R E V I E W
Open Access
Omega-3 fatty acids eicosapentaenoic acid
and docosahexaenoic acid and their
mechanisms of action on apolipoprotein
B-containing lipoproteins in humans: a
review
Jan Oscarsson
*and Eva Hurt-Camejo
Abstract
Background:Epidemiological and genetic studies suggest that elevated triglyceride (TG)-rich lipoprotein levels in the circulation increase the risk of cardiovascular disease. Prescription formulations of omega-3 fatty acids (OM3FAs), mainly eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), reduce plasma TG levels and are approved for the treatment of patients with severe hypertriglyceridemia. Many preclinical studies have investigated the TG-lowering mechanisms of action of OM3FAs, but less is known from clinical studies.
Methods:We conducted a review, using systematic methodology, of studies in humans assessing the mechanisms of action of EPA and DHA on apolipoprotein B-containing lipoproteins, including TG-rich lipoproteins and low-density lipoproteins (LDLs). A systematic search of PubMed retrieved 55 articles, of which 30 were used in the review; 35 additional arrticles were also included.
Results:In humans, dietary DHA is retroconverted to EPA, while production of DHA from EPA is not observed. Dietary DHA is preferentially esterified into TGs, while EPA is more evenly esterified into TGs, cholesterol esters and phospholipids. The preferential esterification of DHA into TGs likely explains the higher turnover of DHA than EPA in plasma. The main effects of both EPA and DHA are decreased fasting and postprandial serum TG levels, through reduction of hepatic very-low-density lipoprotein (VLDL)-TG production. The exact mechanism for reduced VLDL production is not clear but does not include retention of lipids in the liver; rather, increased hepatic fatty acid oxidation is likely. The postprandial reduction in TG levels is caused by increased lipoprotein lipase activity and reduced serum VLDL-TG concentrations, resulting in enhanced chylomicron clearance. Overall, no clear differences between the effects of EPA and DHA on TG levels, or on turnover of TG-rich lipoproteins, have been observed.
Effects on LDL are complex and may be influenced by genetics, such asAPOEgenotype.
Conclusions:EPA and DHA diminish fasting circulating TG levels via reduced production of VLDL. The mechanism of reduced VLDL production does not involve hepatic retention of lipids. Lowered postprandial TG levels are also explained by increased chylomicron clearance. Little is known about the specific cellular and biochemical mechanisms underlying the TG-lowering effects of EPA and DHA in humans.
Keywords:Eicosapentaenoic acid (EPA), Docosahexaenoic acid (DHA), Very-low-density lipoproteins, Low-density lipoproteins, Chylomicrons, Triglycerides, Lipoprotein lipase, Apolipoprotein B, Apolipoprotein E, Apolipoprotein CIII
* Correspondence:Jan.Oscarsson@astrazeneca.com
AstraZeneca Gothenburg, Pepparedsleden 1, SE-431 83 Mölndal, Sweden
Background
Triglycerides (TGs) are carried in the circulation as TG-rich lipoprotein particles, mainly in the very-low-density lipoprotein (VLDL) fraction in the fasted state and as VLDL and chylomicrons in the fed state. High plasma TG levels that meet the definition of mild-to-moderate hypertriglyc-eridemia (2–10 mmol/L [175–885 mg/dL]) strongly en-hance the risk of cardiovascular (CV) disease [1, 2]. Adjustment for high-density lipoprotein (HDL)- and non-HDL-cholesterol markedly reduces the association between plasma TGs and CV disease, indicating a role in the en-hanced CV disease risk for cholesterol carried in the atherogenic remnant lipoproteins associated with hypertri-glyceridemia. However, Mendelian randomization studies indicate a direct causal relationship between TG-rich lipo-proteins and coronary heart disease [1, 2]. Severe hypertri-glyceridemia, defined as TG levels greater than 10 mmol/L (885 mg/dL), is mainly associated with an increased risk of acute pancreatitis [2, 3]. Hypertriglyceridemia is a common disorder, with polygenic and lifestyle factors as its main eti-ology; monogenic etiology is much rarer. The prevalence of mild-to-moderate hypertriglyceridemia estimated from the Copenhagen General Population Study was 28%, while the prevalence of severe hypertriglyceridemia was 0.1% [2]. The prevalence of high TG levels (200–<500 mg/dL) was 16.2% and of very high TG levels (≥500 mg/dL) was 1.1% in the US adult population [4].
First-line treatment for patients with hypertriglyc-eridemia is management of diet (reduced dietary fat, simple carbohydrates and alcohol) and more exercise. Fibrates are recommended as first-line pharmacologic therapy in patients with severe hypertriglyceridemia, while statins are recommended as first-line treatment in patients with mild-to-moderate hypertriglyceridemia [1, 3]. Statins sometimes need to be combined with a fibrate, niacin or omega-3 fatty acids (OM3FAs) to man-age mild-to-moderate hypertriglyceridemia [1, 3]. How-ever, the US Food and Drug Administration recently withdrew previous approvals recommending the com-bination of statins with fibrates or niacin. The decision was prompted by the results of three large trials, which failed to show a reduction in CV events with these ther-apy combinations [5]. OM3FA treatment on top of sta-tins is well tolerated and effectively lowers levels of VLDL particles and TGs [6, 7]. Prescription-grade OM3FA formulations are now the remaining approved combination therapy with statins for further reduction of plasma TGs in patients with severe hypertriglyc-eridemia and increased CV risk; the combination of sta-tins with OM3FAs is therefore of great clinical importance. Doses of about 2–4 g of prescription-grade
OM3FAs, mainly containing eicosapentaenoic acid
(EPA) and docosahexaenoic acid (DHA), reduce plasma TG levels by about 30% and are indicated for prevention
of pancreatitis in patients with severe hypertriglyc-eridemia [1, 3]. There is a lack of evidence that OM3FA treatment reduces CV events in patients with hypertri-glyceridemia of any severity, as recently reviewed by Sis-covick and colleagues [8]. Two randomized outcome trials, REDUCE-IT (REDUuction of Cardiovascular Events with EPA - Intervention Trial) and STRENGTH (Outcomes Study to Assess STatin Residual Risk Reduc-tion with EpaNova in HiGh CV Risk PatienTs with Hypertriglyceridemia), are ongoing to assess residual risk reduction when adding OM3FA therapy to statins [9, 10]. Aside from effects on TG-rich lipoproteins, OM3FAs may reduce CV risk via other mechanisms such as effects on arrhythmias and inflammation, as reviewed by de Roos and colleagues [11]. However, re-duction in atherosclerosis in animal models or humans by administration of OM3FAs has not been convincingly demonstrated [8, 11].
