Assessment of postoperative fracture healing, trauma degree and
neurological functional recovery in thoracolumbar burst fracture
patients with or without screw placement in injured vertebra
Zeng-Feng Du
, Qiang Zhu, Xiao-Lei Ma, Yao-Yao He, Zhi-Yuan Ma, Chun-Tang Xue
Orthopedics Department No. 1, the First Hospital of Yulin Shaanxi Province, Yulin City, Shaanxi Province, 718000
Journal of Hainan Medical University
http://www.hnykdxxb.com/
ARTICLE INFO ABSTRACT
Article history:
Received
Received in revised form Accepted
Available online
Keywords:
Thoracolumbar burst fracture Short-segment pedicle screw fixation Screw placement in injured vertebra Spinal cord injury
Neurological function
Corresponding author: Zeng-Feng Du, Orthopedics Department No. 1, the First
Hospital of Yulin Shaanxi Province, Yulin City, Shaanxi Province, 718000. Tel: 13772944536
Fund Project: Science and Technology Project of Shaanxi Province NO: SX-4213-BBX.
1. Introduction
Thoracolumbar burst fracture is one of the common orthopedic traumatic diseases, the traffic accidents, falling from height and injury by heavy object are the common causes of thoracolumbar burst fracture, that will cause spinal anatomical structure destruction and loss of vertebral stability, and severe cases can even cause spinal cord injury. The goal of clinical treatment of thoracolumbar burst
fracture is to correct spinal deformity, restore spinal stability and farthest protect spinal cord function[1,2]. Posterior pedicle screw fixation is the first choice for thoracolumbar burst fracture surgery, and has the advantages such as ideal surgical field exposure, simple operation steps and less blood loss[3]. Short-segment pedicle screw placement in two adjacent injured vertebral bodies is a common way of posterior pedicle screw fixation, it can keep the spinal motion function to a certain extent, but the fixation strength is relatively low[4]. In recent years, some scholars put forward that screw placement in injured vertebra at the same time of posterior short-segment pedicle screw fixation can increase the fixation strength[5], but the trauma degree and long-term neurological functional recovery have not been reported yet. In the following study, the
Objective: To study the postoperative fracture healing, trauma degree and neurological functional recovery in thoracolumbar burst fracture patients with or without screw placement in injured vertebra.Methods: Patients with single-segment thoracolumbar burst fracture who received posterior short-segment pedicle screw fixation in our hospital between May 2012 and December 2014 were selected as the research subjects and divided into screw placement group (group A) and no screw placement group (group B) according to the screw placement in injured vertebra or not, fracture healing was followed up, the injured vertebral anterior height and Cobb's angle were measured, and serum pNF-H, HSP70, NSE, S100β, GFAP, IL-1β, IL-6, IL-8, IL-10, TNF-毩 and MPO content of determined 3 d after operation. Results:
postoperative fracture healing, trauma degree and neurological functional recovery in thoracolumbar burst fracture patients with or without screw placement in injured vertebra were analyzed.
2. Subjects and methods
2.1 Research subjects
Patients with single-segment thoracolumbar burst fracture who received posterior short-segment pedicle screw fixation in our hospital between May 2012 and December 2014 were selected as the research subjects, and all patients were with clear history of trauma, diagnosed with single-segment thoracolumbar burst fracture by imaging examination after admission, with complete
medical records and followed up for ≥ 12 months. The following
cases were excluded: (1) patients with open fractures; (2) patients with pathological fracture; (3) patients complicated with fracture of the limbs, pelvis and other parts; (4) patients with osteoporosis; (5) patients lost to follow-up. A total of 74 patients were included and divided into screw placement group (group A) and no screw placement group (group B) according to the screw placement in injured vertebra or not during posterior short-segment pedicle screw
fixation. Group A included 34 cases, they were (36.8±5.2) years old,
22 cases were male and 12 cases were female, 21 cases were with thoracic vertebral fracture and 13 cases were with lumbar vertebral
fracture; group B included 40 cases, they were (38.1±4.8) years old,
25 cases were male and 15 cases were female, 26 cases were with thoracic vertebral fracture and 14 cases were with lumbar vertebral fracture. The two groups of patients were not significantly different in general information (P>0.05).
