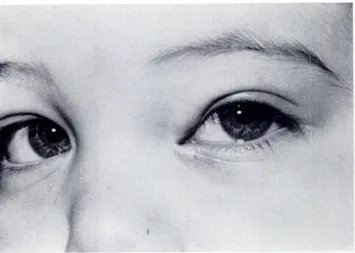
the successful treatment with intralesional corti-costeroid injections.
Intralesional
Corticosteroid
Injections
for
Infantile
Hemangiomas
of the Eyelid
Leonard
B. Nelson,
MD, Judith
E. Melick,
MD, and
Robison
D. Harley,
MD
From the Department of Pediatric Ophthalmology, Wills Eye Hospital, Philadelphia
ABSTRACT. Infants with capillary hemangiomas of the eyelid are at risk for amblyopia and strabismus. Several methods of treating these tumors have been associated with complications and limitations. The use of intrale-sional corticosteroid injections has been demonstrated to be a simple, safe, and effective method of treating capi!-lary hemangiomas of the eyelid. Pediatrics 1984;74:241-245; hemangiorna, corticosteroids, amblyopia, strabismus.
Capillary hemangiomas are benign tumors
corn-posed of proliferating endothelial cells and
anasto-mosing blood-filled channels.’ These tumors occur
in 1% to 2% of newborn children and are usually
of no particular significance.2 Commonly, a small
mass with an overlying red spot is noted shortly
after birth; this mass may grow rapidly during the
first 6 months of life.3 Resolution usually begins in
the second year of life and is complete in 60% of
cases by 4 years of age, and up to 76% by 7 years
of age.4 Redundant skin may remain and plastic
surgery may be required.
Infants with hemangiomas of the eyelid are at
risk for amblyopia and strabismus.5’6 Because of the
emotional, cosmetic, and functional implications of
these tumors around the eye, there is often tremen-dous parental pressure for surgical intervention.
The decision to intervene and the treatment
mo-dality remain controversial. Kushner7 reported
suc-cessfu! treatment of infantile adnexal hemangiomas
using intralesiona! corticosteroid injections. The
purpose of this paper is to alert the pediatrician to
the serious ocular sequelae that may develop from
capillary hemangiomas of the eyelid and to discuss
Received for publication Sept 2, 1983; accepted Nov 2, 1983. Reprint requests to (L.B.N.) Pediatric Ophthalmology Service, Wills Eye Hospital, Ninth and Walnut Streets, Philadelphia,
PA 19107.
PEDIATRICS (ISSN 0031 4005). Copyright © 1984 by the American Academy of Pediatrics.
CASE REPORTS
Case 1
This male patient was the product of a normal
full-term pregnancy. His eyelids appeared normal at birth, but at age 1 week, a mass appeared in the infant’s left upper eyelid; it grew rapidly during the next month.
The infant was first examined at 5 weeks of age. A 2
x 2-cm bluish mass with an overlying red mark involving the left upper lid partially occluded the visual axis. The mass increased in size with dependent positioning. The
infant fixated well with either eye. Retinoscopy findings included mild farsightedness with astigmatism in both eyes. Clinical diagnosis was that of a capillary heman-gioma.
Three weeks later the tumor had increased in size and completely occluded the visual axis (Fig 1). Five days later, while the infant was under general anesthesia, 80 mg of triamcino!one and 16 mg of dexamethasone sodium phosphate were injected into the tumor.
There was marked involution of the tumor beginning
the day after injection. By 1 week after the injection, the eyelid no longer occluded the visual axis.
By age 4 months, the patient had no further regression of the tumor. Injections of triamcinolone and dexameth-asone were repeated. The tumor further decreased in size.
At the 1-year follow-up, the child demonstrated normal fixation in both eyes and no change in the refractive error
of either eye (Fig 2).
Case 2
This male patient was the product of a normal full-term pregnancy. His eyelids appeared normal at birth,
but at age 1 week, a mass appeared in the medial position of the left upper eyelid; the mass grew rapidly during the next 5 weeks.
The infant was first examined at 3 months of age. A 1.5 x 1.5-cm bluish mass on the medial position of the left upper lid partially occuded the visual axis. The infant
4,
) ..
.
.
-t
‘
,#{188}
-:
Fig 2. Following second intralesiona! corticosteroid injection, capillary hemangioma no longer occludes visual axis.
_4_
Fig 1. Eight-week-old infant with capillary hemangioma of left upper lid occluding visual axis.
mild farsightedness with an astigmatic error of the left
eye. The infant was started on a 5-week course of oral prednisone: 5 mg, three times per day, for 2 weeks; 5 mg
twice a day for 1 week; 5 mg daily for 1 week, and finally, 2.5 mg daily for 1 week. Two weeks after institution of corticosteroid therapy, the size of the lesion was reduced to 1 x 1 cm. However, the child had developed a cush-ingoid appearance after 1 month ofprednisone treatment. The cushingoid appearance disappeared approximately 6
weeks. after prednisone t reatment was terminated.