Here, we review the mechanisms of action of the OM3FAs EPA and DHA on production and clearance of apolipoprotein (apo)B-containing lipoproteins, including TG-rich lipoproteins (VLDLs, chylomicrons) and low-density lipoproteins (LDLs). The emphasis is on results obtained in clinical studies. Many studies have demon-strated the TG-rich lipoprotein-lowering effects of OM3FAs, with mechanistic studies focussing on animal models. Less is known about the specific metabolism and effects of the two principal constituents of prescrip-tion OM3FA formulaprescrip-tions, EPA and DHA, and their mechanisms of action in humans. For further reading, a meta-analysis and systematic review was published on this topic by Wei and Jacobson [12]. Another recom-mended review is a comprehensive summary of kinetic studies on the effects of OM3FAs on apoB-containing li-poproteins, published by Harris and Bulchandani [13]. Finally, a review that also includes results from mechan-ism of action studies of OM3FAs on TG metabolmechan-ism in cultured cells and animal models was published by Da-vidson [14].
Search strategy
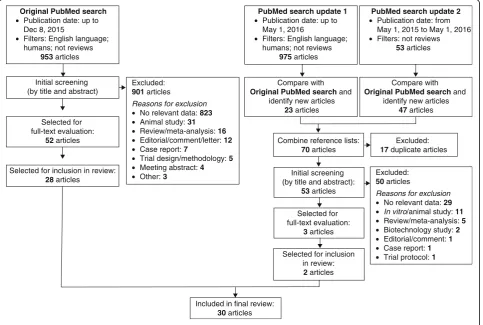
The systematic search process is summarized in Fig. 1. The original literature search was performed on Decem-ber 8, 2015 and identified a total of 953 articles for screening, of which 52 were selected for full-text evalu-ation; 28 of these were used in the review. The most common reasons for excluding articles from the
systematic search were either that they did not con-tain relevant data relating to the effects of DHA and EPA on lipoprotein metabolism, or that they did not report clinical studies. A further literature search process was performed on May 1, 2016 to identify ar-ticles published since the original search, using two approaches. First, a new search was performed using the same terms as the original search, applying a pub-lication cut-off date of May 1, 2016; this revealed 23 new articles. Secondly, another new search was per-formed using the original terms but with a publica-tion date range of May 1, 2015 to May 1, 2016 and without the filter for human studies; this was to en-sure the detection of any recently added articles that may have been missing the appropriate Medical Sub-ject Heading (MeSH) terms for human studies. Com-bining the articles identified using the two update searches and discarding duplicates revealed 53 new articles for screening. Three articles were selected for full-text evaluation, 2 of which were used in the re-view. Thus, from an overall total of 55 potentially relevant articles identified by the systematic search (52 from the original search and 3 from the update search), 30 were used for the review (Table 2).
Table 1Search terms for the systematic PubMed search
Search string category
Search terms used
(1) DHA/EPA ‘docosahexaenoic acid’OR‘docosahexaenoic’OR
‘eicosapentaenoic acid’OR‘eicosapentaenoic’OR
‘icosapentaenoic acid’
(2) Outcomes ‘triglyceride’OR‘triacylglycerol’OR‘triacylglycerols’
OR‘triacylglyceride’OR‘triacylglycerides’OR
‘lipoprotein’OR‘HDL’OR‘HDL-C’OR‘HDLC’OR‘LDL’
OR‘LDL-C’OR‘LDLC’OR‘VLDL’OR‘VLDL-C’OR
‘VLDLC’OR‘apolipoprotein’OR‘postprandial lipids’
OR‘post-prandial lipids’
(3) Mechanism of
action ‘
production’OR‘clearance’OR‘mode of action’OR
‘mechanism of action’OR‘controlled’OR
‘comparative’
Combined search (1)AND(2)AND(3)
DHAdocosahexaenoic acid,EPAeicosapentaenoic acid,HDLhigh-density
lipo-protein,HDLC/HDL-Chigh-density lipoprotein cholesterol,LDLlow-density
lipo-protein,LDLC/LDL-Clow-density lipoprotein cholesterol,VLDLvery low-density
lipoprotein,VLDLC/VLDL-Cvery low-density lipoprotein cholesterol
Included in final review: 30articles
Selected for full-text evaluation:
3articles
Excluded: 50articles
Reasons for exclusion • No relevant data:29 • In vitro/animal study:11 • Review/meta-analysis:5 • Biotechnology study:2 • Editorial/comment:1 • Case report:1 • Trial protocol:1 Selected for inclusion
in review: 2articles
• Publication date: up to Dec 8, 2015
• Filters: English language; humans; not reviews
953articles
Initial screening (by title and abstract)
Selected for full-text evaluation:
52articles
Excluded: 901articles
Reasons for exclusion • No relevant data:823 • Animal study:31 • Review/meta-analysis:16 • Editorial/comment/letter:12 • Case report:7
• Trial design/methodology:5 • Meeting abstract:4 • Other:3
Selected for inclusion in review:
28articles (by title and abstract):Initial screening 53articles Combine reference lists:
70articles
Excluded: 17duplicate articles
• Publication date: up to May 1, 2016
• Filters: English language; humans; not reviews
975articles
Compare with
Original PubMed searchand
identify new articles 23articles
• Publication date: from May 1, 2015 to May 1, 2016
• Filters: not reviews 53articles
Compare with
Original PubMed searchand
identify new articles 47articles
Original PubMed search PubMed search update 1 PubMed search update 2
Table 2 Characteristics of included studies identified by the systematic Pub Med search (Continued) Double-blind, placebo-controlled Hyperlipidemic men and women, n= 42 Control, 0.9 g EPA + 0.8 g DHA No effect on non-heparin or post-heparin plasma LPL activity Nozaki et al. [ 57 ] Open, uncontrolled Hyperlipidemic men and women, n =1 4 2.4 g EPA N/A 6 months Total cholesterol, TG, LDL-C plasma levels significantly reduced; LDL particle size unchanged; CETP activity significantly reduced Olano-Martin et al. [ 60 ]
Double-blind, cross-over, placebo-controlled
Table
2
Characteristics
of
included
studies
identified
by
the
systematic
Pub
Med
search
(Continued)
Control,
fish
diet
(0.38
g
EPA
+
0.67
g
DHA
five
times
weekly),
1.68
g
DHA,
fish
oil
(1.33
g
EP
A
+
0.
95
g
DHA)
DHA
was
incorporated
into
PLs
and
TGs,
while
EPA
was
incorporated
into
PLs
and
CEs;
DHA
retroconverted
to
EPA
Wong
et
al.
[
40
]
Single-blind,
controlled
Obese
men
and
women,
n=
27
Hypocaloric
diet
alone
or
in
combination
with
1.8
g
EPA
+
1.56
g
DHA
Hypocaloric
diet
12
weeks
Compared
with
weight
loss
alone,
EPA
+
DHA
reduced
postprandial
TGs
and
apoB48
Woodman
et
al.