2.2 Operation methods
Both groups received posterior short-segment pedicle screw fixation under general anesthesia, and the method was as follows: patients took prone position, then a median incision was made to separate the skin, subcutaneous tissue and muscle step by step and then expose the injured vertebra and adjacent two vertebral bodies, group B received the placement of a total of 4 short-segment pedicle screws in the two vertebral bodies adjacent to the injured vertebra, group A received the placement of a total of 6 short-segment pedicle screws in the injured vertebra and two vertebral bodies, connecting rods were installed after the locations of screws were confirmed under perspective during operation, and then postural reduction or open reduction was adopted for anatomical reduction of fractured vertebral bodies under perspective, and the transverse connecting links were installed after the reduction was confirmed to be good. The two groups didn’t receive laminectomy or intervertebral fusion, the incision was rinsed, then negative pressure drainage was placed and the incision was closed step by step.
2.3 Follow-up of fracture healing
Before operation as well as 1 week, half a year and 1 year after operation, the thoracolumbar anterioposterior and lateral films as well as CT examination were conducted respectively, the anterior height of injured vertebra and adjacent vertebral bodies was measured, and the injured vertebral anterior height = measured value of injured vertebral anterior height / [(injured upper vertebral anterior height + injured lower vertebral anterior height)/2]; the vertical line of injured upper vertebral superior endplate line and the vertical line of injured lower vertebral inferior endplate line were drawn in sagittal view, and the included angle between two vertical lines was the Cobb’s angle.
2.4 Serum index detection methods
3 d after operation, 5 mL of peripheral venous blood was collected from the two groups and centrifuged to get serum, and enzyme-linked immunosorbent assay kits were used to determine phosphorylated neurofilament heavy (pNF-H), heat shock protein 70 (HSP70), neuron specific enolase (NSE), stellate-derived calcium-binding protein (S100β), glial fibrillary acidic protein (GFAP), interleukin 1β (IL-1β), IL-6, IL-8, IL-10, tumor necrosis factor-α (TNF-α) and myeloperoxidase (MPO) content.
2.5 Statistical methods
SPSS 17.0 software was used to input and process data, measurement data comparison between two groups at different points in time was by t test, measurement data comparison within same group at different points in time was by repeated measure analysis of variance and P<0.05 indicated statistical significance in the differences.
3. Results
3.1 Imaging findings of two groups before and after operation
were less than those of group B.
3.2 Fracture healing of two groups
Before operation, the injured vertebral anterior height and Cobb's angle were not significantly different between two groups (P>0.05). 1 week after operation, the injured vertebral anterior height of two groups were significantly higher than those before operation and Cobb's angle were significantly lower than those before operation (*P<0.05), and the injured vertebral anterior height and Cobb's angle were not significantly different between two groups (P>0.05); half a year and 1 year after operation, the injured vertebral anterior height of two groups were significantly higher than those before operation and Cobb's angle were significantly lower than those before operation (*P<0.05), but the injured vertebral anterior height were significantly lower than those 1 week after operation and Cobb's angle were significantly higher than those 1 week after operation
(&P<0.05), the injured vertebral anterior height of group A half a
year and 1 year after operation were significantly higher than those of group B and Cobb's angle were significantly lower than those of group B (#P<0.05).
Table 1.
Comparison of injured vertebral anterior height and Cobb's angle between two groups before and after operation.
Groups Operation n Injured vertebral anterior height Cobb’s angle
Group A Before operation 34 60.92±8.14 14.79±1.94
1 week after operation 34 92.32±10.52* 4.52±0.62*
Half a year after
operation 34 89.44±9.85*&# 5.48±0.77*&# A year after operation 34 87.91±10.18*&# 6.14±0.73*&#
Group B Before operation 40 61.33±8.97 14.95±2.32
1 week after operation 40 91.98±10.77* 4.58±0.57*
Half a year after
operation 40 84.58±9.14*& 6.36±0.81*& A year after operation 40 81.62±9.67*& 7.04±0.89*&
3.3 Serum content of inflammatory injury mediators
On the 3rd day after operation, analysis of serum content of
inflammatory injury mediators IL-1β, IL-6, IL-8, IL-10,
TNF-毩 and MPO between two groups was as follows: serum IL-1β, IL-6, IL-8, IL-10, TNF-毩 and MPO content of group A were not significantly different from those of group B. Differences in serum IL-1β, IL-6, IL-8, IL-10, TNF-毩 and MPO content were not statistically significant between two groups on the 3rd day after operation (P>0.05).
