White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/148032/
Version: Published Version
Monograph:
Mazzone, P. orcid.org/0000-0003-0944-8031, Carlton, J. orcid.org/0000-0002-9373-7663 and Griffiths, H. orcid.org/0000-0003-4286-5371 (2019) Summary vision screening data : Malawi. Report. Vision Screening Country Reports . EUScreen
©2019 EUScreen. For reuse permissions, please contact the publisher.
[email protected] https://eprints.whiterose.ac.uk/
Reuse
Items deposited in White Rose Research Online are protected by copyright, with all rights reserved unless indicated otherwise. They may be downloaded and/or printed for private study, or other acts as permitted by national copyright laws. The publisher or other rights holders may allow further reproduction and re-use of the full text version. This is indicated by the licence information on the White Rose Research Online record for the item.
Takedown
If you consider content in White Rose Research Online to be in breach of UK law, please notify us by
Summary Vision Screening Data: Malawi
Produced as part of Work Package 3
Paolo Mazzone1, Dr Jill Carlton2, Dr Helen Griffiths3
1. Research Assistant, School of Health and Related Research, University of Sheffield, United Kingdom (UK)
2. Senior Research Fellow, School of Health and Related Research, University of Sheffield, United Kingdom (UK)
3. Senior Lecturer, Academic Unit of Ophthalmology and Orthoptics, University of Sheffield, United Kingdom
(UK)
Information provided by
Wakisa Mulwafu, College of Medicine, University of Malawi - ENT Surgeon
&
Chatonda Manda, Lions Sight First Eye Hospital, Blantyre, Malawi -Paediatric Ophthalmologist
7th May 2019
Disclaimer: This is a summary report representing the responses from a country representative working within eye care services of the country reported. This report does not represent conclusions made by the authors, and is the product of professional research conducted for the EUSCREEN study. It is not meant to represent the position or opinions of the EUSCREEN study or its Partners. The information cannot be fully verified by the
ii
T E U H
and innovation programme under Grant Agreement No 733352
Contents
1. Glossary of Terms iii
2. Abbreviations vi
3. Population and Healthcare Overview 1
4. Vision Screening Commissioning and Guidance 3
5. Screening programme 4
5.1 Vision screening - Preterm babies 4
5.2 Vision screening - Birth to 3 months 4
5.3 Vision screening - 3 months to 36 months 4
5.4 Vision screening - 36 months to 7 years. 4
6. Automated Screening 9
7. Provision for Visually Impaired 10
8. Knowledge of existing screening programme 11
8.1 Prevalence/Diagnosis 11
8.2 Coverage 11
8.3 Screening evaluation 11
8.4 Treatment success 11
9. Costs of vision screening in children 12
9.1 Cost of vision screening 12
9.2 Cost of treatment for amblyopia 12
9.3 Cost of Treatment for strabismus 12
9.4 Cost of treatment for cataract. 12
iii Glossary of Terms
Abnormal test result
A
detected under good conditions. The result on screening equipment may indicate
Attendance rate The proportion of all those invited for screening that are tested and receive a result:
Invited for screening includes all those that are offered the screening test.
Tested and receive a result could be
Attendance rate provides information on the willingness of families to participate in screening.
Compliance with referral
(percentage)
The percentage of those who are referred from screening to a diagnostic assessment that actually attend the diagnostic assessment.
Percentage of compliance provides information on the willingness of families to attend the diagnostic assessment after referral from screening.
Coverage The proportion of those eligible for screening that are tested and receive a result:
Eligible for screening includes those within the population that are covered under the screening or health care programme.
T
diagnostic assessme
Factors such as being offered screening, willingness to participate, missed screening, ability to complete the screen, and ability to document the screening results will influence the coverage.
False negatives The percentage of children with a visual deficit (defined by the
Example: If 100 children with visual deficit are screened, and 1 child passes the screening, the percentage of false negatives is 1%.
False positives The percentage of children with normal vision that are referred from screening to a diagnostic assessment.
iv
Vision screening professional
A person qualified to perform vision screening, according to the practice in the country or region.
Inconclusive test result
A
detected due to poor test conditions or poor cooperation of the child.
Invited for screening
Infants/children and their families who are offered screening.
Outcome of vision screening
An indication of the effectiveness or performance of screening, such as a measurement of coverage rate, referral rate, number of children detected, etc.
Untreated amblyopia
Those children who have not received treatment for amblyopia due to missed screening or missed follow-up appointment.
Persistent amblyopia
Amblyopia that is missed by screening, or present after the child has received treatment.
Positive predictive value
The percentage of children referred from screening who have a confirmed vision loss.
For example, if 100 babies are referred from screening for diagnostic assessment and 10 have normal vision and 90 have a confirmed visual defect, the positive predictive value would be 90%.
Prevalence The percentage or number of individuals with a specific disease or condition. Prevalence can either be expressed as a percentage or as a number out of 1000 individuals within the same demographic.
Programme An organised system for screening, which could be based nationally, regionally or locally.