[
19
]
Double-blind, placebo-controlled
Patients
with
type
2
diabetes
mellitus,
n=
59
Control,
3.8
g
EPA,
3.7
g
DHA
Olive
oil
6
weeks
Similar
effects
of
DHA
and
EPA
on
serum
lipids,
DHA
retroconverted
to
EPA
Woodman
et
al.
[
54
]
Double-blind, placebo-controlled
Patients
with
type
2
diabetes
mellitus,
n=
59
Control,
3.8
g
EPA,
3.7
g
DHA
Olive
oil
6
weeks
DHA
increased
LDL
size
to
a
greater
extent
than
EPA
aEPA
and
DHA
doses
may
be
proportions
of
a
larger
overall
dose
of
oil/OM3FAs
ALA
alpha-linolenic
acid,
Apo
apolipoprotein,
CE
cholesterol
ester,
CAD
coronary
artery
disease,
DHA
docosahexaenoic
acid,
EPA
eicosapentaenoic
acid,
FFA
free
fatty
acid,
LDL
low
density
lipoprotein,
LDL-C
low-density
lipoprotein
cholesterol,
LPL
lipoprotein
lipase,
N/A
not
applicable,
OM3FA
omega-3
fatty
acid,
PL
phospholipid,
PPAR
peroxisome
proliferator-ac
tivated
receptor,
VLDL
very-low-density
lipoprotein,
VLDL-apo
very-low-density
lipoprotein
apolipoprotein,
VLDL-C
very-low-densi
ty
lipoprotein
cholesterol,
VLDL-TG
very-low-densi
ty
lipoprotein
triglyceride,
TG
An additional 35 articles not identified in the system-atic search were included in the review (including the introduction); these were identified during development of the manuscript (citations in papers identified during the screening process, for example). These additional ar-ticles were included in the interests of providing context and completeness, and comprise 8 review articles about OM3FAs, 15 original articles about OM3FAs and lipo-proteins, and 12 articles about the importance of differ-ent lipoproteins in CV disease or mechanisms of action of lipoproteins of general importance for interpreting the OM3FA studies.
Results
Differences in the metabolism of DHA and EPA
After supplementation with fish oil (which contains DHA and EPA esterified to TGs and at lower concentra-tions than prescription-grade OM3FAs), both phospho-lipids and TGs in VLDL are enriched in EPA, while TGs, but not phospholipids, in VLDL are enriched in DHA [15]. This observation was corroborated in another study investigating enrichment of DHA and EPA in all lipoproteins. DHA was found mainly in TGs, while EPA, but not DHA, was found in cholesterol esters [16]. The preferential incorporation of DHA into TGs could help to explain why total DHA levels in plasma do not in-crease to the same extent as EPA levels following fish oil supplementation, because turnover of serum TGs is greater than turnover of phospholipids and cholesterol esters. Moreover, combined treatment with EPA and DHA showed that DHA is more available for beta-oxidation than EPA [17], possibly owing to the enrich-ment of TGs with DHA.
The metabolism of DHA and EPA has been described in clinical studies, with DHA being retro-converted to EPA and EPA being elongated mainly to docosapentae-noic acid (DPA) [18–22]. However, production of DHA from EPA does not seem to occur. Therefore, treatment with purified DHA results in an increase in both DHA and EPA, while treatment with purified EPA does not generally change DHA levels. The increase in EPA levels following DHA intervention can sometimes exceed the increase in DHA plasma levels [18].
Differential effects of DHA and EPA on TG-rich lipoproteins
In general, the TG-lowering effects of DHA and EPA are similar in both normotriglyceridemic [18, 23] and hyper-triglyceridemic patients [19, 22, 24]. In some studies, TG lowering tended to be more effective with DHA than with EPA supplementation in hypertriglyceridemic [18, 25] and normolipidemic individuals [18, 23, 26], while in one study EPA was more effective than DHA in normolipidemic in-dividuals [20]. In normolipidemic inin-dividuals, both DHA
and EPA decrease postprandial TG levels and it is not possible to tell from these studies whether one of the fatty acids has a superior efficacy [21, 27]. In summary, there is no clear difference between DHA and EPA with respect to reduction in fasting or postprandial TG levels.
VLDL production and clearance
A meta-analysis of human kinetic studies showed a consist-ent reduction in VLDL production rate following supple-mentation with OM3FAs, while effects on VLDL clearance were less consistent [13]. In a study investigating the effect of 3 weeks of fish oil versus safflower oil supplementation, VLDL-apoB and TG kinetics in normolipidemic and hyper-triglyceridemic individuals were determined [28]. VLDL-apoB production rate decreased in all individuals, while fractional clearance rate increased in normal individuals but not in hypertriglyceridemic individuals. Moreover, the results indicated that the reduced VLDL production rate was not caused by diminished flux of fatty acids, pointing towards a hepatic effect of OM3FAs on lipid handling. LDL-cholesterol (LDL-C) levels tended to increase and in some individuals an increased influx of LDL was observed, indicating increased hepatic production of LDL particles [28]. In a study comparing 4 weeks of daily supplementa-tion with either 15 g fish oil or 15 g of a blend of corn and olive oil, the clearance rate for VLDL-TGs was not influ-enced by the treatment [15]. It was therefore concluded that the reduction in plasma TGs was most likely caused by diminished VLDL production, in line with the study of Nestel et al. [28]. In more recent VLDL kinetic studies, lower doses of purified OM3FAs have been investigated. Chan et al. conducted a study comparing 4 g daily of OM3FAs and corn oil in 24 dyslipidemic men [29]. Treat-ment with OM3FAs decreased hepatic production of VLDL-apoB by 29% more than corn oil. This effect was ac-companied by a 35% decrease in hepatic TG synthesis. Moreover, conversion of VLDL-apoB to intermediate-density lipoprotein (IDL)-apoB, and IDL-apoB to LDL-apoB, increased significantly. The explanation for the en-hanced conversion of VLDL to IDL and LDL is likely to be a lower number of VLDL particles per lipoprotein lipase (LPL) enzyme, which leads to a greater proportion of parti-cles being converted into LDL [29].
TG and VLDL (including VLDL1) production decreased, and conversion of VLDL to IDL, and IDL to LDL, in-creased. The fractional clearance rate of VLDL, IDL or LDL did not change [30]. This study shows that OM3FA supplementation partly corrects for the underlying dis-order responsible for the atherogenic dyslipidemia in pa-tients with type 2 diabetes by reducing hepatic production of VLDL1.
