Original Article
doi 10.15171/ijep.2017.28
The Prevalence of Intestinal Parasites and
Associated Risk Factors Among Students of Jahrom
University of Medical Sciences
Hassan Rezanezhad1*, Mohammad Reza Shokouh2, Enayatollah Shadmand3, Nooshin Mohammadinezhad2,
Zahra Mokhtarian2, Arash Fallahi2, Hadi Rezaei Yazdi4, Abbas Ahmadi Vasmehjani4, Belal Armand3
1Department of Parasitology, Jahrom University of Medical Sciences, Jahrom, Iran
2Student Research Committee, School of Medicine, Jahrom University of Medical Sciences, Jahrom, Iran 3Department of Parasitology, School of Medicine, Jahrom University of Medical Sciences, Jahrom, Iran 4Department of Immunology and Microbiology, School of Medicine, Jahrom University of Medical Sciences,
Jahrom, Iran
Int J Enteric Pathog. 2017 November;5(4):121-126
http://enterpathog.abzums.ac.irCopyright © 2017 The Author(s); Published by Alborz University of Medical Sciences. This is an open-access article distributed under the
Background
Intestinal parasitic infections (IPIs) have been often
described as a significant public health and socioeconomic
problem in developing countries such as Iran though it
is globally pandemic.
1-3For this reason, always national
programs for fighting against the IPIs have been
important. Such programs help to find endemic level
of various intestinal parasites and might help to clarify
whether widespread or focal measures are needed for
control of the parasites. These infections affect many
individuals such as school children, young students
and infants.
4IPIs lead to symptomatic illness or states
of persistent diarrhea and problems with nourishment
and mental growth,
5,6of course, these parasites rarely
cause death. Lack of sanitary facilities, lack of access to
healthy water and poor hygiene, low socioeconomic
status, malnutrition, marginalization, high population
density, illiteracy and other factors give rise to parasitic
infections.
7,8These conditions threaten the population of
the country and the individuals that are more prone to
intestinal parasites. It also imposes an economic burden
on the community. As a result, the infection rate of these
parasites could show the socioeconomic status. Moreover,
the poor people of developing countries experience
Keywords: Prevalence, Intestinal parasites, Students, Jahrom
Abstract
Background: F: Parasitic infections, especially those caused by intestinal agents could affect social and personal hygiene and health; and to avoid the spread of pollution, monitoring the infectious sources is critical.
Objective: The aim of this study was to estimate the prevalence of intestinal parasites and identify factors associated with intestinal parasitic infections (IPIs) among students of Jahrom University of Medical Sciences during 2013-2014.
Materials and Methods: This study was carried out between September 2013 and February 2014. A total of 1293 stool samples were taken from 431 students and were examined by direct wet mounting and formalin-ether methods. A questionnaire for common risk factors was completed for each individual.
Results: Overall, the prevalence of IPIs was estimated to be 125 (29%) that was caused by both pathogenic and pathogenic intestinal parasites. Various species of pathogenic and non-pathogenic protozoa were detected: Entamoeba coli was the most common parasite (9.04%) followed by Blastocystis hominis (8.12%), and Giardia lamblia (4.64%). In the current study, 3.2% of students were infected with multiple parasites. A significant association was observed between the prevalence of intestinal parasitic infections and the type of accommodation (odds ratio [OR] =1. 5; 95% CI: 1.1; 1.9), parents’ educational level (OR=1. 5; 95% CI: 1.1; 1.9) and gender (OR=1. 5; 95% CI: 1.1; 1.9). No association was detected between the prevalence of infection and age, but a slightly positive prevalence was observed with aging (P=0.66). Conclusion: The data showed that intestinal parasites were slightly more prevalent than expected; that might be due to the interior sources of infection in college, such as carrier students. Hence, performing periodic stool screening of students is a necessity to promote the hygiene among the students.
*Corresponding Author:
Hassan Rezanezhad, Address: Motahhari Street, Department of Parasitology, Jahrom University of Medical Sciences, Jahrom, Iran. Tel: +98- 9173086197; Email: rezasiv@gmail.com
Received May 23, 2017; Revised August 20, 2017; Accepted September 3, 2017 Published Online September 23,
2017
International Journal of
Enteric
Pathogens
an infection cycle where malnutrition and repeated
infections lead to excess morbidity that can continue for
several generations.