3.4 Serum content of spinal cord injury maker molecules
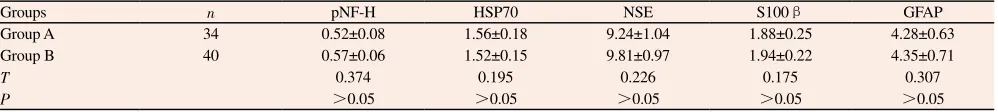
On the 3rd day after operation, analysis of serum content of spinal cord injury maker molecules pNF-H, HSP70, NSE, S100β and GFAP between two groups was as follows: serum pNF-H, HSP70, NSE, S100β and GFAP content of group A were not significantly different from those of group B. Differences in serum pNF-H, HSP70, NSE, S100β and GFAP content were not statistically significant between two groups on the 3rd day after operation (P>0.05).
4. Discussion
Posterior pedicle screw fixation is the main operation method for clinical treatment of thoracolumbar burst fracture, it uses pedicle screws to correct spine malformation and maintain the stability, and both long-segment pedicle screws and short-segment pedicle screws are the optional materials for posterior pedicle screw fixation[6]. Long-segment pedicle screw fixation is with exact effect, higher intensity and more fixation segments that can divide the stress on single screw, but the fixation way will affect the spinal motion segments and cause limited activities[7]. Short-segment pedicle screws need to be placed in two adjacent injured vertebral bodies in internal fixation, and the fixation reduces fixation segments, lessens surgical trauma and protects spinal motion segments; however, short-segment fixation is with smaller strength and excessive stress load on the screw, and the risk of postoperative loss of corrected height and angle, malformation recurrence as well as internal fixation screw
Table 2.
Comparison of serum content of inflammatory injury mediators between two groups.
Groups n IL-1β (ng/mL) IL-6 (pg/mL) IL-8 (pg/mL) IL-10 (pg/mL) TNF-毩 (ng/mL) MPO (pg/mL) Group A 34 9.38±1.07 19.49±2.24 16.78±2.18 38.59±5.14 4.59±0.67 9.16±1.07
Group B 40 9.14±0.95 20.14±2.51 17.05±1.95 39.04±4.89 4.62±0.81 9.45±1.15
T 0.375 0.119 0.247 0.417 0.148 0.648
P >0.05 >0.05 >0.05 >0.05 >0.05 >0.05
Table 3.
Comparison of serum content of spinal cord injury maker molecules between two groups (ng/mL).
Groups n pNF-H HSP70 NSE S100β GFAP
Group A 34 0.52±0.08 1.56±0.18 9.24±1.04 1.88±0.25 4.28±0.63
Group B 40 0.57±0.06 1.52±0.15 9.81±0.97 1.94±0.22 4.35±0.71
T 0.374 0.195 0.226 0.175 0.307
loosening and shifting significantly increases. In recent years, some scholars put forward that in short-segment pedicle screw fixation, vertebral plasty, screw placement in injured vertebra and other ways can be used together to enhance vertebral anterior column support, thus enhancing the strength of short-segment fixation[8,9].