During the next year, there was a slow increase in the
size of the hemangioma with partial occlusion of the pupillary space nasally (Fig 3). The astigmatic error of
the left eye was unchanged. At age 2 years, while the patient was under general anesthesia, 40 mg of triamcin-olone and 8 mg of dexamethasone sodium phosphate were
t..
.
.
.-.
.‘.t
Fig 3. Partial occlusion of pupillary space.
Fig 4. Six months following intralesional resolution of hemangioma.
follow-up examination revealed a normal level of the left upper lid with complete resolution of the hemangioma (Fig 4); however, the astigmatic error of the left eye did not lessen significantly.
DISCUSSION
Numerous authors have reported a high rate of
ocular complications from capillary hemangiomas
corticosteroid injection, there is complete
of the eyelid and have expressed the importance of
early therapy to prevent these complications. Haik
and co-workers6 found an 80% complication rate in 50 children followed over a 5 year period. These complications included amblyopia (60%), skin
changes (50%), strabismus (34%), residual
propto-sis (30%), orbital-palpebral asymmetry (16%),
(2%). In a study3 of 51 infants and children with capillary hemangiomas of the eyelid, visual
compli-cations occurred in 27 patients; the most common
complications were amblyopia (43%) and
strabis-mus (33%).
Robb5 detected asymmetric refractive errors
as-sociated with hemangiomas of the eyelids and orbit
in 46% of 37 children. These induced refractive
errors tended to remain despite eventual resolution
of the hemangioma. This finding supports the
im-portance of early therapy in the treatment of
sig-nificant eyelid capillary hemangiomas.
The factors that influence the decision
concern-ing therapy include: (1) tumor location and size
that cause significant disfigurement, (2) obscura-tion of the visual axis or tumor-induced refractive
changes entailing risk of amblyopia, (3) presence of
marked proptosis, and (4) parental appeals, which
require a careful explanation of the rationale for
treatment and anticipated results.
Several methods of treating adnexal
heman-giomas have been associated with complications
and limitations.’#{176} Even as recently as 1978, Haik and co-workers6 concluded that “present treatment modalities do not appear to be achieving the desired goals of a good cosmetic appearance and functional
outcome.” Therapeutic modalities at that time
in-cluded (1) surgical excision, (2) radiation therapy, (3) systemic corticosteroids, (4) ligation of afferent vessels, (5) injection of sclerosing solutions, (6)
cryotherapy, and (7) radon seed implantation.
Surgical excision may be useful for lesions that
are small and well circumscribed. However, this
method can produce severe scarring as well as
ex-acerbate the innate growth tendency of the tumor.2
Cutaneous atrophy has been associated with
cryo-therapy and the use of radon seeds. Irradiation
therapy may cause cataracts and cutaneous
scar-ring. Sclerosing injections are unpredictable and
also may produce scarring and pain. Systemic
cor-ticosteroids can be an effective way of treating
hemangiomas.9’3 However, not all hemangiomas
respond to systemic corticosteroids, and those that
do respond may show rebound growth as soon as
therapy is discontinued.’2 Complications associated with systemic corticosteroid administration include
growth delay and cushingoid characteristics.
Addi-tionally, Gunn and co-workers’4 reported depressed
T-cell counts in infants treated with systemic
steroids and suggested that these infants may be predisposed to an increased incidence of infection.
In 1979, Kushner’5 used intralesional
cortico-steroid injections in the treatment of adnexal
he-mangiomas and reported favorable responses in
three of four children. Zak and Morin’6
subse-quently reported two patients with upper eyelid
hemangiomas who were successfully treated by
lo-cal injection of corticosteroids. It is interesting to
note that in 1967, Zarem and Edgerton11 reported
in an addendum to their article that two patients
who had been given intralesional injections of pred-nisolone had demonstrated reduction in the size of the hemangioma.
Kushner7 has subsequently reported the results
oftreatment often patients (including four patients
reported in 1979) with adnexal hemangiomas
utiliz-ing intralesional injection of corticosteroids. A
marked and lasting regression of the hemangioma
occurred in eight of ten patients; one patient had a
moderate response. The corticosteroid treatment
proved effective in preventing amblyopia in infants
who had large hemangiomas that occluded the
vis-ual axis and often resulted in a reversal of the
cornea! astigmatism induced by these tumors. No
complications were reported from this therapy. In our patients, the intralesional corticosteroids
(triamcinolone and dexamethasone sodium
phos-phate) were injected in several different areas of
the tumor mass so as to distribute the medication
more evenly. We selected these two drugs in order
to combine the rapid action of dexamethasone
so-dium phosphate with the prolonged action of
tn-amcinolone as advocated by Kushner.7 We
necom-mend 80 mg of tniamcinolone and 16 mg of
dexa-methasone sodium phosphate as the initial dose for
large tumors. For smaller tumors and for repeated
drug injections, half the recommended dose is
in-dicated.