9People of all ages may be affected
by the prevalence of parasitic infections; therefore, these
infections are not specific to special periods. Interestingly,
transmission possibilities of intestinal parasites increase
in areas with high population density, such as garrisons
and schools. Multiple intestinal parasites cause gastric
symptoms. For instance,
Giardia intestinalis
, the former
Giardia lamblia
, is considered as the most prevalent
protozoan parasite across the world which has affected
almost 200 000 000 people currently.
10,11Another usual
enteric protozoan is
Blastocystis hominis
whose parasitic
traits are still controversial.
7It is believed that over
2 000 000 000 people (nearly one-third of the human
population) are infected with intestinal parasites.
12,13Although, the mortality associated with IPIs is low, the
global number of related deaths is considerable, because
of the extent of the complications.
14Objectives
Consequently, determining the prevalence of the IPIs in
crowded populations, such as university students that are
in potential conditions for the transmission of infection to
each other is critical. Given that there is no information
on the prevalence of the intestinal parasites among the
students of universities in the south of Iran, this study
aimed to determine the prevalence and risk factors of
infection among students of Jahrom University of Medical
Sciences.
Materials and Methods
Sample Collection
This cross-sectional, population-based survey was
conducted from September 2013 to February 2014. The
study population consisted of 431 students of Jahrom
University of Medical Sciences, an institute in the southern
part of Iran. Simple random sampling method was used
to select the students. We randomly selected 431 male
and female students. After getting official permission
from the university administration, consent forms were
given to all the study students. Then, a questionnaire
based on sociodemographic data (sex, age, education and
socioeconomic level of parents, field of education, and
living place) was designed. After interviewing, 3 stool
samples were collected from each student in alternate
days.
Parasitological Examination
The samples were immediately transported to a
diagnostic laboratory. Then, the samples were examined
for gastrointestinal parasites. Initially, the slides were
prepared directly from each sample based on the wet
mount method using saline as well as iodine, and slides
were microscopically examined. Furthermore, all of the
samples were examined using the formol-ether method.
Briefly, 5 g of each sample was diluted in 7 mL of 5%
formaline and 3 mL ether, followed by centrifugation for
10 minutes.
Statistical Analysis
All analyses were done using SPSS for windows version
16.0 (SPSS, Chicago, IL, USA). Statistical difference for
each independent variable was identified using the
chi-square or student’s
t
test. The variables (risk factors)
and the prevalence of parasitic infection were compared
using logistic regression analysis with an odds ratio and a
confidence interval of 95%. A
P
value less than 0.05 were
regarded as statistically significant.
Results
Descriptive Characteristics
Demographic and socioeconomic data are shown in
Table 1. A total of 1293 stool specimens were examined
from 431 students in college (3 stool samples from each
student in alternate days). The age range was 19–24
years for all students and the mean age was 21.62 ± 2.34
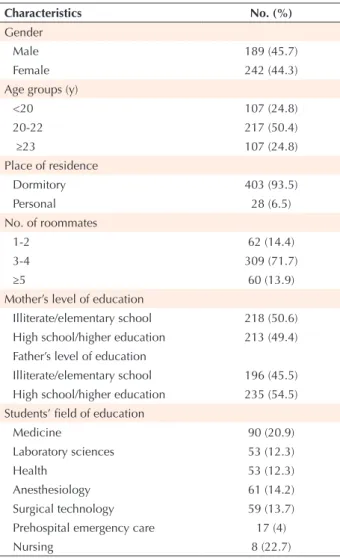
Table 1. Demographic Characteristics of Participants in the Project at Jahrom University of Medical Sciences, Southern Iran, 2013- 2014Characteristics No. (%)
Gender
Male 189 (45.7)
Female 242 (44.3)
Age groups (y)
<20 107 (24.8)
20-22 217 (50.4)
≥23 107 (24.8)
Place of residence
Dormitory 403 (93.5)
Personal 28 (6.5)
No. of roommates
1-2 62 (14.4)
3-4 309 (71.7)
≥5 60 (13.9)
Mother’s level of education
Illiterate/elementary school 218 (50.6) High school/higher education 213 (49.4) Father’s level of education
Illiterate/elementary school 196 (45.5) High school/higher education 235 (54.5) Students’ field of education
Medicine 90 (20.9)
Laboratory sciences 53 (12.3)
Health 53 (12.3)
Anesthesiology 61 (14.2)
Surgical technology 59 (13.7)
Prehospital emergency care 17 (4)
years. The students were classified based on age, and the
results showed that the distribution was 107 for students
aged <20 years (24.8%), 217 for those aged 20–22 years
(50.4%), and 107 for those aged ≥23 years (24.8%).
