Harvey C. Kaplan' Hillier L. Baker, Jr.' O. Wayne Houser' Edward R. Laws, Jr.2 Charles F. Abboud3 Bernd W. Scheithauer4
This article appears in the September/Octo-ber 1985 issue of AJNR and the December 1985 issue of AJR.
Presented at the annual meeting of the American Roentgen Ray Society. Las Vegas, April 1984.
'Department of Diagnostic Radiology, Mayo Clinic and Mayo Foundation, Rochester, MN 55905. Address reprint requests to H. L. Baker, Jr.
2 Department of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, MN 55905.
3 Division of Endocrinology, Metabolism and In-ternal Medicine, Mayo Clinic and Mayo Foundation, Rochester, MN 55905.
4 Department of Pathology, Mayo Clinic and Mayo Foundation, Rochester, MN 55905. AJNR 6:723-732, September/October 1985 0195-6108/85/0605-0723
© American Roentgen Ray Society
723
CT of the Sella Turcica after
Transsphenoidal Resection
of Pituitary Adenomas
A retrospective review of 120 patients undergoing transsphenoidal surgery for pitui-tary adenomas revealed that computed tomography (CT) was less sensitive and less specific than hormonal methods in identifying residual functioning adenomas, However, CT was the only useful method of evaluating nonfunctioning tumors, including pseudo-prolactinomas, Enlargement of the pituitary stalk, when seen on preoperative CT, was 100% predictive of "cure" if the enlargement returned to normal size on a remote follow -up scan (n
=
8) and was 100% predictive of residual tumor if the enlargement persisted or evolved (n = 8), Resolution of stalk displacement was the next most reliable predictor of cure (91%, n=
11), but persistent displacement was less reliable than abnormal intrasellar enhancement in predicting the presence of residual tumor (71%, n=
28, vs.81%, n
=
26). Enhancement in the postoperative sella by other than normal pituitary gland was presumed to be due to inflammation in 19% of patients. Inflammatory enhancement was observed in the presence of autograft and homograft muscle plugs and, unlike enhancement due to untreated tumors, was observed to decrease in size and intensity with time. Intrasellar enhancement was an unreliable criterion of success or failure in cases of microadenoma. All 14 patients with functioning adenomas and preoperative para sellar tumor extension had persistent tumor at postoperative evalua-tion. Of the 47 patients with resected functioning adenomas who had CT scans showing empty or partly empty sellas after operation, 22 (47%) had hormonally detectable residual tumor.During the last decade, advances in computed tomography (CT), transsphenoidal microsurgery, immunohistochemistry, and radioimmunassay have improved the
management of patients with pituitary adenomas. Radioimmunoassay of blood hormone levels has proved to be a more specific and sensitive indicator of the
presence or the persistence of functioning (endocrine hypersecreting) adenomas
after operation than CT [1] because the features of normal and abnormal
postop-erative CT often overlap. CT remains the most reliable method of evaluating nonfunctioning tumors. In this report, we compared CT in patients whose tumors were successfully resected with CT in patients who had residual or recurrent tumor
by independent hormonal criteria and determined the relative merit of CT findings so that they could be usefully applied to nonfunctioning tumors that had no hormonal markers. To date, very little has been reported on these subjects [2].
Materials and Methods
General
724 KAPLAN ET AL. AJNR:6, Sept/Oct 1985
Fig. 1. -120 cases were selected to match proportions of tumors in larger
surgical series to within 1% for ACTH and growth-hormone adenomas and 4% for prolactin and nonfunctioning adenomas. There were approximately equal numbers of cases of prolactin and nonfunctioning macroadenomas. One-third
of non functioning adenomas were pseudoprolactinomas.
8-82 years) were chosen so as to match (within 4%) the proportions of tumor types seen in the larger surgical series (fig. 1). The propor-tions of tumor types in our series closely match those reported by others [3]. Functioning tumors were present in 95 patients and nonfunctioning tumors in 25 patients. All 25 nonfunctioning tumors were macroadenomas (>1 cm), while 37 of the 95 functioning tumors were macroadenomas and 58 were microadenomas (~1 cm) (fig. 1).
Clinical
For the 95 patients with functioning tumors, cures and noncures could be identified by hormonal levels, with provocative tests used to further evaluate borderline cases. This methodology has been described [4-6]. Cure for the 25 patients with nonfunctioning tumors was based on CT criteria that were developed from cases with functioning tumors. Patients with obvious noncures could be further treated with irradiation or bromocriptine (or both), and those with Cushing disease could be treated with bilateral adrenalectomy [7].
