 MM 6.5MM TOTAL 28 33.7 10 20 30 40 50 60 70
All the patients were operated by a single surgeon. The temporal
sclerocorneal tunnel incision was used in all cases. Two site technique of
peribulbar anaesthesia was given to all cases.
The size of the incision was either 6 or 6.5mm depending on the pre
operative evaluation. 55 cases (66.3%) had a 6.5mm scleral incision and
8 cases (33.7%) had a 6mm incision.
TAB-6: INCISION SIZE (MM)
FREQUENCY PERCENT%
28 33.7
55 66.3
[image:64.612.158.486.430.699.2]83 100
FIGURE - 6
55 66.3
FREQUENCY
PERCENT
e surgeon. The temporal
technique of
The size of the incision was either 6 or 6.5mm depending on the
pre-ral incision and
FREQUENCY
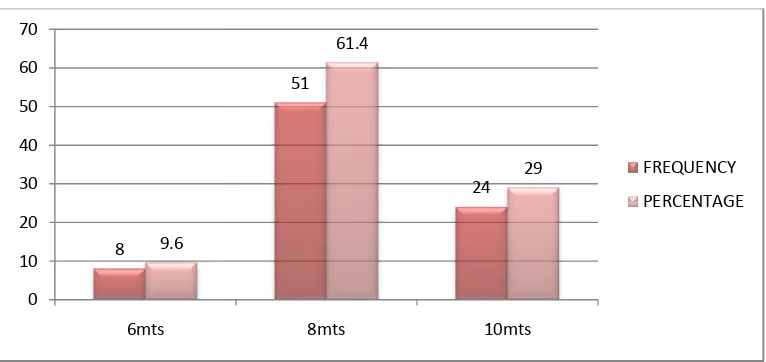
The duration of the surgery was recorded with a stop clock
51 cases (61.4%) were operated
completed in 10 minutes and 8 cases (9.6%) in 6 minutes.
to 10 minutes and average duration is 8.355 minutes.
TAB TIME (MINUTES) 6 8 10 TOTAL 8 9.6 0 10 20 30 40 50 60 70 6mts
The duration of the surgery was recorded with a stop clock and tabulated.
61.4%) were operated in 8 minutes.24 cases (29%) were
completed in 10 minutes and 8 cases (9.6%) in 6 minutes. It varies from 6
to 10 minutes and average duration is 8.355 minutes.
TAB – 7: DURATION OF SURGERY
MINUTES) FREQUENCY PERCENTAGE
8 9.6
51 61.4
24 29.0
[image:65.612.130.513.498.679.2]TOTAL 83 100
FIGURE - 7
51 24 61.4 29 8mts 10mts FREQUENCY PERCENTAGE and tabulated.
in 8 minutes.24 cases (29%) were
It varies from 6
AGE
FREQUENCY