Possible mechanisms explaining reduced VLDL production Atherogenic dyslipidemia is associated with insulin re-sistance. While OM3FA treatment could result in a small improvement in hepatic insulin sensitivity [31], other effects of OM3FAs must be of importance to the decrease in VLDL production resulting from OM3FA treatment. Insulin resistance is associated with increased hepatic fat content. In turn, liver fat content is positively associated with VLDL production [32]. Therefore, re-duced liver fat content should lead to rere-duced hepatic VLDL production. A meta-analysis of human interven-tion studies showed that OM3FAs decrease liver fat con-tent [33], which could help to explain the reduced VLDL production. Studies of OM3FA treatment of patients with non-alcoholic fatty liver disease have shown that re-duction in liver fat content was associated with a change in DHA levels, while fasting plasma TG levels were asso-ciated with EPA enrichment [34]. These results indicate that the relationship between liver fat reduction and plasma TG levels is not similar for DHA and EPA. The exact mechanisms taking place in human liver cells that explain reduced liver fat and reduced VLDL production are still speculative. Clinical studies have shown that OM3FA treatment increases fatty acid oxidation, as de-termined by indirect calorimetry [35, 36]. It is therefore possible that OM3FA treatment reduces VLDL produc-tion via reduced substrate availability, by increasing fatty acid oxidation, which would reduce liver TG content and substrate availability for VLDL production.
In summary, the major mechanism that explains the reduced fasting serum TGs following OM3FA treatment is reduced VLDL production, including a reduced num-ber and size of VLDL particles. Reduced VLDL secretion enhances the rate of conversion of VLDL particles to IDL and LDL particles.
Postprandial lipids and chylomicron production and removal
Several studies have investigated the effect of OM3FA supplementation on postprandial lipoprotein levels and metabolism. A study of the acute and chronic effects of 25 days’ OM3FA supplementation (30% of the total fat from fish oil or 3.5 g OM3FA per 1000 kcal) compared with test meals with mainly saturated fatty acids or mainly omega-6 fatty acids (OM6FAs) on postprandial
lipoprotein metabolism was performed in eight normo-lipidemic individuals [37]. It showed that both acute and chronic supplementation with OM3FAs reduced plasma levels of chylomicrons and postprandial TG levels to a greater extent than saturated fatty acid- or OM6FA-enriched meals. However, the mechanisms for the re-duced chylomicron levels associated with OM3FA sup-plementation were not investigated in this study.
The effects of OM3FA treatment on chylomicron clear-ance have been studied using different methods and the re-sults are consistent with an increased clearance of chylomicrons being the major mechanism that explains re-duced postprandial lipid levels [38, 39]. Thirty-three healthy individuals were treated in a randomized, double-blind, placebo-controlled study with either DHA or EPA ethyl es-ters for 4 weeks, and the effects were compared with those for safflower oil [38]. Both EPA and DHA treatment signifi-cantly increased removal of TGs in chylomicrons in the fed state but not in the fasted state. This finding indicates that OM3FA treatment increases the capacity for TG removal, but this increase in clearance capacity is mainly of import-ance when chylomicron levels are increased. Pre-heparin LPL activity increased following both DHA and EPA treat-ment [38], indicating that increased LPL activity could help to explain the increased clearance of postprandial TG. Ac-cordingly, the DHA and EPA treatments reduced chylo-micron diameter [38], indicating increased hydrolysis of TGs by LPL. In a follow-up analysis of the same study population, margination of TG-rich lipoproteins was mea-sured as an estimation of lipoprotein activity [39]. The in-creased margination of TG-rich lipoproteins with DHA and EPA supplementation indicated that the treatment in-creased either the amount of endothelial bound LPL or the affinity of lipoproteins to LPL [39]. In a recent study, the ef-fects of a hypocaloric diet plus 4 g daily OM3FA supple-mentation for 12 weeks on apoB48 kinetics after ingestion of a high-fat meal were investigated [40]. The clearance rate of apoB48 was increased by both the hypocaloric diet and the OM3FA treatment. Combined hypocaloric diet and OM3FA treatment as compared with hypocaloric diet alone reduced postprandial TG and apoB48 levels further, as well as reducing intestinal apoB48 production [40]. Thus, OM3FA treatment and weight reduction have an additive effect on chylomicron metabolism, postprandial TG and apoB48 levels.
production following OM3FA treatment is probably also of importance for enhanced chylomicron clearance, be-cause that results in fewer VLDL particles competing with chylomicrons for TG hydrolysis by LPL. Finally, OM3FA treatment also seems to reduce the production of chylomicron particles in individuals receiving a hypo-caloric diet.
Lipoprotein lipase
As described in the previous section, OM3FA treatment increases individuals’ TG-rich lipoprotein clearance cap-acity, probably by increasing LPL activity at the endothe-lial surface. Several mechanisms might explain the increased LPL activity. One possibility is that OM3FAs increase LPL expression. In a randomized, double-blind, placebo-controlled study investigating the effects of 6 g fish oil daily for 6 weeks on men with atherogenic dys-lipidemia, adipose tissue biopsies were taken 4–5 h post-breakfast [41]. Interestingly, LPL mRNA expression in adipose tissue increased in patients receiving fish oil supplementation. A potential mechanism for increased LPL mRNA expression is increased activation of the per-oxisome proliferator-activated receptor response element of the LPL gene, which has been demonstrated using a transfection assay [42]. However, the major regulation of LPL activity takes place post-translationally. Detailed studies on post-translational regulation, such as trans-port and dimerization of LPL by OM3FAs, are generally lacking. Comparing pre-heparin and post-heparin LPL activity showed consistently increased pre-heparin activ-ity, while post-heparin activity was unchanged by OM3FA treatment in most studies [38, 39, 43] but not all [41]. It is probable that neither pre-heparin nor post-heparin LPL activity accurately indicate the active en-dogenous pool of the protein on endothelial cells. Post-heparin LPL activity does not necessarily reflect physio-logically active enzyme because all enzymes are activated by heparin. Pheparin activity is a measure of LPL re-leased from endothelial cells, including endogenous plasma activators and inhibitors, and might therefore ex-plain why pre- rather than post-heparin LPL activity is better associated with margination of TG-rich lipopro-teins as an estimation of lipoprotein activity [39].
Apolipoproteins E, CII and CIII
The activity of LPL is regulated by apolipoproteins on TG-rich lipoproteins. ApoCII is an endogenous activator, while apoCIII is an endogenous inhibitor of LPL. Treat-ment with OM3FAs decreases plasma apoCIII levels [7, 44]. EPA alone does not change total plasma levels of apoCIII or apoCII, but decreases apoCII and apoCIII in VLDL [45]. However, there are few studies investigating if EPA has a specific effect on plasma levels and
distribution of apoCII and apoCIII on lipoprotein parti-cles in comparison with DHA.
Apart from inhibiting LPL, apoCIII in VLDLs reduces clearance of VLDL particles by inhibiting the effect of apoE on receptor-mediated uptake [46]. The major cause of reduced plasma VLDL levels is reduced VLDL pro-duction; therefore, it is unlikely that this effect of apoC-III plays a major role in the regulation of VLDL levels following treatment with OM3FAs. Experimental studies show that apoCIII enhances hepatic assembly and secre-tion of VLDL, and human kinetic studies have shown an association between apoCIII and VLDL production [47]. However, it remains to be shown clinically that apoCIII influences VLDL production. ApoCIII is a predictor of CV disease and reduced apoCIII levels may have direct beneficial effects on the vessel wall, such as by reducing its retention of LDL particles (LDL-apoCIII) [48–50]. Therefore, reduction of plasma apoCIII by OM3FAs is potentially positive from the perspective of CV risk, but it is unclear to what extent it contributes mechanistically to fasting TG levels following treatment with OM3FAs.