Surgical
Exact details of the surgical procedure have been described else-where [8-10], but factors affecting the postoperative CT appearance are summarized below. After the tumor was removed, in order to promote hemostasis, stop cerebrospinal fluid leaks, and seal the sellar floor, 91 % of the sellae turcicae were packed with a plug of homograft muscle, 8% with an absorbable gelatin sponge (Gelfoam), and 1 % with homograft fat. The plugs were usually supported by a stent of nasal septal bone (87%), cartilage (12%), or acrylic bone cement (1 %). With macroadenomas, subarachnoid air was frequently introduced via a lumbar needle to prolapse the diaphragma sellae and the superior aspects of the tumor into the operative field. In 19 sellae, a surgical clip was placed, either for dural hemostasis to repair defects in the diaphragm a sellae or as a marker to be followed on plain skull radiographs.
Eight patients had had prior operations (four transsphenoidal and seven transfrontal) and were seen with evidence of residual or recur-rent tumor (3 weeks to 31 years later). Reexploration 0-39 days postoperatively was necessary in three other patients because of iatrogenic cerebrospinal fluid leaks.
IMMEDIATE P.O. PERIOD 0-21 Days
55 Scans (47 Patients)
REMOTE P.O. PERIOD 39 Days -56 Months
15% Axial Only
178 Scans (108 Patients)
Fig. 2.-Decisions to use contrast material and choices of scan planes were made so as to optimally image early and later postoperative (P.O.) changes (see Discussion).
95 Functioning Tumors 25 Nonfunctioning r -__________________________________ ~MACROADENOMAS
57 microadenomas 36 MACRO ADENOMAS
Fig. 3.-Clinical outcome of 95 functioning tumors and 25 nonfunctioning tumors.
Pathologic
In each case, the pituitary adenoma or the postoperative sellar contents were microsectioned and stained with hematoxylin and eosin, Gomori reticulin, and periodic acid-Schiff. Serial microsections were stained immunocytochemically by the peroxidase-antipero xi-dase method, as described by Sternberger et al. [11]. Antisera to growth hormone, prolactin, adrenocorticotropic horrnone (ACTH), follicle-stimulating hormone, luteinizing hormone, and thyroid-stimu-lating hormone were applied (Immulok, Carpenteria, CAl. Pituitary glands that were normal at autopsy served as positive controls; substitution of specific primary antiserum with normal rabbit serum served as negative controls.
Because a nonfunctioning macroadenorna rnay falsely elevate the serum prolactin level by corn pressing the pituitary stalk (pseudopro-lactinoma) [12], immunostaining was performed on the surgical spec-imens in all cases with elevated prolactin levels. Eight pseudoprolac-tinomas were identified, including six that presented as Forbes-Albright syndrome (amenorrhea-galactorrhea). Preoperative blood prolactin levels in these patients were as high as 85.5 ngjml (normal,
AJNR:6, Sept/Oct 1985 CT OF RESECTED PITUITARY ADENOMAS 725
Maximum prolactin level (ng/mil
Postop 400 350 300 250 200 150 100 50 550
119 Cures 1
440
510
~
[
~9~:"":..~
__
\11
11
1
t.
1.'
..
Normal (L..:...:.-.:...:..c'----"..:...!...:.-Ll:..;!'-'l'--_ _ _ _ _ _ _ _A
Maximum
B
prolactin level (ng/ml) Preop1
Postop Growth hormone, (ng/ml) Postop 1400 1200 1000 800 600 250 200 150 100 50Normal [
c
2 4 6 8 10 12 14 16 18 2 4 6 8 10 12 14 16 18
1 2 3 4 5 6 7 1 2 3 4 56789101112131915161718
373
- - -- -- - - -- - -- -
-1
•
I 2 3 4 II 12 1 2 3 4 5 MACRO micro MACRO
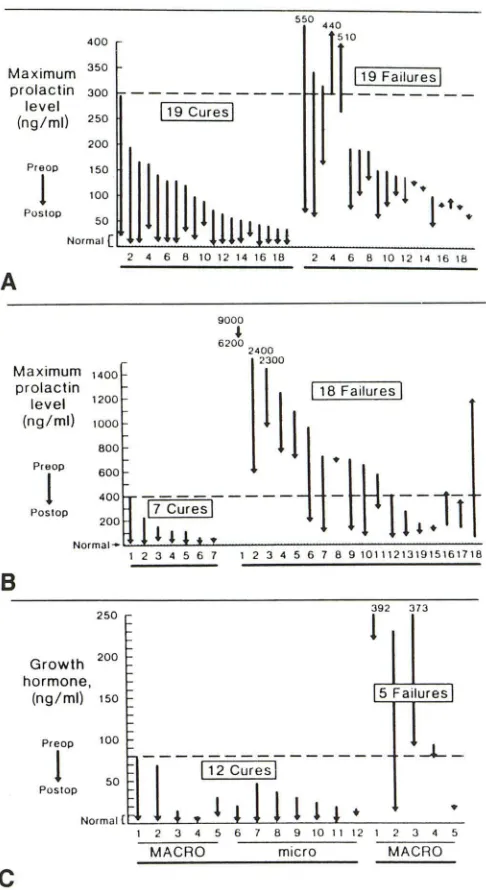
Fig. 4. -Maximal recorded preoperative and postoperative basal prolactin levels for 38 patients with prolactin microadenoma (A) and for 25 with prolactin macroadenoma (8). C, Maximal recorded preoperative and postoperative growth hormone levels for 17 acromegalic patients. Even highest postoperative hormone levels of most patients classified as cures decreased to within normal range. Provocative tests were used to classify borderline cases. Preoperative levels above a given threshold for each tumor type (broken lines) reliably predicted failure. Apparent increases in postoperative prolactin levels in cases 16-18 in 8 were from preoperative bromocriptine therapy, which was discon-tinued postoperatively.