At present, there is still no unified conclusion about the use of screw placement in injured vertebra during short-segment pedicle screw fixation, and the fracture healing of patients with and without screw placement in injured vertebra were analyzed in this study at first. Thoracolumbar burst fracture surgery aims to correct spine malformation and maintain the stability, the injured vertebral anterior height and Cobb's angle were measured to reflect the correction of the vertebral height and angle. The injured vertebral anterior height of two groups 1 week after operation were significantly higher than those before operation and Cobb's angle were significantly lower than those before operation, the injured vertebral anterior height half a year and 1 year after operation were significantly lower than those 1 week after operation and Cobb's angle were significantly higher than those 1 week after operation. This means that no matter the screws are placed in injured vertebra or not, both vertebral height and angle can be effectively corrected in a short time after operation, and different degrees of loss of vertebral corrected height and angle will happen in the long-term postoperative recovery process. Further analysis of the differences in vertebral height and angle correction half a month and 1 year after operation between two groups showed that the injured vertebral anterior height of group A half a year and 1 year after operation were significantly higher than those of group B and Cobb's angle were significantly lower than those of group B. This means that the screw placement in injured vertebra has more ideal fixation effect, and compared with no screw placement in injured vertebra, can reduce the loss of vertebral corrected height and angle.
The advantage of screw placement in injured vertebra is increasing fixation intensity and dividing the stress load on each screw after fixation without increasing fixation segments[10,11]. However, some scholars still hold conservative attitude towards screw placement in injured vertebra in short-segment pedicle screw fixation, and believe that screw placement in injured vertebra may increase the systemic trauma and spinal cord injury caused by operation. Systemic trauma caused by operation is characterized by the enhancement of inflammation and increased generation of inflammatory mediators. Interleukins are the important cytokines mediating inflammatory reaction, IL-1β, IL-6 and IL-8 have proinflammatory effect and they can promote the white blood cell differentiation, migration and infiltration; IL-10 has anti-inflammatory effect, can restrain the activation of a variety of inflammatory cells and the release of inflammatory mediators, and shows compensatory increase in the inflammatory response process. TNF-毩 mediates inflammatory tissue damage in inflammatory response process, and has promoting effect on cascade amplification of the inflammatory response[12,13]. MPO is a characteristic enzyme of neutrophils, exists
in the azurophilic granule and can reflect the degree of neutrophil infiltration[14]. In the study, analysis of serum levels of inflammatory mediators showed that serum IL-1β, IL-6, IL-8, IL-10, TNF-毩 and MPO content were not significantly different between two groups on the 3rd day after operation. This means that screw placement in injured vertebra during short-segment pedicle screw fixation will not increase the degree of trauma.
Activation of systemic inflammatory response not only reflects the increase of systemic trauma, but can also cause spinal cord injury through inflammatory mediators. In order to further clarify the differences in spinal cord injury between thoracolumbar burst fracture patients with and without screw placement in injured vertebra, serum content of spinal cord injury markers pNF-H, HSP70, NSE, S100β, GFAP were analyzed on the 3rd day after operation. pNF-H is the phosphorylated product of neurofilament heavy (NF-H) that is specifically expressed in nerve cells and has with anti-enzymolysis capacity and high stability[15]; HSP70 is a molecule in neurons and glial cells that inhibits the generation of oxygen free radical and promotes the restoration of antioxidant enzymes, and it shows compensatory increase in the process of spinal cord injury[16]; NSE is the catalyzing enzyme highly expressed in brain tissue, spinal cord tissue and peripheral ganglion, and it mediates glycolysis process; S100β is mainly expressed in glial cells and Schwann cells, and can regulate calcium ion homeostasis and signal transmission between inside and outside of cells[17]; GFAP is mainly expressed in astrocytes, and spinal cord injury can cause the reactive hyperplasia of astrocytes and increased generation of GFAP. In the study, the analysis of the above spinal cord injury molecule levels showed that serum pNF-H, HSP70, NSE, S100β and GFAP content were not significantly different between two groups of patients on the 3rd day after operation. This means that screw placement in injured vertebra in short-segment pedicle screw fixation will not increase the degree of spinal cord injury.
To sum up, screw placement in injured vertebra in posterior short-segment pedicle screw fixation treatment of thoracolumbar burst fracture can reduce the loss of vertebral height and kyphosis correction and improve long-term spinal nerve function without increasing the surgical trauma.
References
[1] Sait A, Prabhav NR, Sekharappa V, Rajan R, Raj NA, David KS. Biomechanical comparison of short-segment posterior fixation including the fractured level and circumferential fixation for unstable burst fractures of the lumbar spine in a calf spine model. J Neurosurg Spine 2016; 10: 1-8.