LDL levels, composition and particle size
In most studies investigating the effect of OM3FAs on LDL, there is no effect or a small increase in LDL-C levels. A consistent finding is an increase in mean LDL particle size, with a resulting shift towards those classi-fied as large, rather than small, LDL particles [7, 45, 51– 54]. Larger LDL particles may reduce CV risk because small dense LDL is associated with increased atherogeni-city [55]. A reduction in large VLDL1 production [30] is the most likely explanation for the larger LDL particles after treatment with OM3FAs. Other potential OM3FA-related mechanisms that may explain the changes in LDL particle size are less likely and include effects on hepatic lipase or cholesteryl ester transfer protein (CETP) activity. Hepatic lipase activity is typically un-changed in controlled studies investigating the effects of OM3FAs on patients with dyslipidemia [38, 43, 52]. In-consistent effects on CETP activity have been observed following treatment with OM3FAs: either no change [56], an increase [45] or a decrease [57] in activity.
Differential effects of DHA and EPA on LDL
One potential reason for the contradictory findings of OM3FA treatment on LDL-C levels could be an inter-action between OM3FAs and APOE genotype. ApoE is mainly associated with LDL and VLDL particles in the circulation. It is a high-affinity ligand for the LDL recep-tor as well as for the LDL receprecep-tor-related receprecep-tor and thereby facilitates the hepatic uptake of LDL and VLDL particles. There are three major isoforms of apoE: apoE2, apoE3 and apoE4, which differ in the amino acids present at positions 112 and 158 of the protein. ApoE3 is the most common isoform (70–80%), while the preva-lence of apoE4 is approximately 10–15% and that of apoE2 is approximately 5–10%.
ApoE4 is associated with a greater lipid response to dietary challenges [58]. Minihane et al. were the first to show that the effect of OM3FAs on LDL was dependent on APOE genotype [59]. Total cholesterol levels in-creased inAPOE4carriers and, although not statistically significant, LDL-C levels tended to increase more in APOE4 carriers than in APOE2 or APOE3 carriers fol-lowing OM3FA treatment. However, small dense LDL levels decreased similarly in the different APOE geno-types [59]. The interaction between DHA and EPA re-sponse and APOE genotype (APOE3/E3 vs APOE3/E4) was further investigated in a study comparing the effects of EPA-rich (3.3 g EPA) and DHA-rich (3.7 g DHA) oils, and a control oil, in a 3 × 4-week study separated by 10-week wash-out periods [60]. A differential response to DHA and EPA treatment was observed in APOE4 car-riers. DHA, but not EPA, treatment increased LDL-C in APOE4 carriers, while LDL-C tended to decrease in APOE3 carriers. A possible explanation for these find-ings is that VLDL2 particles fromAPOE4carriers reduce the uptake of LDL [60]. Thus, apoE4-containing VLDLs, in contrast to apoE3-containing VLDLs, compete with LDLs for uptake via the LDL receptor in hepatocytes, which could at least partly explain the higher LDL-C levels inAPOE4carriers compared withAPOE3carriers following DHA treatment. Another likely explanation for the increase in LDL-C inAPOE4 carriers is a greater conversion of VLDL to LDL, which has been shown to occur inAPOE4 carriers in kinetic studies [61]. Further-more, it has been shown thatAPOE4carriers respond to fish oil supplementation with a larger increase in LPL mRNA and post-heparin plasma LPL activity than non-APOE4 carriers [41]. This finding gives a plausible ex-planation for the greater conversion of VLDL to LDL in APOE4 carriers than in APOE3 carriers following OM3FA treatment.
Receptor-mediated LDL uptake
Other studies have investigated the uptake of LDL enriched in OM3FAs in hepatocytes. One study found no difference in the uptake of LDL enriched in OM3FAs
compared with LDL particles not enriched in OM3FAs [51]. Another study found that LDL particles enriched in OM3FAs depressed both LDL receptor mRNA levels and activity to a larger extent than did control LDL [62]. Expression of LDL receptor mRNA in peripheral blood, used as a surrogate marker for expression in the liver, was not influenced by OM3FA treatment in normolipi-demic individuals [51, 63], but decreased in hyperlipid-emic individuals [62, 64]. Proprotein convertase subtilisin/kexin type 9 (PCSK9) is mainly produced by the liver and found in the circulation. It regulates LDL-C levels by promoting degradation of the LDL receptor. Treatment with a DHA-enriched oil [65] or an OM3FA formulation containing both DHA and EPA [66] reduced plasma levels of PCSK9, but not LDL-C. Therefore, PCSK9 is unlikely to be of major importance for LDL turnover following treatment with OM3FA.
To summarize the effects of OM3FAs on LDLs, a small increase in LDL-C levels in hyperlipidemic pa-tients following treatment with OM3FAs could be ex-plained by several, not mutually exclusive, mechanisms. Reduced VLDL production increases the rate of conver-sion of VLDL particles to IDL and LDL particles. Evi-dence from clinical studies suggests that reduced hepatic production of VLDL, especially VLDL1, reduces the TG
Table 3Summary of key findings
•There is no clear difference between DHA and EPA with respect to
reducing fasting or postprandial TG levels.
•The major mechanism explaining reduced fasting serum TG associated
with OM3FA treatment is reduced VLDL production, including a reduced number and size of VLDL particles. The reduced VLDL production results in a faster conversion of VLDL particles to IDL and LDL.
•OM3FA supplementation partly corrects the underlying disorder
responsible for the atherogenic dyslipidemia in patients with type 2 diabetes by reducing hepatic production of VLDL1.
•Potential mechanisms for the inhibitory effect of OM3FAs on VLDL
production include improved hepatic insulin sensitivity, reduced liver fat and increased whole-body fatty acid oxidation.
•There is a relationship between DHA and the apoE4 isoform of apoE,
which results in an increased production of LDL from VLDL as well as in a reduced hepatic uptake of LDL via competition with apoE4-enriched VLDL2. Therefore, patients with the apoE4 variant could contribute to an overall increase in LDL-C in trials using OM3FA formulations containing DHA.
•OM3FAs increase LPL activity, likely by increased expression of the
gene and reflected as increased pre-heparin LPL activity. Increased LPL activity can explain the higher clearance rate of TG-rich lipoproteins postprandially, but normally not in the fasted state because LPL capacity is not rate-limiting when TG levels are not high.