We observed changes in the tumor size within 1
week after injection. Involution of the tumor
grad-ually slows down but may continue for 2 to 3 months. Repeated drug injections may then be
con-sidered at that time. Neither of our patients
devel-oped any systemic complications. The advantages
of intralesional corticostenoid injection in the
treat-ment of adnexal hemangiomas include: (1) ease of
administration, (2) lack of complications, (3) rapid
onset of action which may prevent the development of amblyopia on refractive errors, (4) treatment may
be repeated if necessary, (5) treatment can be
of-fered early in life, and (6) if treatment is unsuc-cessful, other management can still be tried.7
Although no local on systemic complications have
been reported with intralesional conticosteroid
in-jections, this technique does require general
anes-thesia. We perform these injections, which require
only a few minutes, under a nitrous
oxide-oxygen-halothane combination by mask without
intuba-tion.
The mechanism of action of corticostenoids on
hemangiomas may be secondary to a
ac-tion.7 Zarem and Edgerton” noted a minimal degree
of inflammatory reaction in hemangioma biopsy
specimens. Zweifach and co-workers’7 have shown
that corticosteroids increase vascular sensitivity to circulating vasoconstnicting drugs. Arteniolar
con-stniction and narrowing of the precapillary
sphinc-tens in hamster cheek pouches was produced by
daily intramuscular injections ofcortisone.’8 There-fore, increased sensitivity to physiologically
occur-ring vasoconstnictor agents could explain the
reso-lution of hemangiomas by local corticosteroid injec-tions.
If a child has an adnexal hemangioma that is
enlarging and possibly occluding the visual axis or
inducing a refractive error, then treatment is
mdi-cated. Early referral to an ophthalmologist for the
child with an adnexa! hemangioma is important so
that if treatment is necessary it can be started
before serious ocular complications arise.
ACKNOWLEDGMENTS
This work was made possible, in part, by a grant from Fight for Sight, Inc, of New York to the Fight for Sight Children’s Eye Center of Wills Eye Hospital.
REFERENCES
1. Walsh T, Tompkins V: Some observations on the strawberry nevus of infancy. Cancer 1956;9:896-904
2. Jakobiec FA, Jones IS: Vascular tumors, malformations and degenerations, in Duane TD, Jaeger EA (eds): Clinical
Oph-thalmology. Philadelphia, JB Lippincott, 1982
3. Stigmar G, Crawford JS, Ward CM, at al: Ophthalmic
sequelae of infantile hemangiomas of the eyelids and orbit.
Am J Ophthalmol 1978;85:806-813
4. Margileth AM, Museles M: Cutaneous hemangiomas in chil-dren.JAMA 1965;194:523-526
5. Robb RM: Refractive errors associated with hemangiomas of the eyelids and orbit in infancy. Am J Ophthalmol
1977;83:52-58
6. Haik BG, Jakobiec FA, Ellsworth RM, et al: Capillary hemangiomas ofthe lids and orbit: An analysis ofthe clinical features and therapeutic results in 101 cases. Ophthalmology
1979;86:760-792
7. Kushner BJ: Intralesional corticosteroid injection for infan-tile adnexal hemangiomas. Am J Ophthalmol
1982;93:496-506
8. Henderson JS: Orbital Tumors, ed 2. New York, Brian C Decker, 1980, p 117
9. Fost NC, Esterly NB: Successful treatment of juvenile he-mangiomas with prednisone. J Pediatr 1968;72:351-357 10. Hiles DA, Pilchard WA: Corticosteroid control of neonatal
hemangiomas ofthe orbit and ocular adnexa. Am J
Ophthal-mol 1971;71:1003-1008
1 1. Zarem HA, Edgerton MT: Induced resolution of cavernous hemangiomas following prednisolone therapy. Plast Re-constr Surg 1967;39:76-82
12. Katz HP, Askin J: Multiple hemangiomata with thrombo-penia. Am eJDis Child 1968;115:351-357
13. deVenecia G, Lobeck CC: Successful treatment of eyelid hemangioma with prednisone. Arch Ophthalmol
1970;84:98-102
14. Gunn T, Reece ER, Metrakos K, et al: Depressed T cells following neonatal steroid treatment. Pediatrics
1981;67:61-67
15. Kushner BJ: Local steroid therapy in adnexal hemangioma.
Ann Opthalmol 1979;11:1005-1009
16. Zak TA, Morin JD: Early local steroid therapy of infantile eyelid hemangiomas. J Pediatr Ophthalmol Strabismus
1979;18:25-27
17. Zweifach BW, Shorr E, Black MM: The influence of the adrenal cortex on behavior of terminal vascular bed. Ann NYAcad Sci 1953;56:626-633
18. Wyman LC, Fulton GP, Shulman MH: Direct observations on the circulation in the hamster cheek pouch in adrenal insufficiency and experimental hypercorticalism. Ann NY