[2] Aono H, Tobimatsu H, Ariga K, Kuroda M, Nagamoto Y, Takenaka S, et al. Surgical outcomes of temporary short-segment instrumentation without augmentation for thoracolumbar burst fractures. Injury 2016;
47(6): 1337-1344.
RT, et al. Anterior corpectomy via the mini-open, extreme lateral, transpsoas approach combined with short-segment posterior fixation for single-level traumatic lumbar burst fractures: analysis of health-related quality of life outcomes and patient satisfaction. J Neurosurg Spine 2016;
24(1): 60-68.
[4] Javadi SA, Naderi F. The long-term efficacy of pedicular screw fixation at patients suffering from thoracolumbar burst fractures without neurological deficit. Asian J Neurosurg 2015; 10(4): 286-289.
[5] Li DP, Yang HL, Huang YH, Xu XF, Sun TC, Hu L. Transpedicular intracorporeal grafting for patients with thoracolumbar burst fractures.
Saudi Med J 2014; 35(1): 50-55.
[6] Vu TT, Morishita Y, Yugue I, Hayashi T, Maeda T, Shiba K. Radiological outcome of short segment posterior instrumentation and fusion for thoracolumbar burst fractures. Asian Spine J 2015; 9(3): 427-432. [7] Yaldiz C, Asil K, Ozkal B, Ceylan D, Kacira T. Thoracolumbar burst
fractures requiring instrumented fusion: Should reducted bone fragments be removed? A retrospective study. Neurol Neurochir Pol 2015; 49(6): 358-366.
[8] Liu Chao-jian, Cai La-jia, Shi Zhao-hong, Lin Jian-xiong. Posterior short-segment fixation with or without pedicle screw for treating thoracolumbar burst fractures. Orthopedic J China 2016; 24(6): 531-535. [9] Loibl M, Korsun M, Reiss J, Gueorguiev B, Nerlich M, Neumann C,
et al. Spinal fracture reduction with a minimal-invasive transpedicular Schanz Screw system: clinical and radiological one-year follow-up.
Injury 2015; 46(Suppl 4): 75-82.
[10] Eschler A, Ender SA, Schiml K, Mittlmeier T, Gradl G. Bony healing of unstable thoracolumbar burst fractures in the elderly using percutaneously applied titanium mesh cages and a transpedicular fixation
system with expandable screws. PLoS One 2015; 10(2): e0117122. [11] Schouten R, Lewkonia P, Noonan VK, Dvorak MF, Fisher CG.
Expectations of recovery and functional outcomes following thoracolumbar trauma: an evidence-based medicine process to determine what surgeons should be telling their patients. J Neurosurg Spine 2015;
22(1): 101-111.
[12] Tang P, Zhu R, Ji WP, Wang JY, Chen S, Fan SW, et al. The NLRP3/ Caspase-1/Interleukin-1β axis is active in human lumbar cartilaginous endplate degeneration. Clin Orthop Relat Res 2016; 474(8): 1818-1826. [13] Shen S, Guo J, Luo Y, Zhang W, Cui Y, Wang Q, et al. Functional
proteomics revealed IL-1β amplifies TNF downstream protein signals in human synoviocytes in a TNF-independent manner. Biochem Biophys Res
Commun 2014; 450(1): 538-544.
[14] Li H, Liu J, Yao J, Zhong J, Guo L, Sun T. Fracture initiates systemic inflammatory response syndrome through recruiting polymorphonuclear leucocytes. Immunol Res 2016; 64(4): 1053-1059.
[15] Ahadi R, Khodagholi F, Daneshi A, Vafaei A, Mafi AA, Jorjani M. Diagnostic value of serum levels of GFAP, pNF-H, and NSE compared with clinical findings in severity assessment of human traumatic spinal cord injury. Spine 2015; 40(14): 823-830.
[16] Sharma HS, Muresanu DF, Lafuente JV, Sjoquist PO, Patnaik R, Sharma A. Nanoparticles exacerbate both ubiquitin and heat shock protein expressions in spinal cord injury: neuroprotective effects of the proteasome inhibitor carfilzomib and the antioxidant compound H-290/51. Mol Neurobiol 2015; 52(2): 882-898.