•Treatment with OM3FAs reduces plasma levels of PCSK9, but does not
reduce LDL-C levels. Therefore, PCSK9 is unlikely to be of major import-ance for LDL-C levels following treatment with OM3FA.
Apoapolipoprotein,DHAdocosahexaenoic acid,EPAeicosapentaenoic acid,
IDLintermediate-density lipoprotein,LDLlow-density lipoprotein,LDL-C
low-density lipoprotein cholesterol,LPLlipoprotein lipase,OM3FAomega-3 fatty
acid,PCSK9proprotein convertase subtilisin/kexin type 9,TGtriglyceride,VLDL
load of LDL and therefore the LDL particles will con-tain more cholesterol (LDL-C) and become larger. In vitro results indicate that LDL enriched in OM3FAs could reduce LDL receptor activity to a larger extent than control LDL, which could contribute to in-creased LDL-C levels. Finally, there is a relationship between DHA and the apoE4 isoform, which results in increased production of LDL from VLDL as well as in reduced hepatic uptake of LDL via competition with apoE4-enriched VLDL2. Therefore, individual pa-tients with the apoE4 variant could contribute to an overall increase in LDL-C levels in trials using OM3FA formulations containing DHA.
Conclusions
In humans, EPA and DHA reduce plasma TG levels to a similar extent via two main mechanisms: 1) by reducing hepatic production of VLDL lipoproteins; and 2) by in-creasing postprandial LPL activity. Little is known re-garding the specific cellular and biochemical effects of EPA and DHA that are responsible for the TG-lowering mechanisms in humans. Key findings of this review are summarized in Table 3.
Abbreviations
ALA:Alpha-linolenic acid; Apo: Apolipoprotein; CAD: Coronary artery disease; CE: Cholesterol esters; CV: Cardiovascular; DHA: Docosahexaenoic acid; EPA: Eicosapentaenoic acid; FFA: Free fatty acid; HDL: High-density lipoprotein; IDL: Intermediate-density lipoprotein; LDL: Low-density lipoprotein; LDL-C: Low-density lipoprotein cholesterol; LPL: Lipoprotein lipase; MeSH: Medical Subject Heading; OM3FA: Omega-3 fatty acid; OM6FA: Omega-6 fatty acid; PCSK9: Proprotein convertase subtilisin/kexin type 9; PL: Phospholipid; PPAR: Peroxisome proliferator-activated receptor; TG: Triglyceride; VLDL: Very-low-density lipoprotein; VLDL-C: Very-low-density lipoprotein cholesterol; VLDL-TG: Very-low-density lipoprotein triglyceride
Acknowledgments
The systematic literature search was performed by Nesta Hughes, PhD, of Oxford PharmaGenesis, Oxford, UK, funded by AstraZeneca. Editorial support was provided by Richard Claes, PhD, of PharmaGenesis London, London, UK, and was funded by AstraZeneca.
Funding
This work was funded by AstraZeneca.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Authors’contributions
JO drafted the manuscript and EHC reviewed the content. Both authors revised the manuscript and approved the final version of the manuscript.
Authors’information
Not applicable.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
JO and EHC are employed by AstraZeneca.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Received: 23 March 2017 Accepted: 2 August 2017
References
1. Hegele RA, Ginsberg HN, Chapman MJ, Nordestgaard BG, Kuivenhoven JA, Averna M, et al. The polygenic nature of hypertriglyceridaemia: implications for definition, diagnosis, and management. Lancet Diabetes Endocrinol. 2014;2:655–66. 2. Nordestgaard BG, Varbo A. Triglycerides and cardiovascular disease. Lancet.
2014;384:626–35.
3. Berglund L, Brunzell JD, Goldberg AC, Goldberg IJ, Sacks F, Murad MH, et al. Evaluation and treatment of hypertriglyceridemia: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2012;97:2969–89. 4. Miller M, Stone NJ, Ballantyne C, Bittner V, Criqui MH, Ginsberg HN, et al.
Triglycerides and cardiovascular disease: a scientific statement from the American Heart Association. Circulation. 2011;123:2292–333.
5. Food and Drug Administration. Withdrawal of approval of indications related to the coadministration with statins in applications for niacin extended-release tablets and fenofibric acid delayed release capsules (April 18, 2016). Available from: https://s3.amazonaws.com/publicinspection. federalregister.gov/2016-08887.pdf. Accessed 14 Feb 2017.
6. Maki KC, Orloff DG, Nicholls SJ, Dunbar RL, Roth EM, Curcio D, et al. A highly bioavailable omega-3 free fatty acid formulation improves the
cardiovascular risk profile in high-risk, statin-treated patients with residual hypertriglyceridemia (the ESPRIT trial). Clin Ther. 2013;35:1400–11. e1–3 7. Maki KC, Bays HE, Dicklin MR, Johnson SL, Shabbout M. Effects of
prescription omega-3-acid ethyl esters, coadministered with atorvastatin, on circulating levels of lipoprotein particles, apolipoprotein CIII, and lipoprotein-associated phospholipase A2 mass in men and women with mixed dyslipidemia. J Clin Lipidol. 2011;5:483–92.
8. Siscovick DS, Barringer TA, Fretts AM, Wu JH, Lichtenstein AH, Costello RB, et al. Omega-3 polyunsaturated fatty acid (fish oil) supplementation and the prevention of clinical cardiovascular disease: a science advisory from the American Heart Association. Circulation. 2017;135:e867–e84.
9. Patel AA, Budoff MJ. Effects of eicosapentaenoic acid and docosahexaenoic acid on lipoproteins in hypertriglyceridemia. Curr Opin Endocrinol Diabetes Obes. 2016;23:145–9.
10. Davidson MH, Benes LB. The future of n-3 polyunsaturated fatty acid therapy. Curr Opin Lipidol. 2016;27:570–8.
11. de Roos B, Mavrommatis Y, Brouwer IA. Long-chain n-3 polyunsaturated fatty acids: new insights into mechanisms relating to inflammation and coronary heart disease. Br J Pharmacol. 2009;158:413–28.
12. Wei MY, Jacobson TA. Effects of eicosapentaenoic acid versus docosahexaenoic acid on serum lipids: a systematic review and meta-analysis. Curr Atheroscler Rep. 2011;13:474–83.
13. Harris WS, Bulchandani D. Why do omega-3 fatty acids lower serum triglycerides? Curr Opin Lipidol. 2006;17:387–93.
14. Davidson MH. Mechanisms for the hypotriglyceridemic effect of marine omega-3 fatty acids. Am J Cardiol. 2006;98:27i–33i.
15. Sanders TA, Sullivan DR, Reeve J, Thompson GR. Triglyceride-lowering effect of marine polyunsaturates in patients with hypertriglyceridemia.
Arteriosclerosis. 1985;5:459–65.
