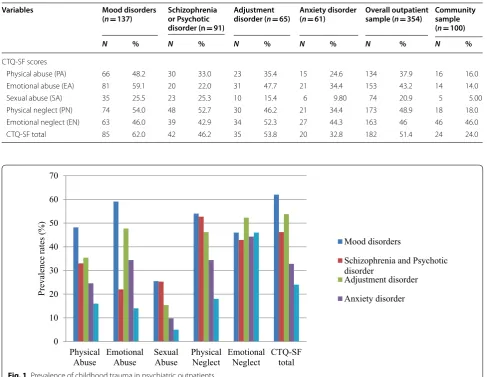
The prevalence of childhood trauma in psychiatric outpatients
Full text
Figure
Related documents
The main hypothesis of the study was to evaluate the percentage, duration, and reasons of complete eden- tulousness in relation to age and gender in rural and urban areas of
If You, Your Family Member(s), the Physician, or another Physician, as appropriate, wishes to request coverage for Prescription Drugs or Related Supplies for which Prior
For Cohen, but not for Rawls, the Difference Principle has both an indirect application (to choices required by the rules that qualify for inclusion in a just basic structure) and
Tarazaga, Distance matrices and regular figures, Linear Algebra Appl. Heiser, Theory of multidimensional scaling,
Shortened order-to-delivery cycle times Improvement in demand driven operations Increase in supply chain efficiency of 10% or greater Better customer and supplier relationships
cDNA: complementary DNA; CFSE: carboxyfluorescein succinimidyl ester; EGFR: epidermal growth factor receptor; EGR1: early growth response 1; FBS: fetal bovine serum; FPRL1:
As customary, all groups in the parish are invited to march in the procession, including the Feast Committee, the Holy Ghost Committee, the Holy Rosary Committee, the
In Aberfeldy continue through on to Bank Street and turn right on to Mill Street with the access to the private parking area being located on your right. POSTCODE PH15 2BB