Protocol for a randomised controlled trial of risk screening and early intervention comparing child- and family-focused cognitive behavioural therapy for PTSD in children following accidental injury
Full text
Figure
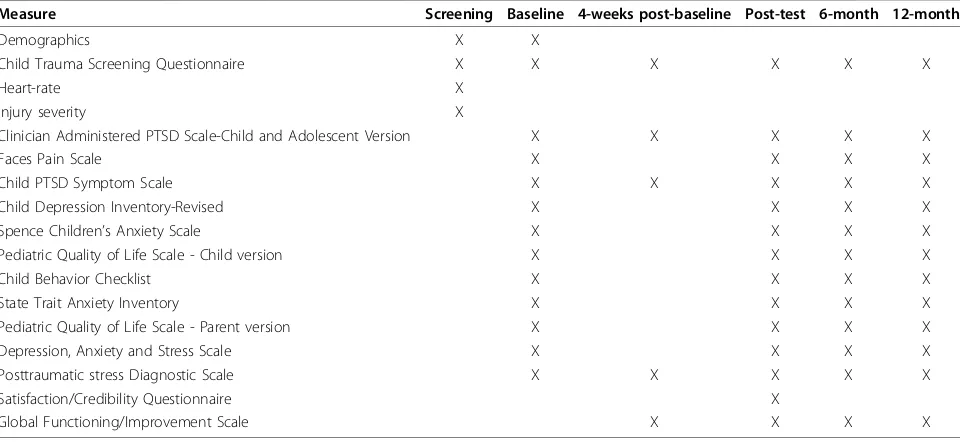
Related documents
The chapters in this volume of the Springer Proceedings in Mathematics & Statistics titled “Advances in Actuarial Sciences and Quantitative Finance” from the proceedings of
Our group attempted to apply NIR-PIT to the treatment of infectious diseases using IgY, which is inexpensive and available in large quantities, and to develop
The Regulation is consistent with the policy objectives of the Health Act 1937, Mental Health Act 2000, Public Health Act 2005, Public Health (Infection Control for
2 shows that metal weight decreases gradually when increasing the concentration of inhibitor in 1 M HCl solution at 30 ° C because the adsorption amount and coverage of inhi- bitor
It is comprised by phonetic awareness, phonics, fluency, vocabulary and text comprehension according to its different levels. a) Phonemic Awareness helps the students learn to
The aim of the study was to determine the epidemiological characteristics of bacterial meningitis observed in neonates born in the Department of Gynaecology and Obstetrics,
- Work and learn autonomously and plan and manage work time in the field of translation and linguistic mediation.. - Have and apply general knowledge in the field of translation