Prevalence of Intestinal Parasitic Infections
Our findings showed a 29% gastrointestinal parasitic
infection among 431 students. Overall, the prevalence
of infection with only 1 parasite species was 22.03%, the
prevalence of infection with 2 parasites was 2.73%, and the
prevalence of infection with 3 parasite species was 0.46%.
In general, 4 distinct intestinal parasite species were
observed. As it is shown in Table 2, the most common
protozoan species were
Entamoeba coli
(9.04% single,
and 1.8% double infection),
G. lamblia
(4.64% single,
and 1.99% double infection),
B. hominis
(8.12% single,
and 1.11% double infection), and
Enterobius vermicularis
(0.23% single, and 0.46% double infection). Moreover,
triple infection with
B. hominis
,
E. coli
and
G. lamblia
was
0.46%.
Probable Relationship of Independent Variables With
Intestinal Parasitic Infections
As it is declared in Table 3, there were several factors related
to intestinal parasitism including parents’ educational
level, place of residence, gender, and other risk factors.
The prevalence of intestinal parasitism in individuals
living in the dormitory was significantly higher than that
in students living in a personal house (odds ratio [OR] =
1.6; 95% CI: 1.8; 2.6,
P
= 0.01). The prevalence of intestinal
infections in individuals, whose fathers had elementary
level of education, was higher than that in students, whose
fathers had higher educational level, and this prevalence
was statically significant (OR
= 0.5; 95% CI: 0.3; 1.1,
P
= 0.02). Moreover, the rate of intestinal infections in
males was significantly higher than that in females (OR =
1.5; 95% CI: 1.1; 2.1,
P
= 0.01).
Discussion
In this study, we investigated the overall rate of IPIs and
the risk factors associated with IPIs among a number
of students of Jahrom University of Medical Sciences, a
medical institute in the southern part of Fars province,
Iran. The prevalence of intestinal parasites was estimated
to be 29%, from which the prevalence of helminth and
protozoan infections were 0.7% and 28.3%, respectively.
Various studies have consistently demonstrated the
widespread distribution of intestinal parasites in Iran
15-19and other countries among different populations,
20,21varying among different races and communities.
Differences in the rate of infection in various studies
could be due to the differences in target populations
and the years in which these surveys were performed.
Comparing our findings with those recently reported
for other populations of Iran, a slightly similar rate of IPI
was revealed. Based on data collected in studies carried
out in different parts of Iran, a 0%–5.8% prevalence of
intestinal helminth parasite infections
15,22,23was reported
that indicated contradictory result with the findings of the
present experiment on students (0.7%), which was lower
than other studies on students in other institutes of Iran
24and other countries.
25However, the current study was
of further importance in comparison with other similar
studies, because students of Jahrom University of Medical
Sciences were studying in interrelated fields with direct
correlations with universal health and this provided
them with higher awareness compared to other groups;
therefore, usual monitoring was found to be more critical.
When there are multiple intestinal infections such
as common IPIs (e.g. infections with
B. hominis
and
G.
lamblia
), we can hypothesize the fact that many species of
protozoa have probably the same route of transmission.
For example, human can be infected with
G. lamblia
by
water and possibly food, and like majority of prevalent
parasites, person-to-person transmission is believed to be
the primary mechanism of infection distribution in the
community of students. Moreover, due to poor personal
hygiene, some students may inadvertently be infected
through food sources.
26On the other hand, the relatively
high prevalence in these individuals could be explained
by poor sanitary conditions, contaminated water supplies,
and high density that in a recent study may be explained as
the result of low awareness among the students regarding
personal hygienic behaviors.
Our results also showed that gender of the students,
living area and parents’ level of education were significantly
correlated with IPI. In our study, the prevalence was
slightly higher in males (34.9%) than in females (24.4%),
Table 2. Prevalence of Single Parasitism and Polyparasitism Among431 Participants in the Project at Jahrom University of Medical Sciences, Southern Iran, 2013-2014
Intestinal Parasites Species Prevalence (%) Single Parasitism
Protozoa Entamoeba coli 9.04
Blastocystis hominis 8.12
Giardia lamblia 4.64
Subtotal protozoa (21.21.80%)
Helminths Enterobius vermicularis 0.23
Subtotal helminths 0.23
Polyparasitism
Double B. hominis + E. coli 0.41
E. coli + G. lamblia 1.16
B. hominis + G. lamblia 0.7
G. lamblia+ E. Vermicularis 0.23
E. coli + E. Vermicularis 0.23
Triple B. hominis + E.coli + G.lamblia 0.46 Subtotal mixed
that was statistically a significant difference (
P
= 0.01).
