Active surveillance in patients with a PSA >10 ng/mL
Full text
Figure


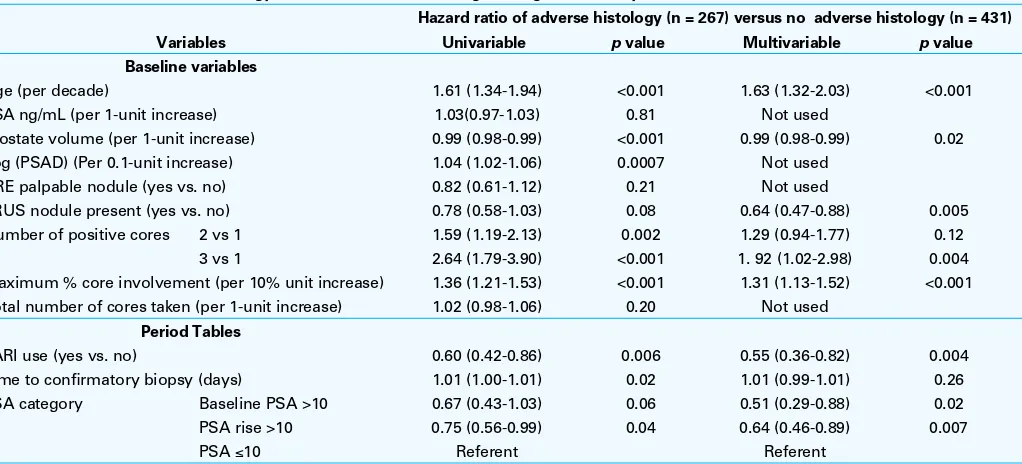

Related documents
My study employs semi-structured interviews – part of an ethnographic method as the main inquiry – together with multi-research methods: textual analysis, inductive
The findings related to the association of the knowledge scores of postmenopausal women with their selected sociodemographic variables shows that, there is a significant
world is Iran, where the national family planning program is "considered a model for developing nations and other Muslim countries" due to its success
Standardized scales were used by the researcher to assess the postmenopausal symptoms among the postmenopausal women i.e centre for menopausal rating scale
The results of this study are perceived ease of use and perceived usefulness has a significant positive effect on the interest of mobile banking users while
The overwhelming impact of the ban on plastic shopping bags on the subsistence marketplace of Ekondo Titi justifies inquiry into their coping strategies considering their
Kouachi, Existence of global solutions to reaction- diffusion systems with nonhomogeneous boundary conditions via a Lyapunov functional , Electronic Journal of
Software Platforms and Languages used in the proposed module are: Application Running on Raspberry Pi is developed using Python language, Web Application is developed