and not by hormonal criteria-which is true for all non functioning tumors.
Radiologic
In our present series, the two most commonly used techniques for scanning the sella after surgery were axial scans without contrast enhancement during the immediate postoperative period and biplanar (axial and coronal) scans with contrast enhancement in the remote
A
B
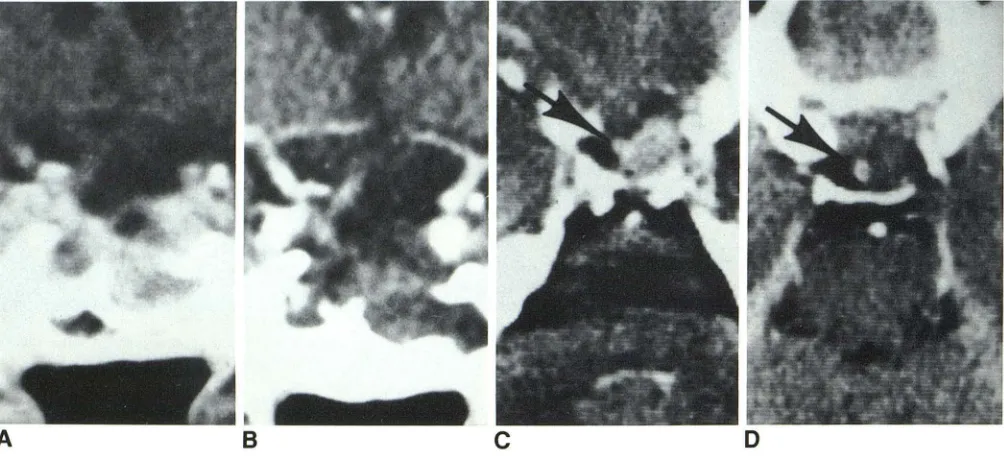
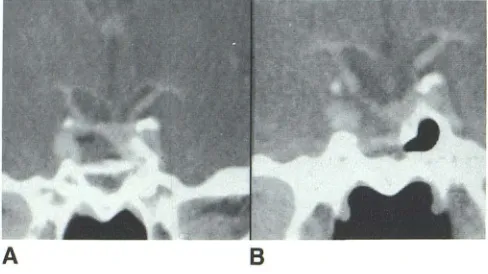
Fig. 5.-At surgery, only fibrous tissue was found in this sella, which had been packed transsphenoidally with autograft muscle 5'/2 months before (A). Enhancement seen here may reflect late stage of inflammatory reaction. 8, 14 months after second surgery, homograft muscle plug also enhanced but was more contracted than autograft plug at 5'12 months. Bony stent is well seen.
postoperative period (fig. 2). Most sellae were scanned with 3-mm slices at 3-mm intervals, although 1.5-mm slices with 1.5-mm intervals in the axial plane were used for reconstruction when direct coronal views could not be obtained.
A total of 369 CT scans were reviewed retrospectively: 136 preoperative and 233 postoperative. Intrasellar contents were eva l-uated for the presence of normal pituitary gland or for alterations from normal. The location, size, and pattern of any density or en-hancement change, as well as the presumed cause (such as air, blood, hemostatic agents, bone, cartilage, muscle, fat, or tumor), were recorded. Suprasellar and parasellar structures, including the pituitary stalk, carotid siphon, cavernous sinus, suprasellar cisterns, optic chiasm, and the sphenoid sinus, were similarly evaluated, and the findings (including displacement and size) were recorded. The CT findings were separated into those seen during initial hospitalization and those seen later on follow-up scans. Of these scans, 55 (47 patients) were obtained in the immediate postoperative period «21 days), while 178 (108 patients) were obtained in the remote po stop-erative period (39 days to 56 months after surgery).
