1
Imaging recommendations in paediatric uroradiology: Minutes of the
ESPR workgroup session on urinary tract infection, fetal
hydronephrosis, urinary tract ultrasonography and voiding
cysto-urethrography
ESPR-Meeting, Barcelona/Spain, June 2007
Riccabona M.⁴, Avni FE.², Blickman JG.³, Dacher JN.
4, Darge K.
5, Lobo
ML.
6, Willi U.
7ESUR Paediatric guideline subcommittee and ESPR paediatric uroradiology
work group
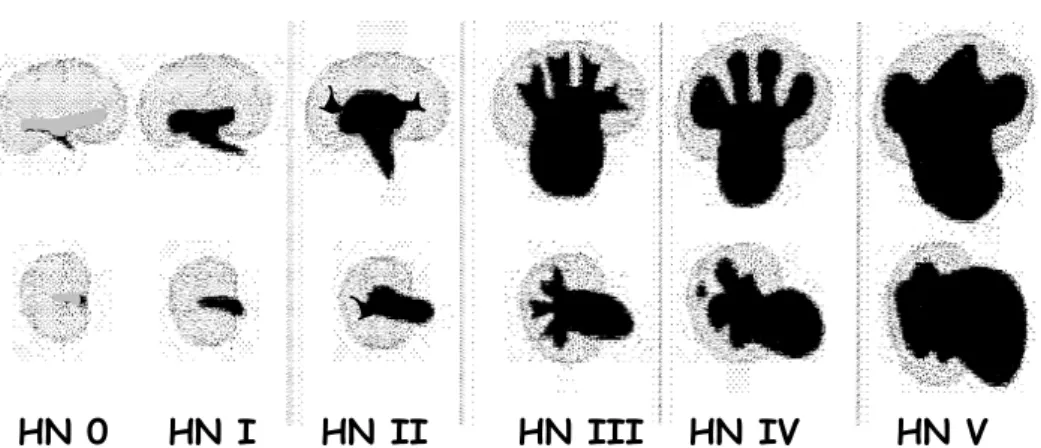
Table 1. Grading of Hydronephrosis (HN)
HN 0 HN I HN II
HN III HN IV HN V
HN 0 = no or minimal collecting system visible, considered normal
HN I = just the renal pelvis visible with an axial diameter less than 5-7 mm, usually considered normal
HN II = axial renal pelvis diameter less than 5/7-10 mm some calices with normal foniceal shape visible
HN III = marked dilatation of the renal calices and pelvis larger than 10 mm with reduced forniceal and papillar differentiation
without parenchymal narrowing
HN IV = gross dilatation of the collecting system with narrowing of the parenchyma (HN V = used in some places additionally, to communicate an extreme HN
with only a thin, membrane-like residual renal parenchymal rim) Neonatal / infantile hydronephrosis (HN) – US grading
3
Table 2
Abbreviations:
(a)CDS = (amplitude coded) colour Doppler sonography = power Doppler, ce-VUS = contrast-enhanced voiding urosonography, US = ultrasound, 3DUS = three-dimensional ultrasound
Procedural guideline: standard paediatric urosonography
well hydrated patient, full bladder, adequate equipment & transducer & training
…
urinary bladder: size (volume), shape, ostium, wall, bladder neck
include distal ureter & retrovesical space / inner genitalia
optional: CDS for urine inflow, perineal US, scrotal US …
post void evaluation
bladder: residual volume, bladder neck, shape & configuration kidneys: dilatation of pelvo-caliceal system / ureter changed
?
optional: (a)CDS & duplex-Doppler, …
kidneys: lateral and / or dorsal, longitudinal and axial sections parenchyma? pelvo-caliceal system?
standardised measurements in 3 axes & volume calculation
if dilated: + max. axial pelvis & calix, narrowest parenchymal width + uretero-pelvic junction
optional: ce-VUS, 3DUS …
Abbreviations:
CDS = colour Doppler sonography, aCDS = power Doppler, ce-VUS = contrast-enhanced voiding urosonography, HI = Harmonic Imaging, US = ultrasound, VUR = vesico-ureteral reflux
Procedural guideline:contrast-enhanced voiding urosonography (ce-VUS)
No diet restriction or enema, urine analysis …
Accepted indications: VUR-follow-up, girls, family screening, bedside Catheterism: feeding tube, 4-8 french, or suprapubic puncture
anaesthetic lubricant or coated plaste
Latex precaution: neuro tube defect, bladder exstrophy
Bladder filling with NaCl (only from plastic containers)
During + after voiding: US of bladder & kidneys
supine ± prone, sitting or standing
Peri-/ post-contrast US of bladder & kidneys
US modalities: fundamental, HI, CDS, dedicated contrast imaging alternate scans of right & left side during & after filling
US contrast medium, e.g., Levovist® - 300 mg/ml, 5%-10% of bladder volume slow, US-monitoring, potentially fractional administration
VUR diagnosis: echogenic micro-bubbles in ureters or renal pelves
5
Table 4
Abbreviations:
AB = Antibiotics, CM = contrast media, HN = hydronephrosis, PUV = posterior urethral valve, UT = urinary tract, UTI = urinary tract infection, VCUG = voiding cystourethrography, VUR = vesico-ureteral reflux
Preparations: no diet restriction or enema, urine analysis, after AB are completed …
Catheterism: feeding tube, 4-8 french or suprapubic puncture anaesthetic lubricant or coated plaster
Latex precaution: neuro tube defect, bladder exstrophy Bladder filling with radiopaque contrast
gravity drip = bottle 30-40 cm above table, watch dripping, AB?