Several studies have reported a higher prevalence of
infection in males than females,
17,19,27whereas other
studies have indicated the opposite findings.
15,18,28In
the present study, infection was more common in the
20-22-year-old age group and was lower in the
20-year-old age group, but these data were not significant.
Interestingly, age is an important risk factor for IPIs; our
finding was similar to that reported in some previous
surveys
24,29and contradictory to some other reports.
9,15,16These differences could be explained by considering the
developed sanitary conditions and behaviors among
students, who were acquainted with proper hygienic
practices in their living places.
Several other risk factors were significantly associated
with IPIs. It was stated that parents’ level of education
was positively associated with the prevalence of pediatric
infection, which the present report confirmed it (
P
=0.02).
However, some studies reported a negative association
in this regard.
30A higher infection rate was observed
among the individuals whose fathers had only elementary
educational level; that was in agreement with the findings
of previous studies.
31-33This indicated that the level of
awareness of parents is directly intertwined with raising
the healthy students that were educated with educational
intervention as an effective means in reducing parasitic
prevalence.
The higher infection rate reported among students
living in dormitory showed a statistically significant
relationship, compared to those living in personal houses
and rental properties (
P
= 0.01). This finding was not in
line with that reported in previous surveys.
24,34This study
Table 3. Univariate Analysis of Factors Associated With Intestinal Parasitic Infection Among Participants in the Project at Jahrom University of Medical Sciences, Southern Iran, 2013-2014
Demographic
& Baseline Characteristics
Parasitic Positive No. (%)
Parasitic Negative
No. (%) OR 95% CI P Value
Gender 0.01
Male 66 (34.9) 183 (65.1)
Female 59 (24.4) 123 (75.6) 1.5 1.1; 2.1
Age groups (y) 0.66
<20 28 (26.2) 79 (73.8)
20-22 63 (29) 154 (71) 0.4 0.1; 0.9
≥23 34 (31.8) 73 (68.2) 0.9 1.3; 2.4
Living regions 0.01
Dormitory 111 (27.5) 292 (72.5)
Personal 14 (50) 14 (50) 1.6 1.8; 2.6
No of roommates 0.68
1-2 19 (30.6) 43 (69.4)
3-4 92 (29.1) 217 (70.2) 0.6 0.7; 1.6
≥5 14 (23.3) 46 (76.7) 1.3 1.9; 2.7
Mother’s level of education 0.09
Illiterate 22 (44.9) 27 (55.1)
Elementary school 27 (26.5) 75 (73.5) 1.7 0.9; 1.4
Tertiary school 20 (29.9) 47 (70.1) 2.2 1.7; 2.1
High school 34 (26) 97 (74) 3.1 2.4; 2.9
Academic 22 (26.8) 60 (73.2) 4.5 3.1; 4.1
Father’s level of education 0.02
Illiterate 20 (38.5) 32 (61.5)
Elementary school 34 (39.5) 52 (60.5) 0.5 0.3; 1.1
Tertiary school 12 (20.7) 46 (79.3) 1.4 1.2; 2.1
High school 27 (22.9) 91 (77.1) 2.7 2.9; 4.1
Academic 32 (27.4) 85 (72.6) 3.6 4.5; 5.8
Students’ field of education 0.39
Medicine 35 (38.9) 55 (61.1)
Laboratory sciences 13 (24.5) 40 (75.5) 1.12 0.87; 1.45
Health 13 (24.5) 40 (75.5) 2.4 2.1; 3.1
Anesthesiology 13 (21.3) 48 (78.7) 3.5 3.6; 4.1
Surgical technology 17 (28.8) 42 (71.2) 4.6 4.5; 5.2
Prehospital emergency 9 (52.9) 8 (47.1) 5.4 5.7; 6.5
also indicated that the high population density increased
the possibility of IPIs. However, our observation did
not suggest a statistically significant relationship
between parasitic infection and either the students’ field
of education (
P
= 0.39) or mothers’ educational level
(
P
= 0.09). Furthermore, the present study showed low
rates of helminths and relatively high rates of potentially
pathogenic protozoan infections, such as
G. lamblia
among students.