Results
Clinical
Of the 95 patients with functioning adenoma, 48 (51 %) were "cured" by surgery alone, whereas 45 (47%) had hor-monal evidence of residual tumor. Of the 25 patients with nonfunctioning tumors (necessarily evaluated by CT criteria only), eight (32%) were cured by surgery and 10 (40%) had incomplete resection. The clinical status of seven patients with nonfunctioning and two with functioning tumors was indeterminate, pending follow-up CT or hormonal testing (fig. 3).
[image:3.612.51.294.81.526.2] [image:3.612.308.558.87.231.2]726
KAPLAN ET AL. AJNR:6, Sept/Oct 1985A
B
A
B
Fig. 7.- A, 7 days. B-O, 18 months. Bony stent (arrows) on coronal (A) and
axial (C) views. O. Adjacent pocket of air at top of stent (arrow) persisted on late follow-up scans. B, Fat density in left parasellar region (arrow) was similar
untreated either because the residual tumor remained indolent or because of the patient's age.
The maximal preoperative prolactin and growth hormone levels of 63 patients with prolactinomas and 17 with acro-megaly were compared. Even without provocative testing,
postoperative hormonal levels separated patients with cures from those with residual functioning tumors fairly well (fig. 4).
Similar methods were used to identify success in patients with Cushing disease.
c
c
Fig. 6.-Bony stent was almost al-ways seen (arrow) on early postoperative scans (day 4). Muscle plug, blood, and residual tumor often overlapped (B and C) and could not be distinguished without serial scans.
D
to orbital fat and was seen in one other non functioning tumor, in addition to this resected gonadotrophic adenoma (cf. fig. 13B). Similar low-density areas have been noted by others in paraseliar regions in Cushing disease [13].
Surgical
The surgeon's impression of residual or grossly invasive tumor was generally accurate, in that 10 patients with func-tioning tumors said to be invasive at surgery and five with
functioning tumors said to be incompletely resected had elevated hormonal levels postoperatively. However, 14 of 48 patients with tumors considered to be "completely" removed
AJNR:6, Sept/Oct 1985 CT OF RESECTED PITUITARY ADENOMAS 727
Fig. 8.-Sequential early postoperative scans demonstrate decreasing at-tenuation of blood and reabsorption of air. Residual tumor is demonstrated on
B
Fig. 9.-After successful removal of ACTH microadenoma, low density
(arrow) seen in sella at 2 weeks (A) but not at 15 months (8) may represent either Gelfoam (which contains air) or free air introduced at surgery. Sphenoid fluid level or debris, seen at 2 weeks, was a common finding in early postop-erative period, and its subsequent disappearance was also typical.
Pathologic
A homograft muscle plug removed from a patient with a
cerebrospinal fluid leak at 39 days histologically demonstrated
early signs of an inflammatory reaction and fibrosis. Dense
fibrous tissue with nonspecific chronic inflammation was
found in the reoperated sellae of two other patients with
diffuse intrasellar enhancement on preoperative CT. One
pa-tient had undergone transsphenoidal surgery elsewhere 5112
months before, and the sella was packed with autograft
muscle (fig. 5), and the second patient had undergone
trans-frontal craniotomy and radiotherapy 16 months before.
Radiologic
The CT appearance of the sella after operation depended
on the size of the tumor, amount of tissue resected, surgical
follow-up scans at 3'12 months. Contrast medium would have added little in immediate postoperative period to identify residual tumor.
technique, materials inserted into the operative site, interval
since surgery, and postoperative therapy.
Early Postoperative Period (0-21 Oays) (47 Patients)
Because most early scans were obtained without contrast
medium, enhancing structures, such as the pituitary gland,
pituitary stalk, residual tumor, carotid siphons, and cavernous
sinus, could not be evaluated. In addition, meaningful
conclu-sions regarding the optic chiasm and suprasellar cisterns were
often impossible because of disturbance from surgical
manip-ulation.
Alterations of intrasellar attenuation were increased by the
bony stent; increased or isodense by blood, tumor, or muscle;
and decreased by air, fat, or Gelfoam.
The septal bone stent was almost always evident on the
axial scan as a linear or curvilinear calcific density (figs. 6 and
7). Hemorrhage occupied the tumor bed in 23 of 40 cases of
macroadenoma but in only one of seven cases of
microade-noma. In cases with serial studies, blood exhibited decreasing
attenuation, regressing toward isodensity, even in this short
(21 day) time span (fig. 8). The appearance of muscle plug,
blood, and residual tumor ranged from hyperdense to iso
-dense, and frequently these three entities could not be distin
-guished with a single examination (fig. 6).