After voiding: ap view of bladder & renal fossae
assess contrast drainage from kidney if refluxed
When voiding: remove catheter, unless cyclic VCUG = 3 fillings, 1st y (s) female: 2 spots of distended urethra (slightly oblique) male: 2-3 spots during voiding (ap & high oblique / lateral) include renal fossae during voiding, if VUR => spot film
Fluoroscopy: signs of increased bladder pressure, imminent voiding, urge bilateral oblique views of distal ureters, include catheter document VUR, include kidney (spot film, intra-renal reflux)
Note:VUR staging, minimise fluoroscopy time and spot films, no blind film
Fluoroscopic view of renal fossae & bladder, initial + early filling
Indications: febrile & recurrent UTI, particularly in infants, suspected PUV UT-malformation, HN > II° or “extended criteria”
Abbreviations:
ce-VUS = contrast-enhanced voiding urosonography, HN = hydronephrosis, IVU =
intravenous urography, MCDK = multicystic dysplastic kidney, MRU = magnetic resonance urography, US = ultrasound, VCUG = voiding cystourethrography
abnormal: pelvis ≥≥≥≥ 7 mm + dilated calyces, or other anomalies (HN > II°)*1 normal (≤ HN II°)
abnormal
USat 1 mo
US
at 3 mo
pelvis ≤ 10 mm
(≤ HN II°) pelvis > 10 mm, HN > II°
Stop follow-up
further morphological & functional evaluation: Scintigraphy, IVU, MRU
US
:
1st US around day 5 normal Stop follow-up abnormal normal pelvis ≥ 10 mm, HN > II° other malformation*2, “extended criteria” *1 VCUG *3prenatal US: mild or moderate dilatation = HN II + III
*1 use extended US criteria considering urothelial sign, kidney size & structure, etc …
*2 US genitography: in all patients with single kidney, MCDK, ectopic kidneys etc …
*3 ce-VUS can be used in girls and for screening populations…
7
Table 6
Abbreviations:
(a)CDS = (amplitude coded) colour Doppler sonography = power Doppler, (a)PN = (acute) pyelonephritis, CRP = C-reactive protein, CT = computed tomography, DD = differential diagnosis, DMSA = static renal scintigraphy, ce-VUS = contrast-enhanced voiding urosonography, MRI = magnetic resonance imaging, PCN = percutaneous nephrostomy, RNC = radionuclide cystography, Tb = tuberculosis, US = ultrasound, UTI = urinary tract infection, VCUG = voiding cystourethrography, VUR = vesico-ureteral reflux, XPN = xanthogranulomatuous pyelonephritis
recommended within first days, particularly in severe symptoms and in infants / neonates UTI *1 US + aCDS acute DMSA normal US no power Doppler or Doppler equivocal *2 clinically upper UTI
normal
• follow-up US
• VUR-evaluation
- always in infants - mostly in < 5 years + recurrent UTI in > 5 ys - VCUG in boys- ce-VUS in girls (if available) - for VUR follow-up
- ce-VUS or RNC (if available)
• late DMSA
after 6 - 12 months or (functional) renal MRI
• bladder function studies
> 6 years, urodynamics
*2 for DD=> MRI/CT Indications:
complicated stone disease (CT, un-enhanced scan) complicated UTI (XPN, Tb, abscess ...) question of tumour Pyo(hydro)nephrosis => PCN if no response to AB-treatment normal US clinically cystitis stop follow-up Pyelitis / Nephritis *2
aPN / scar / upper UTI
*1 UTI criteria:urine sample and blood count Leucocyturia, positive nitrite
positive culture (104 = catheter sample, 106 normal voiding),
Leucocytosis, elevated CRP
reliable clinical diagnosis essential = most important entry criteria for imaging!!
acute renal MRI?
Imaging algorithm in children with urinary tract infection (UTI)
if clinically clear + known normal urinary tract anatomy => no imaging? only delayed imaging for scaring in upper UTI?