16. Vidgren HM, Agren JJ, Schwab U, Rissanen T, Hanninen O, Uusitupa MI. Incorporation of n-3 fatty acids into plasma lipid fractions, and erythrocyte membranes and platelets during dietary supplementation with fish, fish oil, and docosahexaenoic acid-rich oil among healthy young men. Lipids. 1997; 32:697–705.
17. Plourde M, Chouinard-Watkins R, Rioux-Perreault C, Fortier M, Dang MT, Allard MJ, et al. Kinetics of 13C-DHA before and during fish-oil supplementation in healthy older individuals. Am J Clin Nutr. 2014;100:105–12.
18. Egert S, Kannenberg F, Somoza V, Erbersdobler HF, Wahrburg U. Dietary alpha-linolenic acid, EPA, and DHA have differential effects on LDL fatty acid composition but similar effects on serum lipid profiles in normolipidemic humans. J Nutr. 2009;139:861–8.
20. Rambjor GS, Walen AI, Windsor SL, Harris WS. Eicosapentaenoic acid is primarily responsible for hypotriglyceridemic effect of fish oil in humans. Lipids. 1996;31(Suppl):S45–9.
21. Hansen JB, Grimsgaard S, Nilsen H, Nordoy A, Bonaa KH. Effects of highly purified eicosapentaenoic acid and docosahexaenoic acid on fatty acid absorption, incorporation into serum phospholipids and postprandial triglyceridemia. Lipids. 1998;33:131–8.
22. Mori TA, Burke V, Puddey IB, Watts GF, O'Neal DN, Best JD, et al. Purified eicosapentaenoic and docosahexaenoic acids have differential effects on serum lipids and lipoproteins, LDL particle size, glucose, and insulin in mildly hyperlipidemic men. Am J Clin Nutr. 2000;71:1085–94. 23. Buckley R, Shewring B, Turner R, Yaqoob P, Minihane AM. Circulating
triacylglycerol and apoE levels in response to EPA and docosahexaenoic acid supplementation in adult human subjects. Br J Nutr. 2004;92:477–83. 24. Tatsuno I, Saito Y, Kudou K, Ootake J. Efficacy and safety of TAK-085
compared with eicosapentaenoic acid in Japanese subjects with hypertriglyceridemia undergoing lifestyle modification: the omega-3 fatty acids randomized double-blind (ORD) study. J Clin Lipidol. 2013;7:199–207. 25. Schwellenbach LJ, Olson KL, McConnell KJ, Stolcpart RS, Nash JD, Merenich
JA, et al. The triglyceride-lowering effects of a modest dose of docosahexaenoic acid alone versus in combination with low dose eicosapentaenoic acid in patients with coronary artery disease and elevated triglycerides. J Am Coll Nutr. 2006;25:480–5.
26. Grimsgaard S, Bonaa KH, Hansen JB, Nordoy A. Highly purified eicosapentaenoic acid and docosahexaenoic acid in humans have similar triacylglycerol-lowering effects but divergent effects on serum fatty acids. Am J Clin Nutr. 1997;66:649–59.
27. Agren JJ, Hanninen O, Julkunen A, Fogelholm L, Vidgren H, Schwab U, et al. Fish diet, fish oil and docosahexaenoic acid rich oil lower fasting and postprandial plasma lipid levels. Eur J Clin Nutr. 1996;50:765–71. 28. Nestel PJ, Connor WE, Reardon MF, Connor S, Wong S, Boston R.
Suppression by diets rich in fish oil of very low density lipoprotein production in man. J Clin Invest. 1984;74:82–9.
29. Chan DC, Watts GF, Mori TA, Barrett PH, Redgrave TG, Beilin LJ. Randomized controlled trial of the effect of n-3 fatty acid supplementation on the metabolism of apolipoprotein B-100 and chylomicron remnants in men with visceral obesity. Am J Clin Nutr. 2003;77:300–7.
30. Ouguerram K, Maugeais C, Gardette J, Magot T, Krempf M. Effect of n-3 fatty acids on metabolism of apoB100-containing lipoprotein in type 2 diabetic subjects. Br J Nutr. 2006;96:100–6.
31. Lalia AZ, Johnson ML, Jensen MD, Hames KC, Port JD, Lanza IR. Effects of dietary n-3 fatty acids on hepatic and peripheral insulin sensitivity in insulin-resistant humans. Diabetes Care. 2015;38:1228–37.
32. Adiels M, Taskinen MR, Packard C, Caslake MJ, Soro-Paavonen A, Westerbacka J, et al. Overproduction of large VLDL particles is driven by increased liver fat content in man. Diabetologia. 2006;49:755–65. 33. Parker HM, Johnson NA, Burdon CA, Cohn JS, O'Connor HT, George J.
Omega-3 supplementation and non-alcoholic fatty liver disease: a systematic review and meta-analysis. J Hepatol. 2012;56:944–51. 34. Scorletti E, West AL, Bhatia L, Hoile SP, McCormick KG, Burdge GC, et al. Treating
liver fat and serum triglyceride levels in NAFLD, effects of PNPLA3 and TM6SF2 genotypes: Results from the WELCOME trial. J Hepatol. 2015;63:1476–83. 35. Couet C, Delarue J, Ritz P, Antoine JM, Lamisse F. Effect of dietary fish oil on
body fat mass and basal fat oxidation in healthy adults. Int J Obes Relat Metab Disord. 1997;21:637–43.
36. Mostad IL, Bjerve KS, Bjorgaas MR, Lydersen S, Grill V. Effects of n-3 fatty acids in subjects with type 2 diabetes: reduction of insulin sensitivity and time-dependent alteration from carbohydrate to fat oxidation. Am J Clin Nutr. 2006;84:540–50.
37. Weintraub MS, Zechner R, Brown A, Eisenberg S, Breslow JL. Dietary polyunsaturated fats of the W-6 and W-3 series reduce postprandial lipoprotein levels. Chronic and acute effects of fat saturation on postprandial lipoprotein metabolism. J Clin Invest. 1988;82:1884–93. 38. Park Y, Harris WS. Omega-3 fatty acid supplementation accelerates
chylomicron triglyceride clearance. J Lipid Res. 2003;44:455–63.
39. Park Y, Jones PG, Harris WS. Triacylglycerol-rich lipoprotein margination: a potential surrogate for whole-body lipoprotein lipase activity and effects of eicosapentaenoic and docosahexaenoic acids. Am J Clin Nutr. 2004;80:45–50.
40. Wong AT, Chan DC, Barrett PH, Adams LA, Watts GF. Effect of omega-3 fatty acid ethyl esters on apolipoprotein B-48 kinetics in obese subjects on a
weight-loss diet: a new tracer kinetic study in the postprandial state. J Clin Endocrinol Metab. 2014;99:E1427–35.
41. Khan S, Minihane AM, Talmud PJ, Wright JW, Murphy MC, Williams CM, et al. Dietary long-chain n-3 PUFAs increase LPL gene expression in adipose tissue of subjects with an atherogenic lipoprotein phenotype. J Lipid Res. 2002;43:979–85.