Protocol Documented procedure or sequence for screening, which could include which tests are performed, when tests are performed, procedures for passing and referring, and so forth.
Quality assurance A method for checking and ensuring that screening is functioning adequately and meeting set goals and benchmarks.
Referral criteria A pdetermined cut-off boundary for when achild should be re-tested or seen for a diagnostic assessment.
Risk babies / Babies at-risk
All infants that are considered to be at-risk or have risk-factors for vision defects/ophthalmic pathology according to the screening programme.
Two common risk factors are admission to the neonatal-intensive care unit (NICU) or born prematurely. However, other risk factors for visual defects may also be indicated in the screening
v
Sensitivity The percentage of children with visual defects that are identified via the screening programme.
For example, if 100 babies with visual defects are tested, and 98 of these babies are referred for diagnostic assessment and 2 pass the screening, the sensitivity is 98%.
Specificity The percentage of children with normal vision that pass the screening.
For example, if 100 babies with normal vision are tested, and 10 of these babies are referred for diagnostic assessment and90 pass the screening, the specificity is 90%.
Target condition The visual defect you are aiming to detect via the screening programme.
Well, healthy babies
vi
1. Abbreviations
ACT: Alternating Cover Test
BCVA: Best Corrected Visual Acuity
CT: Cover Test
EI: Eye Inspection
EM: Eye Motility
Fix: Fixation
GDP: Gross Domestic Product
Hir: Hirschberg test
NICU: Neonatal-intensive care unit
PM: Pursuit Movements
PPP: Purchasing Power Parity
PR: Pupillary Reflexes
RE: Retinal Examination
RR: Red Reflex Testing
VA: Visual Acuity
1
2. Population and Healthcare Overview
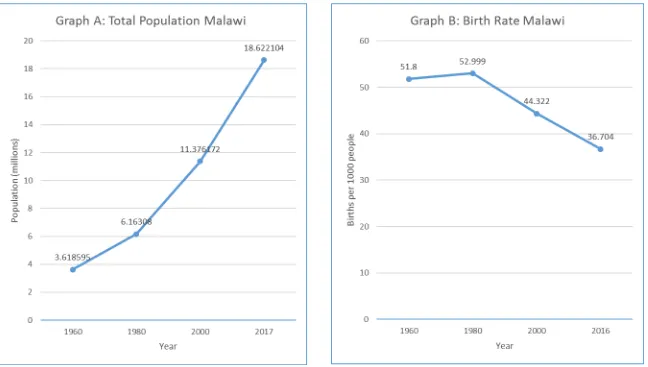
The population of Malawi is estimated as 18,622,104 (World Bank, 2018a) and birth rate estimated at 37 births/1,000 population in 2016 (World Bank, 2018b). The change in population and birth rate from 1960 to 2017 is shown in Figure 1, graphs A and B respectively.
Malawi had a reported population density of 197.52 people per square kilometre in 2017 and this has risen from 39.25 people per square kilometre in 1961 (World Bank, 2018c). Infant mortality in 2017 was estimated at 38.5 deaths/1,000 live births in total (World Bank, 2018d).
2
Figure 1: Change in the Total Population and Birth Rate in Malawi between 1960 and 2017
3
3. Vision Screening Commissioning and Guidance
The vision screening programme began in 2016, but only in the southern region of Malawi. Vision screening takes place in hospitals, private clinics and schools and is funded by the Ministry of Health. It is conducted by optometrists, ophthalmology residents and ophthalmologists. It is estimated that there are 30 vision screening professionals per million population. Nurses and teachers are listed as general professionals that do not screen, but could do so with additional training. However, there is no specific training available to perform vision screening.
Vision screening is not embedded into a general preventative child healthcare screening system. The current provision in the region described (Southern region) is decided upon by a paediatric ophthalmologist.
4
4. Screening programme
In Malawi, the target condition screened for by vision screening is amblyopia. The health care professionals delivering vision screening, venue for screening and tests used vary depending on the age of the child as shown in Tables 1, 2 and 3 respectively. Specific details of the screening offered within each age group are described more fully in sections 5.1 to 5.4 below.
5.1 Vision screening - Preterm babies
Preterm babies up to the age of 3 months are screened by a paediatric ophthalmologist. There is no established location of this vision screening, some take place in the eye department of a hospital but ideally it is completed in neonatal units, kangaroo units and under five units.
Screening is carried out in babies born with birth weight of less than 1.5kgs. Once in the
system, babies would be followed up using the ROP protocol. The tests conducted at this age
include eye inspection, fixation, red reflex testing, eye motility, Hirschberg test, retinal examination, pursuit movements and pupillary reflexes.
5.2 Vision screening - Birth to 3 months
Well, healthy babies up to the age of 3 months are screened by either a paediatrician or an ophthalmologist in a hospital or a private clinic at birth and 3 months of age. The tests conducted at this age include eye inspection and red reflex testing. Babies are referred for further diagnostic examination after 1 abnormal test result or 2 inconclusive test results.