Air was present in the tumor bed or subarachnoid space in
22 of 40 cases of macroadenoma but was not encountered
in any of the seven cases of microadenoma. In almost all
cases, detectable intrasellar air was reabsorbed within 21
days. In one case, postoperative deterioration of the muscle
plug and seal was accompanied by a sudden increase of
intracranial air and massive cerebrospinal rhinorrhea. Unlike
intrasellar fat, air and Gelfoam were usually reabsorbed and
not seen on later scans (fig. 9), with one exception (fig. 7).
All patients had alterations in the sphenoid sinus, with
changes ranging from complete opacification to moderate
membrane thickening. In one-fifth of the patients, fluid, debris,
728 KAPLAN ET AL. AJNR:6. Sept/Oct 1985
A
B
Fig. 10. -ACTH macroadenoma at 9 (A) and 18 (B) months (6 and 15 months postirradiation. respectively). Typical decrease in contrast enhancement of residual tumor usually occurs 6-12 months after irradiation. Nonfunctioning
A
B
Fig. 11. -8ecause of normal prolactin levels after removal of prolactin microadenoma. we concluded that postoperative enhancement seen here at 17 months (A) was due to inflammation. B. Follow-up scan 10 months later. Decrease in enhancement is uncharacteristic of untreated tumor.
Contrast enhancement was used in 11 of the 47 cases and
enabled the detection of enlargement of the pituitary stalk (to a diameter equal to or larger than the basilar artery at the level of the dorsum sellae) in four cases (two with preoperative
enlargement) and stalk displacement in one case (also present preoperatively). Contrast medium was of no particular help in
evaluating the other structures.
Remote Postoperative Period (39 Days-56 Months) (108
Patients)
Findings (in order of prevalence) on the late follow-up CT
scans of the 95 patients with functioning tumors included
c
o
adenoma at 6 (C) and 13 (0) months (3 and 10 months postirradiation. respectively). Persistent enlargement and displacement of stalk (arrows). de-spite decreased enhancement and size of residual tumor after irradiation.
TABLE 1: Postoperative CT Changes in 12 Acromegalic Patients "Cured" by Surgery
No. of Patients
Finding Finding Present on Finding Improved on Preoperative CT Postoperative CT
Cutis gyrata . . . . . . . . 4 3
Eye muscle enlargement . 7 3
Pituitary stalk enlargement 7 6
Note.-Follow-up was 5 days to 42 months (mean. 16.7 months). No improvement in
these features was seen in any of five other patients with residual tumor.
normal-appearing pituitary gland in 60, empty or partially empty sella in 47, displaced stalk in 28, enhancing intrasellar tissue other than normal gland in 26, enlarged stalk in 10, acromegalic soft-tissue changes in seven, and inferior migra-tion of the optic chiasm in four.
Of the 60 patients with no enhancing tissue other than normal-appearing pituitary gland, 20 (33%) had residual tumor by hormonal criteria.
About half of all patients (including 47 of the 95 with
functioning tumors) had an empty or partly empty sella post-operatively. The secondary empty sella developed after
re-section of the functioning macroadenoma in 18 patients and after removal of a microadenoma in 29. Of the 47 patients, 22 (eight with empty and 14 with partially empty sellae) had hormonal evidence of residual tumor, even though most of them lacked evidence of tumoral enhancement.
Tumor enhancement, when seen, varied in character and
could be described in different cases as diffuse, mottled,
peripheral, focal, or nodular [14] (fig. 10). Such enhancement
was absent in 17 (81 %) of 21 cases of microadenoma and in
[image:6.612.59.561.82.311.2] [image:6.612.55.299.377.536.2]AJNR:6. Sept/Oct 1985 CT OF RESECTED PITUITARY ADENOMAS 729
Fig. 12.-Acromegalic soft-tissue changes such as cutis gyrata (arrows)
and enlargement of eye muscles and
pi-tuitary stalk were observed to disappear postoperatively in cured patients (see
ta-ble 1).
A
B
o
E
evidence of residual tumor. Surgical clips, which would have
obscured any enhancement, were present in two of the latter
three cases. Similar enhancement was seen about the floor
of the sella near the homograft muscle plug in five (11 %) of
46 patients in whom functioning tumors had been surgically
"cured" and in the previously mentioned patient with an
autograft muscle plug. Unlike neoplastic enhancement, this
inflammatory change decreased in subsequent scans (fig. 11).