42. Rudkowska I, Caron-Dorval D, Verreault M, Couture P, Deshaies Y, Barbier O, et al. PPARalpha L162V polymorphism alters the potential of n-3 fatty acids to increase lipoprotein lipase activity. Mol Nutr Food Res. 2010;54:543–50. 43. Harris WS, Lu G, Rambjor GS, Walen AI, Ontko JA, Cheng Q, et al. Influence
of n-3 fatty acid supplementation on the endogenous activities of plasma lipases. Am J Clin Nutr. 1997;66:254–60.
44. Kastelein JJ, Maki KC, Susekov A, Ezhov M, Nordestgaard BG, Machielse BN, et al. Omega-3 free fatty acids for the treatment of severe
hypertriglyceridemia: the EpanoVa fOr Lowering Very high triglyceridEs (EVOLVE) trial. J Clin Lipidol. 2014;8:94–106.
45. Homma Y, Ohshima K, Yamaguchi H, Nakamura H, Araki G, Goto Y. Effects of eicosapentaenoic acid on plasma lipoprotein subfractions and activities of lecithin:cholesterol acyltransferase and lipid transfer protein. Atherosclerosis. 1991;91:145–53.
46. Zheng C, Khoo C, Furtado J, Sacks FM. Apolipoprotein C-III and the metabolic basis for hypertriglyceridemia and the dense low-density lipoprotein phenotype. Circulation. 2010;121:1722–34.
47. Yao Z, Wang Y. Apolipoprotein C-III and hepatic triglyceride-rich lipoprotein production. Curr Opin Lipidol. 2012;23:206–12.
48. Lee SJ, Campos H, Moye LA, Sacks FM. LDL containing apolipoprotein CIII is an independent risk factor for coronary events in diabetic patients. Arterioscler Thromb Vasc Biol. 2003;23:853–8.
49. Crosby J, Peloso GM, Auer PL, Crosslin DR, Stitziel NO, Lange LA, et al. Loss-of-function mutations in APOC3, triglycerides, and coronary disease. N Engl J Med. 2014;371:22–31.
50. Jorgensen AB, Frikke-Schmidt R, Nordestgaard BG, Tybjaerg-Hansen A. Loss-of-function mutations in APOC3 and risk of ischemic vascular disease. N Engl J Med. 2014;371:32–41.
51. Nenseter MS, Rustan AC, Lund-Katz S, Soyland E, Maelandsmo G, Phillips MC, et al. Effect of dietary supplementation with n-3 polyunsaturated fatty acids on physical properties and metabolism of low density lipoprotein in humans. Arterioscler Thromb. 1992;12:369–79.
52. Nordoy A, Hansen JB, Brox J, Svensson B. Effects of atorvastatin and omega-3 fatty acids on LDL subfractions and postprandial hyperlipemia in patients with combined hyperlipemia. Nutr Metab Cardiovasc Dis. 2001;11:7–16. 53. Tani S, Nagao K, Matsumoto M, Hirayama A. Highly purified
eicosapentaenoic acid may increase low-density lipoprotein particle size by improving triglyceride metabolism in patients with hypertriglyceridemia. Circ J. 2013;77:2349–57.
54. Woodman RJ, Mori TA, Burke V, Puddey IB, Watts GF, Best JD, et al. Docosahexaenoic acid but not eicosapentaenoic acid increases LDL particle size in treated hypertensive type 2 diabetic patients. Diabetes Care. 2003;26:253.
55. Dejager S, Bruckert E, Chapman MJ. Dense low density lipoprotein subspecies with diminished oxidative resistance predominate in combined hyperlipidemia. J Lipid Res. 1993;34:295–308.
56. Calabresi L, Villa B, Canavesi M, Sirtori CR, James RW, Bernini F, et al. An omega-3 polyunsaturated fatty acid concentrate increases plasma high-density lipoprotein 2 cholesterol and paraoxonase levels in patients with familial combined hyperlipidemia. Metabolism. 2004;53:153–8.
57. Nozaki S, Matsuzawa Y, Hirano K, Sakai N, Kubo M, Tarui S. Effects of purified eicosapentaenoic acid ethyl ester on plasma lipoproteins in primary hypercholesterolemia. Int J Vitam Nutr Res. 1992;62:256–60.
58. Hagberg JM, Wilund KR, Ferrell RE. APO E gene and gene-environment effects on plasma lipoprotein-lipid levels. Physiol Genomics. 2000;4:101–8. 59. Minihane AM, Khan S, Leigh-Firbank EC, Talmud P, Wright JW, Murphy
MC, et al. ApoE polymorphism and fish oil supplementation in subjects with an atherogenic lipoprotein phenotype. Arterioscler Thromb Vasc Biol. 2000;20:1990–7.
60. Olano-Martin E, Anil E, Caslake MJ, Packard CJ, Bedford D, Stewart G, et al. Contribution of apolipoprotein E genotype and docosahexaenoic acid to the LDL-cholesterol response to fish oil. Atherosclerosis. 2010;209:104–10. 61. Demant T, Bedford D, Packard CJ, Shepherd J. Influence of apolipoprotein E
62. Lindsey S, Pronczuk A, Hayes KC. Low density lipoprotein from humans supplemented with n-3 fatty acids depresses both LDL receptor activity and LDLr mRNA abundance in HepG2 cells. J Lipid Res. 1992;33:647–58. 63. Schmidt S, Willers J, Stahl F, Mutz KO, Scheper T, Hahn A, et al. Regulation
of lipid metabolism-related gene expression in whole blood cells of normo-and dyslipidemic men after fish oil supplementation. Lipids Health Dis. 2012;11:172.
64. Dawson K, Zhao L, Adkins Y, Vemuri M, Rodriguez RL, Gregg JP, et al. Modulation of blood cell gene expression by DHA supplementation in hypertriglyceridemic men. J Nutr Biochem. 2012;23:616–21.
65. Rodriguez-Perez C, Ramprasath VR, Pu S, Sabra A, Quirantes-Pine R, Segura-Carretero A, et al. Docosahexaenoic acid attenuates cardiovascular risk factors via a decline in proprotein convertase subtilisin/kexin type 9 (PCSK9) plasma levels. Lipids. 2016;51:75–83.
66. Graversen CB, Lundbye-Christensen S, Thomsen B, Christensen JH, Schmidt EB. Marine n-3 polyunsaturated fatty acids lower plasma proprotein convertase subtilisin kexin type 9 levels in pre- and postmenopausal women: a randomised study. Vasc Pharmacol. 2016;76:37–41.
• We accept pre-submission inquiries
• Our selector tool helps you to find the most relevant journal
• We provide round the clock customer support
• Convenient online submission
• Thorough peer review
• Inclusion in PubMed and all major indexing services
• Maximum visibility for your research
Submit your manuscript at www.biomedcentral.com/submit