5.3 Vision screening - 3 months to 36 months
Infants aged from 3 to 36 months of age are screened by an ophthalmologist in a hospital, preferably at 3 years of age, but this may vary. The vision screening tests conducted at this age include eye inspection, fixation, red reflex testing, eye motility, Hirschberg test retinal examination, pupillary reflexes, cover test and alternate cover test. There is no structured sequence to these tests. Infants are referred for further diagnostic examination after 1 abnormal test result or 2 inconclusive test results.
5.4 Vision screening - 36 months to 7 years.
Children aged from 36 months up to 7 years of age are screened by an ophthalmologist or an optometrist (visual acuity only) in either a hospital or school. The tests conducted at this age include eye inspection, fixation, red reflex testing, eye motility, Hirschberg test, pupillary reflexes, cover test, alternate cover test and visual acuity measurement. There is no structured sequence to these tests. Infants are referred for further diagnostic examination after 1 abnormal test result or 2 inconclusive test results.
5
6
Table 1: Healthcare professionals who conduct vision screening in each age group
Table 1 Paediatric Ophthalmologist
Ophthalmologist Paediatrician Optometrist
Preterm babies × × ×
0 to 3 months × ×
3 to 36 months × × ×
[image:13.842.77.770.120.453.2]7
Table 2: Vision screening tests used in vision screening for each age group
Table 2 EI EM Fix RR Hir RE PM PR CT ACT VA
Preterm
babies × × ×
0 to 3 months × × × × × × × × × ×
3 to 36
months ×
3 to 7 years ×
8
[image:15.842.79.769.101.394.2]Table 3: Location of vision screening for each age group
Table 3 Private Clinic Hospital School
Preterm babies ×
0 to 3 months ×
3 to 36 months × ×
9
5. Automated Screening
10
6. Provision for Visually Impaired
11
7. Knowledge of existing screening programme
8.1 Prevalence/Diagnosis
There is no data available concerning the prevalence of amblyopia, strabismus or congenital cataract.
8.2 Coverage
The percentage of children who are invited for vision screening is not known. It is not known who invites children for vision screening, or how this is done. The coverage of vision screening is estimated as 1% and attendance of these invited children to vision screening is estimated at less than 10%.
8.3 Screening evaluation
The number of false negative referrals and false positive referrals is not known. However, it
vision
screening is 0.95 and the specificity of vision screening is 0.90.
8.4 Treatment success
Optometrists and ophthalmologists are the only professionals that prescribe glasses to children under the age of 7 years. Other treatment options include patching and cataract surgery. Not all eligible children are treated due to payment problems relating to families having to pay for glasses.
12
8. Costs of vision screening in children
9.1 Cost of vision screening
The salary costs for vision screening professionals ranges from $200 (176 Euros*) for an optometrist, $300 for an Ophthalmology resident and $800 (705 Euros*) for a young ophthalmologist per year, ranging from $1.25 per hour to $5.00 per hour (1.10 - 4.40 Euros*). It is estimated that it costs $4,000 (3523 Euros*) to train general preventative child healthcare screening professionals, between leaving secondary education to qualification. The total screening costs for vision screening per year are estimated at $500 (440 Euros*) which is $2 (1.76 Euros*) per child. However, coverage is low.
9.2 Cost of treatment for amblyopia
The estimated costs of treating typical patients with refractive amblyopia is $80 (70 Euros*) for the glasses only. The estimated costs of treating typical patients with strabismic amblyopia is $100 (88 Euros*).
9.3 Cost of Treatment for strabismus
The estimated costs for strabismus surgery including follow up is $150 (132 Euros*).
9.4 Cost of treatment for cataract.
The estimated costs for congenital cataract surgery, including follow up of deprivation amblyopia, is $299 (263 Euros*).
13
9. References
The World Bank (2018a). Population, total | Data. [online] Available at: https://data.worldbank.org/indicator/SP.POP.TOTL?locations=MW [Accessed 25 February 2019].
The World Bank. (2018b). Birth rate, crude (per 1,000 people) | Data. [online] Available at: https://data.worldbank.org/indicator/SP.DYN.CBRT.IN?locations=MW [Accessed 25 February 2019].
The World Bank. (2018c). Population density (people per sq. km of land area) | Data. [online] Available at: https://data.worldbank.org/indicator/EN.POP.DNST?locations=MW [Accessed 25 February 2019].
The World Bank. (2018d). Mortality rate, infant (per 1,000 live births) | Data. [online] Available at: https://data.worldbank.org/indicator/SP.DYN.IMRT.IN?locations=MW [Accessed 25 February 2019].
The World Bank. (2018e). Life expectancy at birth, total (years) | Data. [online] Available at: https://data.worldbank.org/indicator/SP.DYN.LE00.IN?locations=MW [Accessed 25 February 2019].
The World Bank. (2018f). Death rate, crude (per 1,000 people) | Data. [online] Available at: https://data.worldbank.org/indicator/SP.DYN.CDRT.IN?locations=MW [Accessed 25 February 2019].