Displacement of the stalk from its usual midline position,
seen preoperatively in 38 patients, persisted in 27 and
dis-appeared in 11. Twenty of the 27 patients had residual tumor,
as did one other in whom displacement evolved. By contrast,
10 of the 11 patients in whom stalk displacement disappeared
c
Fig. 13.-Bony stent acted as nidus for regions of ectopic calcification. A
-C. One patient at 4 (8) and 29 (e) months. D and E. Another patient at 4 days (D) and 29 months (E). Presence of stent (D. arrow) or any obvious associated calcifications should not be confused with tumoral calcification. Fat density in posterior parasellar region (E. arrow) is similar to that in fig. 7B.
were cured (four had microadenoma and six had
macroad-enoma).
Enlargement of the stalk, seen preoperatively in 12 patients,
persisted in four and disappeared in eight. All four with persistent enlargement and four others in whom enlargement
evolved had residual tumor. Again, contrast-enhanced studies
revealed that all eight patients in whom the enlargement
disappeared were cured (six had microadenoma and two had
macroadenoma).
Of 37 patients with functioning macroadenoma, 14 had
extension into the parasellar regions on preoperative CT
examination, and none of the 14 was cured surgically. Of 11
ex-730 KAPLAN ET AL. AJNR:6, Sept/Oct 1985
A
B
Fig. 14.-Stent disappeared in one patient with residual tumor. A, 5 days.
B, 13 months.
tension preoperatively, seven were not cured and four had indeterminate outcomes pending follow-up CT. If the experi-ence with functioning macroadenomas is applicable to these nonfunctioning adenomas, we would expect these four pa-tients to have residual tumor.
Preoperative or postoperative nonsurgical therapy-radia-tion, bromocriptine, or a combination of the two-in addition
to reducing the levels of prolactin and growth hormone [15], frequently caused a decrease in tumor enhancement and
size, which was typically visible on CT 6-12 months after
commencement of treatment (fig. 10). In general, the effects
on enhancement were seen only with radiation or the combi-nation-type therapies. All methods usually led to shrinkage of tumor bulk most strikingly demonstrated in prolactin
microad-enomas, which were radiologically detectable in only 33% of
patients treated with bromocripine preoperatively, compared
with 75% of the patients without such treatment.
In acromegalic patients who were cured, soft-tissue
changes, such as cutis gyrata and eye muscle or stalk en-largement, were observed to disappear postoperatively (table
1) (fig. 12). Other less frequent alterations seen in all tumor
types included inferior migration of the optic chiasm assoc
i-ated with the postoperative empty sella and alterations in and
about the bony stent. In one patient with residual tumor, the
stent disappeared, whereas in four others, the stent appeared to act as the nidus for deposits of ectopiC calCification, from
which it was separated by a lucent zone in two patients (figs. 13 and 14).
Finally, surgical clips, present in 19 sellae, rendered CT
indeterminate in most cases, even despite hormonal evidence of residual tumor in five.
Discussion
As a result of the selection criteria applied in this study, the
observed cure rates were lower than those reported by Laws
and coworkers [1, 6, 8-10, 16] for their overall surgical experience. Patients whose hormone levels returned promptly
to normal after removal of a proved functioning tumor gener-ally had persisting normalization of pituitary function. This was not necessarily true for patients with
pseudoprolacti-TABLE 2: CT Indicators of Success or Failure of Surgical Treatment in 95 Cases of Functioning Pituitary Tumors
No. of No. of Patients ·Cured"
Finding Patients with with Residual (Success) or
Finding Tumor (Failure) (%)
Success (n
=
48):Pituitary stalk enlargement
resolved 8 8 (100)
Pituitary stalk displacement
resolved 11 10 (91)
No intrasellar abnormal
enhancement. 60 40 (66)
Empty or partly empty sella 47 22 (47)
Failure (n
=
45):Pituitary stalk enlargement
persisted or evolved . 8 8 (100)
Pituitary stalk displacement
persisted or evolved . 28 20 (71)
Parasellar extension on
preop-erative CT. 14 14 (100)
Intrasellar abnormal
enhance-ment (inflammatory in 19%) 26 21 (81)
Note. -This table summarizes the prevalence of vanous findings seen on preoperative and postoperative CT arranged in order of their relative value in predicting curative resection and residual tumor, as independently assessed by hormonal criteria. These trends were seen in both microadenoma and macroadenoma. Clinical status of Ncure" is unknown in two cases pending follow-up hormonal and CT studies.
noma, whose decreased levels of prolactin may simply reflect an elimination of the mass effect. Residual functioning tumor was diagnosed by elevated blood hormone levels, even when tumor could not be resolved by CT. Furthermore, when
preoperative levels of prolactin exceeded 400 ngjml or growth
hormone levels exceeded 90 ngjml, surgery was uniformly unsuccessful at completely ablating the tumor (fig. 4).