Conclusion
As a matter of fact, pathogenic IPIs among students of
medical universities should be frequently monitored
because of their direct relationship to the health of the
community; however, there has been little investigations
done on this group. Therefore, it is suggested that these
students take a set of personal hygienic programs and
behaviors. And in doing so, there exists a need to promote
the mass scale health conditions to raise awareness about
health and hygiene. However, further prospective studies
should be conducted before coming to any conclusion.
Authors’ ContributionsConcept studies and design: HR; Sample collection, administrative, technical, and material support: MRS, ES, NM, ZM, AF, BA; Analysis and interpretation of data: HR, AAV, HRY; Drafting of the manuscript: BA, AAV; and Study supervision: HR.
Ethical Approval
The approval of Ethics Committee of Jahrom University of Medical Sciences was obtained (code: Jums.REC.1393.001). Informed oral consent was also obtained from all the patients.
Conflict of Interest Disclosures
The authors declare that they have no conflict of interests. Financial Support
This work was financially supported by Jahrom University of Medical Sciences.
Acknowledgments
The authors would like to thank the students at Jahrom University of Medical Sciences who participated in this research project. This work was financially supported by Jahrom University of Medical Sciences (Jums.REC.1393.001).
References
1. Steketee RW. Pregnancy, nutrition and parasitic diseases. J Nutr. 2003;133(5 Suppl 2):1661s-1667s.
2. WHO. Control of Tropical Diseases. Geneva: WHO; 1998. 3. Rokni MB. The present status of human helminthic diseases
in Iran. Ann Trop Med Parasitol. 2008;102(4):283-295. doi:10.1179/136485908x300805
4. Saksirisampant W, Prownebon J, Kulkumthorn M, Yenthakam S, Janpla S, Nuchprayoon S. Prevalence of intestinal parasitic infections among school children in the central region of Thailand. J Med Assoc Thai. 2006;89(11):1928-1933. 5. Kim BJ, Ock MS, Chung DI, Yong TS, Lee KJ. The intestinal
parasite infection status of inhabitants in the Roxas city, The Philippines. Korean J Parasitol. 2003;41(2):113-115.
6. Garcia LS, Bruckner, DA. Diagnostic Medical Parasitology.
3rd ed. Washington, DC: ASM Press; 1997.
7. US CDC. DPDx: Laboratory Identification of Parasites of Public Health Concern. Atlanta: Center for Disease Control Prevention; 2006.
8. Cox G, Francis E, Julius P, Wakelin KD, eds. Parasitology; 9th ed. Philadelphia: WB Saunders; 1999.
9. Mehraj V, Hatcher J, Akhtar S, Rafique G, Beg MA. Prevalence and factors associated with intestinal parasitic infection among children in an urban slum of Karachi. PLoS One. 2008;3(11):e3680. doi:10.1371/journal.pone.0003680 10. Kain KC, Pillai DR. Common intestinal parasites. Current
Treatment Options in Infectious Diseases. 2003;5:207-217. 11. Minenoa T, Avery MA. Giardiasis: recent progress in
chemotherapy and drug development. Curr Pharm Des. 2003;9(11):841-855.
12. Schistosomiasis and soil-transmitted helminth infections--preliminary estimates of the number of children treated with albendazole or mebendazole. Wkly Epidemiol Rec. 2006;81(16):145-163.
13. Chan MS. The global burden of intestinal nematode infections--fifty years on. Parasitol Today. 1997;13(11):438-443. 14. WHO. Geographical distribution and useful facts and stats.
Geneva: WHO; 2006.
15. Daryani A, Sharif M, Nasrolahei M, Khalilian A, Mohammadi A, Barzegar G. Epidemiological survey of the prevalence of intestinal parasites among schoolchildren in Sari, northern Iran. Trans R Soc Trop Med Hyg. 2012;106(8):455-459. doi:10.1016/j.trstmh.2012.05.010
16. Sayyari AA, Imanzadeh F, Bagheri Yazdi SA, Karami H, Yaghoobi M. Prevalence of intestinal parasitic infections in the Islamic Republic of Iran. East Mediterr Health J. 2005;11(3):377-383.
17. Arani AS, Alaghehbandan R, Akhlaghi L, Shahi M, Lari AR. Prevalence of intestinal parasites in a population in south of Tehran, Iran. Rev Inst Med Trop Sao Paulo. 2008;50(3):145-149.
