General Public Expectation from the Communication Process with their Healthcare Providers
Full text
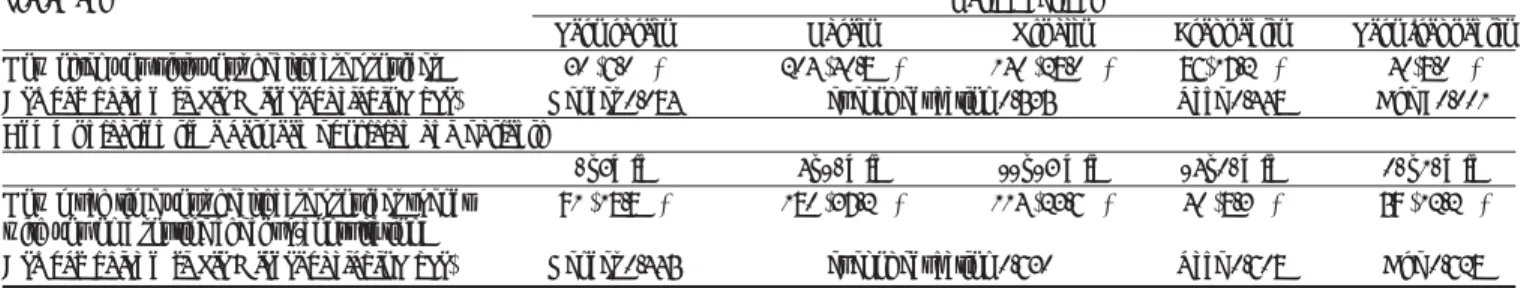
Figure
Related documents
○ If BP elevated, think primary aldosteronism, Cushing’s, renal artery stenosis, ○ If BP normal, think hypomagnesemia, severe hypoK, Bartter’s, NaHCO3,
On June 9, 2003, the Tax Discovery Bureau (Bureau) of the Idaho State Tax Commission issued a Notice of Deficiency Determination (NODD) to [Redacted] (taxpayers), proposing income
The current report, which is part of the Iranian Cataract Surgery Survey (ICSS), 31 reviewed some effective factors on hospitalization time in cataract surgery with a focus
In terms of mordant type and method, the use of CaO mordant with post and combined methods generated the best light fastness to light with a value of 4-5 (good
This essay asserts that to effectively degrade and ultimately destroy the Islamic State of Iraq and Syria (ISIS), and to topple the Bashar al-Assad’s regime, the international
Contradicting this explanation, however, are data that coronary blood flow is increased, not decreased, in patients with septic shock, and that elevated troponin levels in a majority