To understand the postoperative CT changes within the sella, one must appreCiate that certain foreign materials were
implanted at surgery. Since in our patients the foreign material
most often was homograft muscle, we initially assumed that CT enhancement observed in 11 % of hormonally cured pa
-tients represented an inflammatory reaction due to tissue mismatch. We have, in fact, histologically documented such
a response in the presence not only of homograft muscle but also of autograft (nonforeign) muscle (fig. 5). Therefore, we
have concluded that CT enhancement in the absence of
residual tumor is due in part to an inflammatory response to these tissues. Of the 26 cases with postoperative intrasellar
enhancement, five (19%) were presumably due to inflam
-mation and 21 (81 %) to tumor. The fact that most muscle plugs were not observed to enhance may merely reflect a variability in the time course and severity of the inflammatory reaction, in addition to the possible effect of tissue mismatch.
The time course of various postoperative intrasellar
changes has implications for optimizing the conduct of CT
examinations. In the early postoperative period, intrasellar
attenuation may be increased by blood, tumor, or muscle plug. Hemorrhage is of the most immediate clinical concern
and cannot be distinguished from residual tumor on contrast
-enhanced scans, so we have generally elected to use non
-contrast CT. Intrasellar and subarachnoid air was normally
[image:8.612.58.302.87.224.2] [image:8.612.318.560.105.303.2]AJNR:6, Sept/Oct 1985 CT OF RESECTED PITUITARY ADENOMAS 731
weeks after operation. Persistent or increasing amounts of
air on serial scans beyond this time imply the presence of a
fistulous communication and should be cause for concern.
Serial CT scans are valuable during the remote
postoper-ative period to distinguish the usual progressive atrophy and
fibrosis of a muscle plug-leading to a partly and then
com-pletely empty sella-from the persistence of tumor mass. If
contrast medium is added, serial CT may also identify
inflam-matory enhancement that, unlike the enhancement of
un-treated residual tumor, decreases in size and intensity with
time (fig. 11).
While untreated residual tumors may show increasing size
and enhancement, the use of irradiation or bromocriptine
postoperatively usually reversed these effects, with
enhance-ment and size decreasing after irradiation or combination
therapy and size alone affected by bromocriptine [17]. These
effects were obtained 6-12 months after irradiation and
con-siderably earlier after bromocriptine therapy. The substantial
decrease in the CT detection rate of prolactin microadenomas
before operation in patients treated with bromocriptine
sug-gests that CT localization of microadenomas should be
car-ried out routinely before bromocriptine therapy. The
de-creased enhancement after irradiation may be due in part to
attenuation of the inflammatory response.
Enlargement or displacement of the pituitary stalk was
correlated with the presence of functioning microadenoma
and macroadenoma in cases of acromegaly, Cushing disease,
and, to a lesser extent, prolactinoma. The enlargement of the
pituitary stalk to a diameter equal to or greater than the
basilar artery at the level of the dorsum sellae, if seen on
preoperative CT, was 100% predictive of cure if the
enlarge-ment returned to normal on a remote follow-up scan and was
100% predictive of failure if the enlargement persisted or
evolved. These findings did not apply to the immediate
post-operative period (table 2).
Resolution of stalk displacement that was seen
preopera-tively was the second most reliable predictor of cure, but
displacement that persisted or evolved postoperatively was
less reliable than parasellar extension on preoperative CT or
abnormal intrasellar enhancement in predicting the presence
of residual tumor. The CT findings that were most predictive
of curative surgical resection and failure are summarized in
table 2. These observations should also be applicable to the
evaluation of nonfunctioning tumors.
In addition to having enlargement of the pituitary stalk,
acromegalic patients exhibited enlargement of other soft
tis-sues: scalp (cutis gyrata) and extraocular muscles. When a
surgical cure was attained, these alterations regressed on
postoperative scans (fig. 12) (table 1).
In general, our surgical colleagues were correct in predicting
persistent tumor if they observed gross tumor invasiveness.
They also greatly assisted the radiologist by eschewing the
use of intrasellar surgical clips (unless absolutely necessary).
These metallic clips create CT artifacts, the most common
cause of diagnostic difficulty. Of the patients with
microade-noma, surgical cures were attained in 100% (seven of seven)
of acromegalic patients, 77% (10 of 13) of patients with
Cushing disease, and 50% (19 of 38) of patients with
prolactinoma. These variations may reflect differences in
de-tectability at surgery, bromocriptine pretreatment, or
multifo-cality and diffuseness of some tumors.