18. Haghighi A, Khorashad AS, Nazemalhosseini Mojarad E, Kazemi B, Rostami Nejad M, Rasti S. Frequency of enteric protozoan parasites among patients with gastrointestinal complaints in medical centers of Zahedan, Iran. Trans R Soc Trop Med Hyg. 2009;103(5):452-454. doi:10.1016/j. trstmh.2008.11.004.
19. Nasiri V, Esmailnia K, Karim G, Nasir M, Akhavan O. Intestinal parasitic infections among inhabitants of Karaj City, Tehran province, Iran in 2006-2008. Korean J Parasitol. 2009;47(3):265-268. doi:10.3347/kjp.2009.47.3.265 20. Omorodion OA, Isaac C, Nmorsi OP, Ogoya EM, Agholor
KN. Prevalence of Intestinal parasitic infection among tertiary institution students and pregnant women in south-south, Nigeria. J Microbiol Biotech Res. 2012;2(5):815-819. 21. Aksoy U, Akisu C, Bayram-Delibas S, Ozkoc S, Sahin S,
Usluca S. Demographic status and prevalence of intestinal parasitic infections in schoolchildren in Izmir, Turkey. Turk J Pediatr. 2007;49(3):278-282.
22. Rezaiian M, Jalalian M, Kia EB, Massoud J, Mahdavi M, Rokni MB. Relationship between Serum Ige and Intestinal Parasites. Iran J Public Health. 2004;33(1):18-21.
23. Asgari G, Nateghpour M, Rezaian M. Prevalence of intestinal parasites in the inhabitants of islam-- shahr district. Journal of School of Public Health and Institute of Public Health Research. 2003;1(3):67-74.
24. Arbabi M, Talari SA. Prevalence of intestinal parasites in students of Kashan University of Medical Sciences. J Ilam Univ Med Sci. 2003;12(44, 45):24-33. [Persian].
25. Adungo NI, Ondijo SO, Otieno LS. Intestinal parasitoses and other infections in a college community. East Afr Med J.
1991;68(1):52-56.
26. Bennett JE, Hill DR. Giardia lamblia. In: Mandell GL, Dolin R, ed. Principles and Practice of Infectious Diseases. 6th ed. New York: Churchill Livingstone; 2007:2888-2893.
27. Quihui L, Valencia ME, Crompton DW, et al. Role of the employment status and education of mothers in the prevalence of intestinal parasitic infections in Mexican rural schoolchildren. BMC Public Health. 2006;6:225. doi:10.1186/1471-2458-6-225
28. Sharif M, Daryani A, Asgarian F, Nasrolahei M. Intestinal parasitic infections among intellectual disability children in rehabilitation centers of northern Iran. Res Dev Disabil. 2010;31(4):924-928. doi:10.1016/j.ridd.2010.03.001 29. Yanagida J, Ishiyama S, Rai SK, Ono K. Study on Intestinal
Parasitosis among Public School Children in Kathmandu, Nepal. Bull Kobe Tokiwa Coll (Japan). 2004;26:55-8.
30. Uga S, Hoa NT, Thuan le K, Noda S, Fujimaki Y. Intestinal parasitic infections in schoolchildren in a suburban area of
Hanoi, Vietnam. Southeast Asian J Trop Med Public Health. 2005;36(6):1407-1411.
31. Nematian J, Nematian E, Gholamrezanezhad E, and Asgari AA. Prevalence of intestinal parasitic infections and their relation with socio-economic factors and hygienic habits in Tehran Primary School Students. Acta Tropica. 2004;92:179-186.
32. Ostan I, Kilimcioglu AA, Girginkardesler N, Ozyurt BC, Limoncu ME, Ok UZ. Health inequities: lower socio-economic conditions and higher incidences of intestinal parasites. BMC Public Health. 2007;7:342. doi:10.1186/1471-2458-7-342 33. Wordemann M, Polman K, Menocal Heredia LT, et al.
Prevalence and risk factors of intestinal parasites in Cuban children. Trop Med Int Health. 2006;11(12):1813-1820. doi:10.1111/j.1365-3156.2006.01745.x
34. Karrar ZA, Rahim FA. Prevalence and risk factors of parasitic infections among under-five Sudanese children: a community based study. East Afr Med J. 1995;72(2):103-109.