Of 36 successfully resected microadenomas, 16 were seen
on preoperative CT as positive-enhancing areas and eight as
low-density areas, but 12 were not seen definitely. These
areas correlated with tumor locations noted in the operative
reports, and the abnormalities were absent on postoperative
scans. The absence of abnormal enhancement
postopera-tively was not a reliable criterion of cure, however, in that
81 % of residual functioning microadenomas lacked evidence
of abnormal enhancement in the postoperative period. If the
tumor extended into the parasellar region on preoperative
CT, it was virtually always refractory to cure.
Tumor calcification was rarely seen, and although the bony
stent varied in appearance with time, its true nature is obvious
and should not be misidentified as a neoplastic deposit.
REFERENCES
1. Laws ER Jr. Transsphenoidal microsurgery in the management
of acromegaly. In: Smith JL, ed. Smith's neuro-ophthalmology focus. New York: Masson, 1980:289-293
2. Waller RM III, Hoffman JC Jr, Tindall GT. CT of the sellar and parasellar region following transsphenoidal surgery. Presented
at the annual meeting of the Radiological Society of North
America, Chicago, November 1983
3. Robert F. Electron microscopy of human pituitary tumors. In:
Tindall GT, Collins WF, eds. Clinical management of pituitary disorders. New York: Raven, 1979:113-131
4. Abboud CF, Laws ER Jr. Clinical endocrinological approach to hypothalamic-pituitary disease. J Neurosurg 1979;51: 271-291
5. Fode NC, Laws ER Jr, Abboud CF, Randall RV, Kempers RD.
Prolactin secreting pituitary adenoma: a review and study of their
implications for fertility in women. J Neurosurg Nurs 1980;
12:210-213
6. Laws ER Jr, Ebersold MJ, Piepgras DG, Randall RV, Salassa
RM. The results of transsphenoidal surgery in specific clinical
entities. In: Laws ER Jr, Randall RV, Kern EB, Abboud CF, eds.
Management of pituitary adenomas and related lesions with emphasis on transsphenoidal microsurgery. New York: Appleton-Century-Crofts, 1982: 277 -305
7. Chang CH. Management of pituitary tumors (course 818). In:
Marks JE, Griem ML, eds. Syllabus: categorical course in therapy
of CNS tumors. Chicago: Radiological Society of North America, 1983
8. Laws ER Jr. Transsphenoidal tumor surgery for intra sellar pa-thology. Clin Neurosurg 1979;26:391-397
9. Laws ER Jr. Transsphenoidal approach to lesions in and about
the sella turcica. In: Schmidek HH, Sweet WH, eds. Operative
neurosurgical techniques: indications, methods, and results, vol.
1. New York: Grune & Stratton, 1982:327-341
10. Kern EB, Laws ER Jr. The rationale and technique of selective
transsphenoidal microsurgery for the removal of pituitary tumors.
In: Laws ER Jr, Randall RV, Kern EB, Abboud CF, eds. Mana ge-ment of pituitary adenomas and related lesions with emphasis on transsphenoidal microsurgery. New York: Appleton-Century
-Crofts, 1982:219-244
11. Sternberger LA, Hardy PH Jr, Cuculis JJ, Meyer HG. The unla
-beled antibody enzyme method of immunohistochemistry: prep
732
KAPLAN ET AL. AJNR:6, Sept/Oct 1985(horseradish peroxidase-antihorseradish peroxidase) and its use in identification of spirochetes. J Histochem Cytochem
1970;18:315-333
12. Randall RV, Scheithauer BW, Laws ER Jr, Abboud CF. Pseu-doprolactinomas. Trans Am Clin Climatol Assoc 1982,94: 114-121
13. Bachow TB, Hesselink JR, Aaron JO, Davis KR, Taveras JM.
Fat deposition in the cavernous sinus in Cushing's disease.
Radiology 1984;153: 135-136
14. Gardeur D, Naidich TP, Metzger J. CT analysis of intrasellar
pituitary adenomas with emphasis on patterns of contrast
en-hancement. Neuroradiology 1981 ;20: 241-247
15. Spark RF, Dickstein G. Bromocriptine and endocrine disorders.
Ann Intern Med 1979;90:949-956
16. Randall RV, Laws ER Jr, Abboud CF, Ebersold MJ, Kao PC,
Scheithauer BW. Transsphenoidal microsurgical treatment of prolactin-producing pituitary adenomas: results in 100 patients.
Mayo Clin Proc 1983;58: 1 08-121
17. McGregor AM, Scanlon MF, Hall K, Cook DB, Hall R. Reduction
in size of a pituitary tumor by bromocriptine therapy. N Engl J